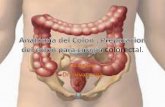
Colon ap 7-21-10
-
Upload
haripriya-uppala -
Category
Technology
-
view
631 -
download
0
Transcript of Colon ap 7-21-10

7/21/2010
Colon Anatomy and Physiology

Cecum
Blind pouch below the entrance of the ileum Almost entirely invested in peritoneum Mobility limited by small mesocecum Ileum enters posteromedially
Angulation maintained by superior and inferior ileocecal ligaments
Three pericecal recesses or fossae Superior, inferior, retrocecal

Ileocecal valve
Valve de Bauhin Ileocecal sphincter
Slight thickening of muscular layer of terminal ileum Relaxes in response to food in the stomach
Competence Regulates ileal emptying Angulation plays a role in prevention of reflux

Appendix
Vermiform appendix Elongated diverticulum from posteromedial cecum
about 3.0 cm below ileocecal junction Mean length 8-10cm, approx 5 mm diameter Mesoappendix contains vessels 85-95% posteromedial toward ileum
Also can be retrocecal, pelvic, subcecal, pre-ileal, and retro-ileal

Ascending colon
15 cm long, from ileocecal junction to right colic or hepatic flexure
Retroperitoneal Covered anteriorly and on both sides, not posteriorly
Jackson’s membrane Adhesions between right abd wall and anterior colon
Hepatic flexure supported by nephrocolic ligament

Transverse colon
45 cm long Intraperitoneal Greater omentum fused on anterosuperior aspect Splenic flexure angle attached to diaphragm by
phrenocolic ligament More acute, higher, and more deeply situated than hepatic
flexure

Descending colon
25 cm Retroperitoneal Narrower and more dorsally situated than ascending
colon

Sigmoid colon
35-40 cm long Mobile, omega shaped loop Intraperitoneal Mesosigmoid attached to pelvic walls in inverted V,
resting in intersigmoid fossa Left ureter immediately below, crossed anteriorly by spermatic,
left colic and sigmoid vessels

Rectosigmoid junction
Last 5-8 cm of sigmoid and upper 5 cm of rectum Tinea libera and tinea omentalis fuse and where
haustra and mesocolon terminate 6-7 cm below sacral promontory
Narrowest portion of large intestine Functional sphincter

Blood supply
Superior mesenteric artery (midgut) Supplies cecum, appendix, ascending colon, proximal 2/3 of
transverse colon Middle, right and ileocolic branches
Inferior mesenteric artery (hindgut) Supplies distal 1/3 of transverse, descending, sigmoid Left colic and 2-6 sigmoidal arteries Becomes superior hemorrhoidal after crosses left common iliac
Venous drainage follows arterial supply

Collateral circulation
Marginal artery of Drummond Griffiths’ critical point Sudeck’s critical point Arc of Riolan Meandering mesenteric artery
Presence indicates severe stenosis of SMA or IMA

Colonic Physiology
Not an essential organ, but has a major role in maintaining health of the body
Extrensic nervous component from autonomic system Affects motor and sensory Parasympathetics are excitatory o Motor component through acetylcholine and tachykinins (substance
P) o Visceral sensory function
Sympathetic input is inhibitory to colonic peristalsis Excitatory to sphincters Inhibitory to non-sphincteric muscle Mediated by alpha-2 adrenergic receptors Agonists relax the tone

Colonic Physiology
Intrinsic nervous component is enteric nervous system Mediate reflex behavior independent from brain or
spinal cord Neuronal plexuses in myenteric and
submucosal/mucosal layers Myenteric plexus regulates smooth muscle function Submucosal plexus modulates mucosal ion transport and absorptive
functions
Acetylcholine, opioids, norepinephrine, serotonin, somatostatin, cholecystokinin, substance P, VIP, neuropeptide Y, and nitric oxide are important neurotransmitters

Salvage, Metabolism, and Storage
More than 400 different species of bacteria, most anaerobes
Feed on mucous, residual proteins, complex carbs Fermentation of carbs produces short chain fatty
acids Acetate, propionate, butyrate Occurs in right and proximal transverse colon
Proteins are broken down into SCFAs, branched chain FAs, ammonia, amines, phenols, and indols Become a nitrogen source for bacterial growth

Short Chain Fatty Acids
Butyrate Least amount produced Primary energy source for colonocytes Role in cell proliferation and differentiation Important in absorption of water and salt
Propionate Combines with 3 carbon compounds in liver for gluconeogenesis
Acetate Most abundantly produced Used to synthesize longer-chain FAs by liver Energy source for muscle

Salvage, Metabolism, and Storage
Proximal colon More saccular Acts as a reservoir Fluid moves through quickly, solid material slower Principal site for SCFA production
Distal colon More tubular Acts as a conduit Protein degredation
Haustral segmentation facilitates mixing, retention of luminal material, formation of solid stool

Transport of Electrolytes
Presented 1-2 L of water/day Absorbs 90% Only 100-150 mL eliminated in stool Can increase to 5-6 L/day when challenged
Important in recovery of salts Absorbs sodium and chloride
Sodium absorbed against concentration and electrical gradients Secretes bicarb and potassium

Transport of Electrolytes
Chloride is exchanged for bicarb Secreted into lumen to neutralize organic acids produced Occurs at luminal border of mucosal cells
Potassium movement is passive secondary to active absorption of sodium Active secretion may occur in distal colon Coupled with potassium in bacteria and mucous in stool, may
explain relatively high concentration of K+ in stool
Secretes urea Metabolized to ammonia Majority is absorbed passively

Transport of Electrolytes
Aldosterone enhances fluid and sodium absorption SCFAs are principle ions and stimulate sodium
absorption Absorption of water and salt occurs primarily in
ascending and transverse colon Active transport of sodium creates osmotic gradient and water
passively follows
Surface mucosal cells responsible for absorption Crypt cells involved in fluid secretion

Peristalsis
Waves of alternate contraction and relaxation that propel contents, contractile events
No cyclic motility Segmental contractions, either single or bursts of
contractions, rhythmic or arrhythmic Propagated contractions Allows slow transit and opportunity for contents to maximally
contact mucosal surface
Low-amplitude propagated contraction (LAPC) Long spike bursts Related to meals and sleep-wake cycles, passage of flatus

Peristalsis
High-amplitude propagated contraction (HAPC) Migrating long spike bursts Equivalent of mass movement Move large amounts of stool toward the anus Approx 5 times daily
Haustra are static and partially occluding Disappear with peristalsis Correspond with mass movement

Cellular Basis for Motility
Circular muscle Longitudinal muscle Interstitial cells of Cajal (ICC)
Pacemaker cells Regulation of motility Electrically active, create ion currents Basal pathway for slow waves between circular and
longitudinal muscle
All electrical activity dependent on stimulation by stretch or chemical mediation
Critical volumes of distention needed for propulsion

Colonic Motility
Exhibits circadian rhythm Decreased activity at night Increase in activity after waking and after meals (HAPCs)
Regional differences in pressure activity Transverse and descending have more activity during the day Rectosigmoid most active at night Women have less activity in transverse and descending colon
Stress influences function Induces prolonged propagated contractions

Colonic Motility
Right and transverse colon are major sites of solid stool storage Remains in right colon for extended periods to allow for
mixing
Gastrocolic reflex Immediate increase in tonic contraction of proximal colon
after a meal Unknown mediator
CCK Well know colonic stimulator Increases colonic spike activity in a dose-dependent manner Possible postprandial stimulator

Defecation
Process begins up to an hour before—a preexpulsive phase Increased propagating and nonpropagating activity in the
entire colon May propel stool to distal colon and stimulate afferent nerves
15 min before defecation, second phase increases sensation of the urge to defecate through propagating sequences Associated with at least one high amplitude HAPC

Modulation of Visceral Sensation
Enteroenteric reflexes mediated by spinal cord Alters smooth muscle tone, increasing or decreasing activation of nerve
endings in gut or mesentery
Direct central modulation of pain Through descending noradrenergic and serotonergic pathways from the
brainstem
Referred pain Overlap of input from visceral structures perceived as being from somatic
structures Same embryonic dermatome
Visceral sensation can relay via collaterals to reticular formation and thalamus Changes in appetite, affect, pulse, blood pressure through autonomic,
hypothalamic, and limbic systems

Constipation
Infrequent or hard to pass stools Dietary, pharmacologic, systemic, or local causes Seen more frequently in sedentary people Idiopathic slow transit constipation
Altered colonic motor response to eating, impaired or decreased HAPCs
Reduced or absent propulsive activity Not helped by fiber
IBS 5-HT4 receptor agonists and CCK-1 agonists

Obstructed Defecation
Usually due to abnormalities in pelvic function Failure of puborectalis to relax with defecation, rectocele,
perineal descent, etc Marker studies show collection in left colon Associated with total colonic inertia
Sigmoidocele Colonic source Relieved and treated with sigmoid resection

Ogilvie’s Syndrome
Acute colonic pseudoobstruction Parasympathetics have decreased function with
increased sympathetic input Cecum can become extremely dilated Treatment is Gastrografin enema to R/O distal
obstruction Can also treat with neostigmine
Cholinesterase inhibitor Allows more available acetylcholine for neurotransmission in
parasympathetic system to promote contractility

Irritable Bowel Syndrome
Altered bowel habits associated with pain constipation-predominant, diarrhea-predominant,
or mixed type Unclear pathophysiology Men—diarrhea predominates Antispasmodics (anticholinergics), low-dose TCAs,
5-HT3 antagonists