Common Pediatric Emergencies - excellence.creighton.edu · pneumothorax FB, severe asthma,...
Transcript of Common Pediatric Emergencies - excellence.creighton.edu · pneumothorax FB, severe asthma,...

9/4/2018
1
Common Pediatric
EmergenciesAngie Kratochvil-Stava, M.D.
September 7, 2018
Objectives
Evaluate and initiate treatment for critically ill infants
Evaluate and initiate treatment for critically ill children
NO DISCLOSURES

9/4/2018
2
Physical Exam
Physical Exam – Principles
Early identification is better than cardiorespiratory failure
Primary physiologic problem easier to identify early
Age appropriate responses
Steps in patient survey are same as for adults, but different specific signs of distress or physiologic instability

9/4/2018
3
Physical Exam – Rapid Assessment Appearance
Tone Moving vigorously? Resisting exam? Good muscle tone?
Interacting Alert? Reach out for objects? Readily distracted by sounds, people?
Consolable Consoled by caregiver?
Look/Gaze Fix on face? Or a “nobody home” stare?
Speech/cry Strong and spontaneous? Or weak, muffled?
Physical Exam – Rapid Assessment Work of Breathing
Abnormal airway sounds
Altered speech, stridor, wheezing, grunting
Abnormal positioning
Head bobbing, tripoding
Retractions Supraclavicular, intercostal, substernal retraction of chest wall
Flaring Nasal flaring

9/4/2018
4
Physical Exam – Rapid AssessmentPutting it Together
Normal appearance and increased work of breathing = respiratory distress
Abnormal appearance and increased work of breathing = respiratory failure
Abnormal appearance and abnormally decreased work of breathing = late respiratory failure
Physical Exam – Rapid AssessmentCirculation
Pallor White skin indicating lack of peripheral blood flow and an attempt to compensate for shock
Mottling Patchy skin discoloration with patches of cyanosis, due to vascular instability and loss of compensation
Cyanosis Bluish discoloration indicating shock and/or respiratory failure

9/4/2018
5
Physical Exam – Primary SurveyABCs – Airway and Breathing
Audible sounds – stridor, wheezing Loudness not correlated with severity
Respiratory Rate Caution with fever, anxiety, pain, excitement
Pulse oximetry
Physical Exam – Primary SurveyABCs – Interpreting Breath Sounds
Stridor upper airway obstruction croup, FB
Wheezing lower airway obstruction asthma, FB
Expiratory Grunting
Inadequate oxygenation pneumonia, pulm. contusion
Inspiratory Crackles
fluid/mucus/blood in airway
pneumonia, pulm. contusion
Absent Breath Sounds w/ inc. work of breathing
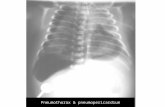
complete obstruction, pleural fluid, consolidation, pneumothorax
FB, severe asthma, hemothorax, pneumothorax

9/4/2018
6
Physical Exam – Primary SurveyABCs – Circulation
Color and skin perfusion Shock – compensated or decompensated Hypoxia? Infection? Head Trauma? Drugs?
Heart Rate – varies with age Blood Pressure – challenging in small kids Capillary Refill Pulse Quality End organ perfusion – kidneys, brain
Critical Newborn

9/4/2018
7
Critical Newborn
10-day-old full term infant presents with poor feeding and decreased alertness
Critical Newborn – Scenario 1
Pale, listless, weak cry
HR 180, RR 60, BP 78/50, Temp 103.5
Irritable with exam, no focal findings
Lungs: CTA, tachypnea, no retractions
Circulation: cap refill 1 second, warm and well-perfused

9/4/2018
8
Critical Newborn – Scenario 1Sepsis
Febrile newborns less than 28 days CBC, blood culture UA, urine culture LP, CSF culture IV Abxs – Ampicillin & Gentamicin/Cefotaxime
Most common bacteria: E. coli, GBS
Consider CXR HSV – HSV PCR of CSF and IV Acyclovir
ill-appearing, seizures, skin lesions
Critical Newborn – Scenario 1Sepsis
Febrile newborns 29-90 days: ill-appearing Essentially same as for <29 days old
Most common pathogens: S. pneumo, H. flu, N. meningiditis
IV Antibiotics Consider adding vancomycin
May choose ceftriaxone instead of cefotaxime
Use ampicillin in infants 29-60 days old

9/4/2018
9
Critical Newborn – Scenario 1Sepsis
Febrile newborns 29-90 days: well-appearing Minimum evaluation
CBC, blood culture, UA and urine culture
If term, uneventful birth, low-risk labs, and good follow-up, MAY observe as outpatient with 24 hour follow-up Low-risk labs
CBC - I:T <0.2, 5000-1500 WBC
UA - normal
If empiric antibiotics are used, must do LP May empirically use ceftriaxone or cefotaxime after LP
Consider CXR if respiratory symptoms
Critical Newborn – Scenario 1Sepsis – Difficult Situations
Unsuccessful LP Obtain blood and urine cultures
Less than 28 days, begin IV antibiotics at meningitis doses If positive blood or urine, reattempt LP
Treat as if meningitis if CSF pleocytosis
29-90 days, may observe

9/4/2018
10
Critical Newborn – Scenario 1Sepsis – Difficult Situations
Patient on Antibiotics Cannot be considered low-risk for serious
bacterial illness
Must admit for empiric IV antibiotics and obtain blood, urine, and CSF cultures
Critical Newborn – Scenario 1Sepsis – Difficult Situations
Concomitant Viral Infections Influenza positive – may omit LP if > 28 days and
low-risk lab results Do CBC, blood culture, UA, urine culture, CXR
Bronchiolitis – same as for Influenza

9/4/2018
11
Critical Newborn
10-day-old full term infant presents with poor feeding and decreased alertness
Critical Newborn – Scenario 2
Pale, lethargic, gray
HR 200, RR 60, BP 70/40, Temp 98.8
Lungs: retractions, grunting, crackles
Circulation: cool, 4-5 sec cap refill
Cardiac: 3/6 systolic ejection murmur
Liver: extends to pelvis

9/4/2018
12
Critical Newborn – Scenario 2Cardiogenic Shock – Management
ABCs and vascular access
Oxygen saturation (pre/postductal)
Hyperoxia challenge
ABG
Dopamine/Dobutamine if hypotensive
Judicious fluid resuscitation
Prostaglandin E1
Critical Newborn – Scenario 2Cardiogenic Shock – Management
Prostaglandin E1 Relaxes smooth muscle of ductus arteriosus
IV infusion: 0.05 mcg/kg/min
Side effects: tachycardia, hypotension, apnea
Must have secondary IV access
Must have intubation materials available

9/4/2018
13
Critical Newborn – Scenario 2Cardiogenic Shock – Management
After initial stabilization, consider CBC
Blood culture
Echocardiogram
EKG
Broad Spectrum IV antibiotics
Intubate and ventilate prior to transfer
Critical Newborn
10-day-old full term infant presents with poor feeding and decreased alertness

9/4/2018
14
Critical Newborn – Other Causes
Inborn Errors of Metabolism Glucose, electrolytes, ammonia, ABG
Non-accidental trauma A shaken baby often presents with poor feeding
as the only sign of abuse
Critical Pediatric Patients

9/4/2018
15
Pediatric Emergency – Scenario 1
3-year-old male with known asthma presents with sudden onset cough and “wheezing.” He has received albuterol via nebulizer every 3 hours x 3 without improvement.
Pediatric Emergency – Scenario 1
Sitting, leaning forward, coughing
HR 170, RR 56, BP 92/66, Temp 98.8
Lungs: rare breath sounds on right, left normal
Circulation: normal
CXR: severe atelectasis of right lung

9/4/2018
16
Pediatric Emergency – Scenario 1Foreign Body
Most common in kids < 3 years
Most common objects: peanuts, grapes, coins, small toys, jewelry, latex balloons, hot dogs
Majority aspirated into right lung
Suspicious when acute respiratory distress and no prodromal illness
Pediatric Emergency – Scenario 1Foreign Body – CXR
About 10% of FBs are radioopaque May see radiolucent objects if severe
obstruction Most common findings in lower airway FBA
Hyperinflated lung Atelectasis Mediastinal shift Pneumonia
Inspiratory/Expiratory Films

9/4/2018
17
www.radrounds.com/photo/1791588:Photo:16860?c
Pediatric Emergency – Scenario 2
7-month-old presents with 3 days of low-grade fever, vomiting, and diarrhea. She is limp and very sleepy.

9/4/2018
18
Pediatric Emergency – Scenario 2
Pale, limp, doesn’t cry
HR 200, RR 50, BP 80/50, Temp 100.8
Lungs: Rapid breathing, clear lungs
Circulation: cool peripherally, central pulses 1+, peripheral pulses not palpable, cap refill 5 seconds
GI: 3 stools during exam
Pediatric Emergency – Scenario 2Hypovolemic Shock
Shock – failure of the cardiovascular system to provide sufficient oxygen and other substrates to meet the metabolic demands of the tissues
Three Stages Compensated – normal BP, alert
Decompensated – dec. BP, dec. consciousness
Irreversible – bradycardia, apnea, hypotension

9/4/2018
19
Pediatric Emergency – Scenario 2Hypovolemic Shock – Management
IV/IO access No more than 3 IV attempts before IO
20 ml/kg crystalloid infused in < 20 minutes and reassess
Repeat 20 ml/kg fluid boluses
Use pulses, extremity temp, cap refill, level of alertness to guide therapy
Pediatric Emergency – Scenario 3
A 15-month-old infant presents with 2 days of rhinorrhea, cough, and low-grade fever. The child became acutely worse after going to bed and the parents now describe a “squeaking” noise and difficulty breathing.

9/4/2018
20
Pediatric Emergency – Scenario 3
Sitting on parents lap, suprasternal retractions, tachypnea, stridor
HR 160, RR 62, BP 102/76, Temp 101.2
Chest: Intercostal/suprasternal retractions
Lungs: Inspiratory stridor
Circulation: normal
Pediatric Emergency – Scenario 3Croup (Laryngotracheobronchitis)
Most common cause: parainfluenza virus
Most common ages: 3 months – 3 years
Harsh, barking/seal-like cough, hoarseness, and stridor following a few days of coryza and low-grade fever
Symptoms caused by upper airway edema, which narrows the subglottic region

9/4/2018
21
Pediatric Emergency – Scenario 3Croup – Management
Cool mist or humidified oxygen
Nebulized racemic epinephrine 0.05 ml/kg of 2.25% solution in 3 ml NS
Risk of rebound edema 30-90 minutes after
Dexamethasone 0.6 mg/kg PO/IM/IV (max 10 mg)
Inhaled Budesonide?
Prednisolone?
Pediatric Emergency – Scenario 4
5-year-old child presents with dry cough and increasing shortness of breath over the last 24 hours. He has been taking cetirizine for allergic rhinitis for the last two weeks. No fever.

9/4/2018
22
Pediatric Emergency 4 – Asthma Epidemiology – National
20.3 million asthmatics in U.S.
Morbidity/Mortality 1.8 million ER visits annually
500,000 hospitalizations
5000 deaths
Pediatric Emergency 4 – Asthma Epidemiology – National (Peds)
#1 chronic childhood illness in U.S.
Almost 5 million children with asthma
3rd ranking cause of pediatric hospitalization
4th most common cause for pediatric visits
14 million lost school days annually

9/4/2018
23
Pediatric Emergency – Scenario 4Asthma
What is asthma? Bronchial muscle spasm
Mucosal edema
Inflammation
Mucus plugging
Severity of wheezing does not always correlate with severity of airway obstruction
Peak flow of limited value in young patients
Pediatric Emergency – Scenario 4 Asthma - Pathophysiology
Sensitive airways that react to irritants that normal lungs can filter out
When irritants are inhaled swelling and inflammation occurs, making it hard
for air to pass in and out of lungs
the muscles around the airways constrict, making the airways even smaller
more thick, sticky mucus is made, making it hard for air to pass through

9/4/2018
24
Pediatric Emergency – Scenario 4 Asthma - Pathophysiology
The 4 main signs of asthma Dry, hacking cough
Wheezing
Chest tightness
Shortness of breath
Pediatric Emergency – Scenario 4Asthma – Management
Relieve bronchial muscle constriction Rescue/Quick medications
SABA – nebulizer or inhaler w/spacer
Oxygen
Decrease inflammation/swelling/mucus Maintenance/Controller medications
Inhaled steroids
Leukotriene receptor antagonist
Allergy treatments

9/4/2018
25
Pediatric Emergency – Scenario 4Asthma – Quick Relief
Used in ALL asthma
Also called reliever/rescue medications
Quickly decrease muscle constriction
Medicine is breathed into the lungs using an inhaler (with spacer) or nebulizer Spacer with mask for younger children
Levalbuterol has no proven benefit over albuterol
Pediatric Emergency – Scenario 4Asthma – Management – Spacers
1. Shake the inhaler at least 5 times and take cap off.2. Place the spacer on the end of the inhaler.3. Relax and breathe out. Hold your head looking straight ahead, not
looking down.4. Put the spacer in your mouth, on top of your tongue.
Close your lips around the spacer.5. Press down on the inhaler.
This will put 1 puff of medicine into the spacer.
6. Breathe in slowly and deeply until your lungs are full, five times.
7. Wait at least 1 minute. Then repeat the above steps.

9/4/2018
26
Pediatric Emergency – Scenario 4Asthma – Controller MedicationsUsed in persistent asthmaDo not stop an asthma episodeShould be taken every day, even when
children are feeling wellAct over a long period of time, taking weeks to
reach effectiveness
Tell families to think of them as vitamins protecting children from serious illnessNot addicitve, rare side effects
Pediatric Emergency – Scenario 4Asthma – Management
Relieve bronchospasm Oxygen (bronchodilator)
Albuterol - 0.15 mg/kg in 3 ml NS (max 5 mg) Short acting beta-2 agonist
May repeat every 20 minutes x 3, then minimum 30 minutes intervals or continuous
Decrease airway inflammation Prednisone 2 mg/kg PO/IM/IV (max 60 mg)
If no improvement after one dose albuterol

9/4/2018
27
Pediatric Emergency – Scenario 4Asthma – Management
Moderate-Severe, consider adding: Ipratropium with first three albuterol treatments
Anticholinergic – bronchodilation through smooth muscle relaxation
250 mcg/dose if < 20 kg, 500 if > 20 kg
Only proven useful in ER setting
IV magnesium sulfate smooth muscle relaxant
75 mg/kg (max 2.5 grams) over 20 minutes
Pediatric Emergency – Scenario 4Asthma – Management
Moderate-Severe, consider adding: Parenteral beta 2 agonists
Terbutaline SC/IM 0.01 mg/kg dose (max 0.4 mg/dose) May repeat q 20 minutes x 3
Epinephrine SC/IM 0.01 mg/kg dose (max 0.4 mg/dose) May repeat q 20 minutes x 3, then every 2-6 hours
Terbutaline IV Bolus 10 mcg/kg over 10 min, then 0.3-0.5 mcg/kg/min,
inc. by 0.5 mcg/kg/min q 30 min (max 5 mcg/kg/min)

9/4/2018
28
Pediatric Emergency – Scenario 5
2-month-old former 35 week premature infant presents with few days of rhinorrhea and mild cough and now having difficulty breathing. Infant has felt warm and is not eating well.
Pediatric Emergency – Scenario 5
Anxious appearing infant in respiratory distress
HR 180, RR 85, BP 80/40, Temp 101.6
Chest: moderate retractions, occasional grunting
Lungs: scattered wheezes, fine crackles
Circulation: warm, well-perfused

9/4/2018
29
Pediatric Emergency – Scenario 5Bronchiolitis
Etiologies: RSV, human metapneumovirus
Causes small airway obstruction
Most severe in children < 2 years
Prodrome: cough, coryza, low-grade fever
Apnea in very young infants
CXR: hyperinflation w/patchy infiltrate and atelectasis
Pediatric Emergency – Scenario 5Bronchiolitis – Management
Treatment – What Works Oxygen
IV fluids
Patience and Time

9/4/2018
30
Pediatric Emergency – Scenario 5Bronchiolitis – Management
Treatment – What Might Work Bronchodilators (albuterol)
Trial acutely, small percentage may respond
Racemic Epinephrine More helpful than albuterol, especially in ED
Hypertonic Saline Potentially reduces airway edema and mucus
plugging
Surfactant in ICU patients
Pediatric Emergency – Scenario 5Bronchiolitis – Management
Treatment – What Doesn’t Work Chest Physiotherapy
Steroids
Antibiotics
Ribavirin

9/4/2018
31
Pediatric Emergency – Scenario 6
A 4-month-old infant who started coughing while sitting in an infant seat. She then had a large emesis, turned “white,” and had a long pause in her breathing.
Pediatric Emergency – Scenario 6
Well-appearing, alert infant, sitting on mom’s lap
HR 120, RR 32, BP 86/48, Temp 98.9
Chest: Breathing non-labored, symmetric
Lungs: Clear
Circulation: warm, well-perfused

9/4/2018
32
Pediatric Emergency – Scenario 6ALTE (Apparent/Acute Life-Threatening Event)
An episode that is frightening to the observer and is characterized by some combination of apnea, color change, change in tone, choking, or gagging
No ICD-9 code for ALTE
0.05-1% of infants
Pediatric Emergency – Scenario 6ALTE
Etiology found in half with H & P and focused evaluation Differential diagnosis is LONG
Most common GERD with laryngospasm (30%)
Neuro – breath-holding, seizure (20%)
Infection

9/4/2018
33
Pediatric Emergency – Scenario 6ALTE
Retrospective study of 471 patients Characterized long and short term risk for death,
child abuse, abnormal neurological outcomes
11% were ultimately victims of child abuse No risk factors identified Other studies, 1-2.5% had abusive head trauma
Risk factors: vomiting, irritability, 911 call
5% with adverse neurologic outcome Risk factors: family history of seizure
Pediatric Emergency – Scenario 6ALTE - Recommendations
No intervention? Monitor at home? Admit? Admit with A/B monitor if more than one episode
or history of physiologic compromise
Focused work-up based on H & P Was it truly life-threatening? Frightening?
If “real” and no clear explanation, consider: CBC, UA, BMP, EKG, CXR, toxicology screen
Inpatient neurologic evaluation low yield Don’t forget child abuse!

9/4/2018
34
Questions