CHAPTER - 7 STUDIES AT KLE UNIVERSITY...
Transcript of CHAPTER - 7 STUDIES AT KLE UNIVERSITY...
-
SECTION-II 7 : Studies at KLEUH
56
CHAPTER - 7
STUDIES AT KLE UNIVERSITY HOSPITAL
After ensuring that the equipments and accessories were available in adequate
number we practiced and acquired the skill of attaching the probes quickly without
disturbing the routine care of the newborn. Two nursing staff were identified and were
also trained in this protocol. Further they also received training in maintenance of
equipment, ensuring that good signal and waveform were being displayed on the
screen, and that the probes were attached properly through out the monitoring in the
DR, during transfer from DR to PNW and later in the PNW. We then decided to
embark on our study.
To begin with, we studied the time motion of mother in labor and Newborn:
Mother was shifted to the delivery room when in established labor. She was
monitored by the attending resident and nurse. CTG monitoring was done if
necessary. Pediatric resident was also simultaneously informed about the progress of
the patient. Delivery was conducted by the senior resident; consultant was called in
presence of any complications or when there was need for assisted delivery.
Newborn resuscitation team comprised of a registrar, a resident and a nurse
trained in NRP 2006protocol.[134]
The investigator and resuscitation team worked
independently during the study period but the team was not blinded to the data that
was monitored. Routinely, the team provided required care to the newborn under
radiant warmer, dried and wrapped the baby in the piece of cloth brought by the
relatives which was either from thin dhoti, cotton saree (40%), polyester or any other
synthetic material (60%). The newborn infant was wrapped in three folds which
covered the head partially. Diapers and head caps were not used. The baby was kept
-
SECTION-II 7 : Studies at KLEUH
57
under warmer till mother was ready to receive the baby for breast feeding. This period
varied from 40 minutes to one and half hour depending on the time taken for
stabilization of the mother. A clinical examination to rule out any obvious life
threatening anomalies was performed by the resident on each baby. Injection Vitamin
K 1 mg intramuscular was given to all the babies.
Baby was encouraged to suckle at the breast when kept with the mother
wrapped in the cloth and was monitored for signs of respiratory distress and proper
attachment at the breast. The baby and mother were kept in the DR for minimum 2
hours (2 1/2-4 hours average 3 hours) before they were shifted to the postnatal ward.
All infants weighing ≤ 2200 grams were shifted to the Kangaroo mother care ward.
Stable infants weighing >2200 grams were shifted to the PNW with the mother.
It is the norm in the Indian family that each mother is accompanied by an
experienced relative (her mother, sister or aunt) who takes over the care of the
newborn allowing the mother to take rest. This was followed in our community also.
All the babies were exclusively breast fed on demand. Generally primi mothers
preferred to feed the baby in lying down position which allowed them to take rest.
Experienced mothers breast fed the baby sitting up by placing the baby on the lap.
During the study period the PNW in the hospital was a general 60 bed, open
ward, for mothers and newborns with no air conditioning or central heating system.
Windows of the unit were open or closed depending on the weather conditions. As
per local practice, infants did not wear a cap, shirt or socks. Infants were co-bedded
with mother. Infants were wrapped in the cloth, which partially covered their head
and were covered with same blanket as that of the mother. All the infants were
exclusively breast fed on demand, and breast-feeding was not interrupted during the
study. Change of wet and soiled clothing was done as needed.
-
SECTION-II 7 : Studies at KLEUH
58
Routine monitoring of the baby was done by the nurse in PNW and
encouraged exclusive breast feeding.
The hospital having accepted Baby friendly
initiative, it was the hospital policy not to
advocate top milk for well term normal
newborns in the postnatal ward. Babies did
not receive bath during the hospital stay.
The baby was discharged from the
postnatal ward along with the mother in 3-5
days.
7.1. METHODOLOGY
We carried out feasibility study on 5 infants delivered at KLEUH (TCH) to
test the study protocol and to get acquainted with the use of equipments. After
delivery, the newborn infant was received in a tray covered with warm hospital cloth
and time of birth and time taken to clamp the cord was noted. After cutting the cord
the infant was placed on the resuscitation trolley under the radiant warmer and care
was given as per NRP 2006 guidelines by the team assigned for resuscitation. The
monitoring was initiated by the investigating team as described under
methodology.(Fig 7.1)
Monitoring of other Physiologic Parameters
After the oxygen sensor and temperature probes were securely attached to the
baby we attached disposable neonatal BP cuff 3cm × 9cm for non invasive blood
pressure monitoring to the left upper limb. After application of the cuff, baby was
Fig 7.1. Monitoring of the newborn under
warmer. BP cuff is attached to the left
arm.Temperature probes are placed on
abdomen & right foot. SpO2 sensor is
attached to right palm.
-
SECTION-II 7 : Studies at KLEUH
59
settled by gentle stroking or allowing sucking at his/her fingers. The left hand was
gently placed in semi flexed to extended position and BP was recorded. If no
recording was obtained in 2 attempts at 2 minutes interval due to movements of the
baby then no further attempts were made till baby settled down. The study protocol
was planned to monitor blood pressure every 15 minutes starting from 5 minutes of
birth for first one hour and then every four hours till 12 hours from birth. This was not
possible when baby was feeding or crying and hence we obtained NIBP recordings
whenever feasible with standard protocol.
The baby was assessed for following clinical parameters regularly at 5, 15, 30
minutes, one hour, 2-4 hours, 6-8 hours & 10-12 hours. Intervals were chosen not to
disturb the baby and mother while resting. All the details were entered in the clinical
assessment protocol which was prepared for the study. (Annexure-III-A)
1. Color was noted over the tongue, palms and soles and marked as pink or blue.
Any color other than pink (pale, dusky) was recorded as blue. The recognition of
color was done by the investigator and/or by another Pediatrician who had
agreement on the labeling it as pink or blue after practicing over 10 babies.
Simultaneous SpO2 was recorded in the patient chart.
2. Temperature was assessed by placing the dorsum of
hand over the trunk, palms and soles and was recorded
as cold or warm. Simultaneous abdominal and foot
temperature was noted. (Fig 7.2)
3. Capillary refill time (CRT) was assessed at three points
i.e. midpoint of sternum, midpoint of left palm and sole
Fig 7.2. Human Touch method for
clinical assessment of Temp
Fig 7.3.Assessment of CRT on sole
-
SECTION-II 7 : Studies at KLEUH
60
Stop watch was started, moderate pressure to blanch
the skin was applied for 5 seconds and released.
Capillary refill was counted in seconds. Simultaneous
Blood pressure was noted. (Fig 7.3) Room temperature &
humidity were also noted at regular intervals during
the study using standard Thermo-Hygro clock (MEXTECH M288CTH JAPSIN
Instrumentation, India) (Fig 7.4)
Care in the Delivery Room:
Initially infants were wrapped in a cloth and kept under warmer with 40%
heater output. All the babies were wrapped
in a single piece of cloth brought by the
relatives. They were then given to the
mother for breast-feeding at mean (SD) age
of 0.75(0.5) hours after birth (Fig 7.5) and
remained with the mother until transfer to
postnatal ward (PNW). After stabilization,
both mother and newborn infant were
transferred to PNW with all the electronic
attachments to the baby. Mean time of transfer from DR to PNW was 2.5(0.8) hours
from birth, and mean (SD) time taken to transfer was 15(8) minutes.
Fig 7.4. MEXTECH
Thermohygroclock
Fig 7.5. Monitoring of the newborn in DR
with mother. Baby is placed next to the
mother wrapped in a cloth after first
breast feed
-
SECTION-II 7 : Studies at KLEUH
61
Care in Post Natal Ward:
Mother and baby dyad was wheeled in to
the postnatal ward with all the attachments to the
baby and uninterrupted electronic monitoring. They
were co- bedded as per the routine practice in the
postnatal ward and baby and mother were covered
with same blanket. (Fig7.6) Breast feeding was
continued uninterruptedly. The probe wires were
long enough to allow moving the baby on the bed.
Electronic monitoring was thus continued for
12 hours. Mother and her attendant were also
shown various parameters that were being monitored. If the probes got detached or
good waveform was not seen on the monitor, the probes were reattached, oxygen
saturation sensor replaced and the time noted to cancel those readings from the final
data analysis. After each completed study, the data was downloaded from the monitor
via USB port and transferred to a computer for processing.
With this experience of feasibility study, the time intervals for clinical
assessment of the babies were modified and the time for recording blood pressure was
also grouped in time intervals from birth to 12 hours. Our protocol initially included
record of the time of specific activities such as feeding, change of clothing etc by
mother. We found that the mothers were not much interested and they preferred to
rest during first 12 hours. Hence we deleted this record from assessment protocol. The
revised protocol was submitted to and approved by the ethical committee of the KLE
University.
Fig 7.6. Monitoring of the newborn
in PNW. Mother & baby are co-
bedded and covered with same
blanket.
-
SECTION-II 7 : Studies at KLEUH
62
Phase I Study:
This was carried out from July 2008 to September 2008 in the TCH which is a
rainy season in India. The analysis of data showed significant hypothermia in
newborns delivered in TCH (discussed later page no.77 to 81). To understand the
effect of seasonal variation we carried out Phase II of the study after rainy season.
Phase II Study:
This was carried out in the TCH from January 2009 to March 2009 which is
recognized by the local weather authority as spring season. We followed the same
protocol as in the Phase I study for enrollment and monitoring of the newborns.
We analyzed the data on electronic monitoring to understand the trends in
physiological parameters during transitional adaptation by infants delivered in TCH.
7.2. RESULTS OF PHYSIOLOGIC PARAMETERS MONITORED AT
KLEUH SITE:
600 deliveries occurred from July 2008 to October 2008 at this site. This being
a tertiary referral center, 50% deliveries were of antenatally detected high risk
mothers and hence excluded from the study. Of the rest mothers with no antenatal risk
factors, 40% needed some assistance during labor, 20% deliveries occurred at night
when all the necessary arrangements prior to the delivery were not possible and 10%
babies needed help in the form of free flow oxygen or bag and mask ventilation. With
these exclusion criteria being strictly followed we had a convenience sample of 30
infants over 3 months period in phase I and 38 infants in phase II study.
-
SECTION-II 7 : Studies at KLEUH
63
7.2. A. Demographic Characteristics
Of the 30 infants enrolled in phase I study, 8 infants were excluded due to
inadequate data collection or technical difficulties in data collection. Additionally 2
parents did not give consent to continue monitoring for 12 hours. The data of the
remaining 20 infants was included in the data analysis
Of the 38 infants in Phase II, 2 parents did not consent to continue monitoring
for 12 hours in the study. Data could not be recorded in 5 infants due to technical
difficulties. The remaining 31 infants were monitored as per the protocol and included
in the data analysis. Details of the infants included in the study are shown in Table
7.1. 55% were boys and 45% were girls. Both groups were comparable in regards to
birth weight and gestation.
Table 7.1. Demographic characteristics of newborns in Phase I & II at TCH
Site No & Gender Gestation
in Weeks
Birth Weight
(Grams)
TCH Phase I 6 Boys
14 Girls
38.7±1.1 2811±325
TCH Phase II 22 Boys
9 Girls
38.4±1.1 2856.6±318
Maternal details:
All mothers were in the age group of 19-28 years. 7(13%) were uneducated,
3(5%) had received primary school education only and the rest (80%) had received
secondary school education. All belonged to class III-IV modified BG Prasad
classification. [140]
Mean (SD) duration of labor was 9.6(4.3) hours. The mothers were
normotensive at admission and had mean (SD) Hb of 10.9(1.1)grams%. Majority
-
SECTION-II 7 : Studies at KLEUH
64
were second gravida (55%), 33% were primigravida and the rest were multi gravida
mothers.
Table 7.2 gives the details about mean duration of labor, Apgar score and
mean time taken to obtain first data in the two studies at TCH.
Table 7.2. Labor & delivery characteristics in phase I & II at TCH
Study
site
Mean
Duration
of labor
Mean
Apgar
Score
1 min
Mean
Apgar
score
5 min
Mean time
from birth to
first
data(minutes)
Mean time to
clamp the
cord
(Seconds)
TCH
Phase I
8.5±1.1
(6-11)
hours
7±1.2 8.3±0.5 3.2±0.25* 24.8±22.5
TCH
Phase II
7.9±1.8
(4-10)
hours
8.2±0.9 9.2±0.8 2.4±0.3* 22.8±17.3
* Difference statistically significant ( P=.02)
There was no significant difference in duration of labor in mother and mean
time to clamp the cord in two phases. Mean Apgar score in both groups were 7,8 and
8,9 at 1 and 5 minutes respectively. The difference in time to acquire first data from
time of birth was significant in the two phases.
7.2. B. Analysis of oxygen saturation:
Fig 7.7 shows a typical SpO2 recording in a baby in the delivery room. This
was a term baby boy weighing 3100 grams who did not require resuscitation after
birth. First SpO2 tracing was obtained at 95 seconds in this infant and total 7778
data points for SpO2 were collected at an interval of 5 seconds over 11 hours time
from birth. The values shown in graph are the SpO2 values at 30 seconds time interval
-
SECTION-II 7 : Studies at KLEUH
65
over first 30 minutes of life. The infant achieved SpO2 of 90% by 6 minutes and 95%
by 7.5 minutes from birth.
Fig. 7.7. Change in SpO2 over 15 minutes period from birth in a newborn at TCH
Table 7.3 gives the median (IQR) oxygen saturation at intervals of one minute
from birth to 15 minutes of age. The first median (IQR) oxygen saturation level which
was recorded in 9 newborns by 2 minutes of age was 69%(68-79). At 5 minutes
median SpO2 was 88%. A gradual rise in SpO2 is seen till it reaches a plateau of 96%
from 12 minutes of life. Number of babies in whom SpO2 was recorded is also shown.
50 55 60 65 70 75 80 85 90 95
100
0.0
1.0
2.0
3.0
4.0
5.0
6.0
7.0
8.0
9.0
10
.0
11
.0
12
.0
13
.0
14
.0
S
p
O
2
%
Time from birth in minutes SpO2(%)
-
SECTION-II 7 : Studies at KLEUH
66
Table 7.3. Median (IQR) values of oxygen saturation (SpO2%) from one to
fifteen minutes and one to twelve hours of birth.
TFB
(min)
Median SpO2(IQR) TFB
(hours)
Median
SpO2(IQR)
2 69(68-79)N=9 1 98(95-100)N=48
3 80(74-91)N=27 2 98(95-100)N=46
4 82.5(76-90)N=34 3 97(95-99)N=49
5 88(81-90)N=42 4 97(95-100)N=50
6 89(83-92.5)N=43 5 96(94-98)N=46
7 91(87-96)N=46 6 96(93-98)N=44
8 92(87-97)N=45 7 95(93-98)N=48
9 93(88-97)N=45 8 96(94-98)N=49
10 94(88-97)N=45 9 96(94-97)N=47
11 95(93-97)N=45 10 96(94-97)N=48
12 96(91-98)N=45 11 96(94-97)N=47
13 96.5(90-98)N=46 12 95(93-97)N=49
14 96.5(92-99)N=46
15 96(93-99)N=46
Figure 7.8 shows the cumulative sequential changes in oxygen saturation in all
51 babies studied. The median level of SpO2 of 90% and 95%saturation was attained
at 6.5 minutes and at 11 minutes of life respectively.
-
SECTION-II 7 : Studies at KLEUH
67
Fig 7.8. Box and Whiskers graph showing change in SpO2 over first 15 minutes
in 51 infants at TCH
Box and Whiskers graph showing change in SpO2 over first 15 minutes in 51 infants.
The median and IQR of oxygen saturation at intervals of one minute are shown. Box
gives the interquartile range (25th
to 75th
centile) and the whiskers represent 1.5 IQR
beyond each box. Median is represented by the horizontal line in the box.
40
50
60
70
80
90
100
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15
SpO
2 %
Time From Birth in Min
-
SECTION-II 7 : Studies at KLEUH
68
Difference in trends in SpO2 in two seasons:
Fig 7.9 shows the trend in SpO2 change in phase I and phase II study at TCH.
Infants from both groups achieved oxygen saturation of 95% by 11 minutes. The
difference in SpO2 at 2 and 3 minutes though clinically significant it is not statistically
significant due to small no. of readings.(N=3&9 at 2&3 min respectively in Phase I)
Fig 7.9. Trends in SpO2 in infants delivered in phase I & II at TCH
7.2. C. Color and Oxygenation
At birth all babies had blue or pale palms and soles. Tongue and oral mucosa
was pink at birth except in 2 infants but they did not require supplemental oxygen as
per NRP 2006 protocol and all infants were centrally pink by 5 minutes.
Fig7.10 shows sequential changes in the color of palms and soles over first 2
hours in a newborn infant. This was full term normal vaginal delivery and baby did
not need resuscitation. The color changed to pink gradually over next few minutes.
Fig7.10.a & Fig 7.10.b shows color of palms and soles by 5 minutes of life.
Oxygen saturation at this time was 89%. Both palms and soles were dusky.
10
20
30
40
50
60
70
80
90
100
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15
S
p
O
2
%
Time from birth in minutes
SpO2 Phase II SpO2 Phase I
-
SECTION-II 7 : Studies at KLEUH
69
Fig 7.10.c & fig. 7.10.d color of palms and soles at 15 minutes of life when
oxygen saturation was 100%. Note the change in color of palms but soles still have
dusky hue.
Fig 7.10.e & Fig 7.10.f Color of palms and soles at 2 hours of life.Both palms
and soles were bright pink in color and oxygen saturation was > 95%. Soles were still
cold to touch.
Fig 7.10.b Blue soles at 5 minutes
Fig 7.10.a Blue palms at 5 minutes
Fig 7.10.d Blue soles at 15 minutes Fig 7.10.c Color of palms improved towards pink by 15 minutes
Fig 7.10.e Pink palms at 2 hours
Fig 7.10.f Pink soles at 2 hours
Fig 7.10.f Pink soles at 2 hours
-
SECTION-II 7 : Studies at KLEUH
70
Infants with initial pale palms and soles developed dusky hue before turning
pink and took comparatively longer time to become pink. During this phase the
oxygen saturation changed from 96%to 97 %. (Difference in SpO2 is not statistically
significant.P=.1) The readings showed skewed distribution. Median (IQR) time taken
for palms to become pink from blue was 30 minutes (16.2-135 minutes, N=40)) but
pale palms took significantly longer time 3.25hours (2.9-4.4,N=11)) to become pink.
This was also associated with CRT > 4 seconds (discussed later Page no76). By 15
minutes 19 (37.25%) infants had pink palms but pink soles were noted in only one
baby (2%).
Table 7.4 shows the sensitivity and specificity of pink color (combined data of
blue/pale palms and soles to pink) & warmth of palms & soles in relation to SpO2
≥95% & abdominal temperature (Ta) ≥ 36.50C at specific time intervals from birth.
The time intervals were determined based on the mean time at which the change in
color and temperature was noted.
Table 7.4. Sensitivity & specificity of color and touch to recognize normal oxygen
saturation and body temperature from birth.
Pink Palms Pink Soles Pink &
Warm Palms
Pink & warm
Soles
TFB
Median(IQR)
30(16.2-135)min 3.3(1.3-
5.1)hours
3.3(2.5-
6)hours
6.5(4-8)hours
Sensitivity 77% 65% 70% 66%
Specificity 14% 20% 36% 20%
By one hour 41 infants (80%) had pink palms where as only 12 (23.5%)
infants had pink soles. No significant differences were found in saturations when
-
SECTION-II 7 : Studies at KLEUH
71
palms became pink (96%) as compared to saturations when soles became pink (97%).
16 (31%) infants had blue palms when SpO2 was less than 92 %.( Table 7.5).
Soles always became pink later than the palms. Blue soles became pink earlier
(median time 2.1 hours N=41) than soles that were pale at birth (median time 6 hours,
N=10). But there was no statistically significant difference in SpO2. All babies took
11 minutes to reach SpO2 of 95% but the palms and soles became pink only by
3.3(1.3-5.1) hours. Thus there was a significant discordance between skin color and
actual oxygen saturation. This is a clinically important observation.
Table 7.5. Oxygen saturation and clinical assessment of color & warmth.
SpO2 98%
Palms pink & Warm (N=51) 3 12 16 20
Soles Pink & warm (N =51) 1 18 12 20
Palms remained blue and cold
(max SpO2)(N=51)
16 7 17 11
7.2. D. Changes in heart rate
The earliest recorded median (IQR) heart rate was 182 bpm (160-189). By 15
minutes it gradually came down to 154bpm (145-169). Fig 7.11 is a box and whiskers
showing change in heart rate over first 15 minutes of birth.
-
SECTION-II 7 : Studies at KLEUH
72
Fig. 7.11: Change in heart rate in 51 infants in first 15 minutes at TCH.
Fig. 7.11. is a Box and Whiskers graph showing change in heart rate (bpm)
over first 15 minutes in 51 infants. The median and IQR of heart rate at intervals of
one minute are shown. Box gives the interquartile range (25th
to 75th
centile) and the
whiskers represent 1.5 IQR beyond each box. Median is represented by the horizontal
line in the box.
All the values are shown in Table 7.6. It also gives the values of HR every
hour from 1 to 12 hours of life .
Table 7.6. Median heart rate in bpm from 2 to 15 minutes of life and 1 to 12
hours of life
TFB (minutes) HR bpm
Median (IQR)
TFB (Hours) HR bpm
Median (IQR)
2 182(160-189)N=9 1 136(128-142)N=48
3 183(167-192)N=27 2 127(114-138)N=46
4 179(150-190)N=34 3 118(111-123)N=49
5 180(167-190)N=42 4 118(110-130)N=50
6 175(163-186)N=43 5 118(109-125)N=46
10
60
110
160
210
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15
h
e
a
r
t
R
a
t
e
Time from birth in minutes
-
SECTION-II 7 : Studies at KLEUH
73
7 176(159-184)N=46 6 119(108-128)N=44
8 167(158-181)N=45 7 122(113-138)N=48
9 166(154-181)N=45 8 123(112-134)N=49
10 165(154-173)N=45 9 121(112-135)N=47
11 163(150-173)N=45 10 124(116-136)N=48
12 160(149-172)N=46 11 122(114-137)N=47
13 156(144-171)N=46 12 125(116-132)N=49
14 157(148-170)N=46
15 154(145-169)N=46
Heart rate came down even further to 118 bpm (111-123) by 3 hours of life. At
12 hours the median heart rate recorded was 125 bpm (116-133).
7.2. E. Trend in NIBP over 12 hours
We ensured that the NIBP was recorded when baby was quiet after application
of the cuff and during recording of the blood pressure as per the standard
recommended protocol. This was difficult especially in the first fifteen minutes and at
times we had to abandon recording the blood pressure. We recorded 351 NIBP
readings in 51 babies. However we excluded 65 readings as they were out of the
specified time or taken during excessive movements or crying. So we analyzed 289
readings (83%) of which 172 readings were taken in first hour of life. The earliest
NIBP reading recorded was by 4 minutes of age.
For analysis the mean blood pressure readings during each 15 minutes interval
in first hour of life, every 3 hours till 6 hours and then between 6-12 hours were
calculated as shown in table 7.7.
-
SECTION-II 7 : Studies at KLEUH
74
Table 7.7. Mean±SD systolic, diastolic and mean blood pressure from 5 minutes
to 12 hours after birth.
TFB No of
infants
Systolic BP
mmHg
Diastolic
BP mmHg
Mean BP
mmHg
5-15 min 33 70.05±9 43.7±9 52.5±8
15-30 min 49 68.21±8 41.4±7 50.4±7
30-45 min 44 69.5±11 40.9±8 50.5±8
45-60 min 46 69.9±8.5 41.2±7 50.1±7
1-3 hours 41 68.0±6 41.0±7 50.8±5
3-6 hours 34 65.2±7* 39.2±7* 48.1±6*
6-12 hour 35 69.1±8 43.76±7 52.05±9
*Statistically significant difference in blood pressure compared to all previous and
later readings.(P
-
SECTION-II 7 : Studies at KLEUH
75
from 1-6 hours of birth. The difference was statistically significant when compared
with previous readings till 3 hours. A gradual rising trend in the blood pressure was
seen between 6-12 hours interval.
7.2. F. Capillary Refill Time
Capillary refill time was more prolonged in soles than palms at 5 minutes.
(Maximum 8 seconds on soles, 5 seconds on palms, and 3 seconds on sternum) .It
gradually decreased in all areas especially in first hour as shown in table 7.8.
Table 7.8. Mean CRT±SD from 5 minutes to 12 hours of birth on palms and soles
Time from birth 5min 15min 30min 1hr 12 hours
CRT palm (sec) 4.5±.7 3.7±0.6 3.3±0.45 3.16±0.37 3±0.22
CRT sole(sec) 5.8±0.9 5.1±1.2 4.8±1.1 4.1±1.01 3.3 ±0.46
CRT sternum (sec) 3±0.52 2±0.50 2±0.37 2±022 2±022
Mean CRT was 3.3±.45 seconds in palms when they became pink. We
observed that the CRT improved first followed by change in color to bright pink both
in palms and soles.
We compared the mean CRT with systolic blood pressure to study their
correlation.
Table 7.9 gives mean CRT on soles, mean systolic blood pressure, and
sensitivity and specificity of CRT on soles to mean systolic blood pressure in every 15
minutes interval from birth to 1 hour of life. There was no major change in mean
systolic pressure from 1 to 60 minutes of life (not statistically significant) but the
difference in CRT from 5 minutes to 1 hour was statistically significant.
-
SECTION-II 7 : Studies at KLEUH
76
Table 7.9. CRT, mean ±SD systolic blood pressure at specific time intervals from
birth till 1 hour, Sensitivity & specificity of CRT to mean systolic blood pressure
Time from
birth
CRT Sole
(min)
Mean Systolic BP
with 95% CI
(mmHg)
Sensitivity Specificity
5-15 min
N=34
5.8±0.9 70±9.2
67.2-73
69% 50%
15-30 min
N=44
5.1±1.1 68.2±8.2
66.3-70.3
65% 31%
30-45 min
N=48
4.3±1.1 69.9±8.4
67.3-72.4
77% 35%
45-60 min
N=49
3.5±0.6 69.9±8.5
67.4-72.3
64% 41%
CRT remained prolonged for longer time over palms & soles when palms &
soles were cold.
The order of physiologic transition that we noted was: improved oxygen
saturation (11minutes), CRT shortening on palm (15min-1 hour), pink color (30min-
3.3hours) & warmth (3.3-6.5hours).They progressed in cephalo caudal manner: hands
to feet.
7.2. G Abdominal and foot temperature in first 12 hours
Phase I of our study was conducted from July to October 2008. This was rainy
season and Belgaum had the typical cold (environmental temperature 18- 270C) and
humid (50-90%) weather during the study period. Phase II was conducted from
January to March 2009 which was spring time in this part of Karnataka.
Environmental temperature during this period varied from 22-280C and humidity was
in the range of 35-45%.
-
SECTION-II 7 : Studies at KLEUH
77
Table 7.10 gives the mean room temperature(0C) and humidity(%) in the DR
and PNW of KLEUH during the study period. The temperature in the DR was 0.80C
lower than in PNW during both seasons and the temperature in DR and PNW was
higher by a minimum of 1.50C during the spring season compared to that of rainy
season. Humidity in rainy season was 30% higher than during spring season.
Table 7.10. Room temperature and humidity in Rainy (Phase I) &
spring (Phase II) seasons in DR & PNW at TCH
Location DR PNW
Season Rainy Spring Rainy Spring
Room Temperature0C
Mean±SD
24.5 ±1.3* 26.18±1.1 * 25.36± 1.14 * 26.9±1.3 *
Humidity Mean±SD 79.3±8 %* 47.2± 6%6 * 81±9% * 50± 8 %*
*The difference in temperature and humidity in DR and PNW was significant
during the two phases.
Thermal Adaptation in Rainy & Spring Season:
Temperature trends of Phase I and Phase II are shown in Figure 7.13. The
trends in Ta and Tf in different seasons are plotted against time from birth to 12 hours
of age. Both the groups started at similar Ta and Tf in the delivery room. The mean
Ta in both groups continued to be similar all through the study period. The mean time
taken to reach temperature (Ta) of 36.50C by 50% infants was 3.9 hours. A significant
difference was seen in mean Tf between the two groups in the delivery room and in
the postnatal ward (P=0.02, P=0 respectively).
-
SECTION-II 7 : Studies at KLEUH
78
Fig 7.13. Trends in abdominal(Ta) and foot (Tf) skin temperature from 5
minutes to 12 hours of birth in rainy(phase I ) and spring (phase II) season.
Difference in Trends by Season:
Rainy season: in the delivery room the mean (SD) Ta was 34.60C (0.69) at 5 minutes
and reached maximum of 35.90C (0.6) at 2 hours of age, but the mean (SD)Tf dropped
precipitously to 30.30C(1.5) by 2.5 hours. Mean Td increased from 3.5(0.8) at 15
minutes to 5.48(0.9) before transfer of the infant to the PNW. During transfer of the
infant to the PNW Tf dropped further reaching a mean Tf of 30.20C (1.3) and Td of
5.30C (1.4) at 3 hours of age. In the PNW the mean Ta &Tf dropped further down to
35.50C (0.8) and 29.7
0C (1.33) by 4.5 hours. Ta gradually increased to 36.02(0.4) at 8
hours of age and rose further to 36.40C (0.48) by 12 hours of age. Mean Tf increased
to 32.90C (2.97) by 12 hours. Mean Td also increased to 5.94
0C (1.39) at 4.5 hours of
age and decreased gradually to 3.540C (1.56) by 12 hours.
Spring Season: in the delivery room the maximum mean (SD) Ta was 35.80C (0.51)
by 1 hour of age. The lowest recorded Ta and Tf was 35.270C (1.8) and 30.39
0C(1.28) respectively with maximum mean (SD) Td of 5.2
0C(1.1) at 1.5 hours. During
28.0
29.0
30.0
31.0
32.0
33.0
34.0
35.0
36.0
37.0
38.0
0.1
0.5
0.8
1.0
1.5
2.0
3.0
4.0
5.0
6.0
7.0
8.0
9.0
10
.0
11
.0
12
.0
T
e
m
p
0
C
Time from birth in hours
Ta (phase I)
Tf ( phase I)
Ta (phase II)
Tf (phase II)
-
SECTION-II 7 : Studies at KLEUH
79
transfer Tf dropped further to 30.330C (0.12) and Td increased to 5.3
0C (1.2) but Ta
was maintained at 35.60C (0.08) during this period. In the PNW, the mean (SD) Tf
dropped to the minimum of 30.130C (0.14) by 2.5 hours and then showed a consistent
rise to maximum of 33.50C (1.9) by 12 hours of life. Ta showed a rising trend to reach
maximum of 36.50C (1.9) by 12 hours of life.
Table 7.11 gives mean ±SD Ta and Tf in DR and PNW in two seasons. The
difference in abdominal temperature though small, was statistically significant in two
seasons. The foot temperature was significantly higher in DR and PNW in spring
season than in rainy season.
Table 7.11. Mean ±SD Ta & Tf in DR & PNW in Rainy and spring season
Ta Mean(SD) Tf Mean (SD)
DR PNW DR PNW
Rainy season(I) 35.6±0.26 35.9±0.24 30.6±0.43 31.3±1.07
Spring season(II) 35.6±0.21 36.1±0.19 31.2±0.58 32.6±0.76
P(Rainy vs. spring) NS 0.0002 .002 0
Selected data points in 2 groups at 0.08 hours (5 minutes), 2, 6 and 12 hours
are shown in Table 7.12. Ta, Tf is high and Td is low at all points in infants from
Phase II but the difference in Ta, Tf and Td between two groups is statistically
significant at 6 hours from birth(P ≤.04). At 12 hours the difference is marginally
significant for Tf (P
-
SECTION-II 7 : Studies at KLEUH
80
Table 7.12. Mean ±SD Ta & Tf at specific time from birth in phase I & II
Time
from
Birth
(hours)
Ta (I)
Mean± SD
Ta(II)
Mean± SD
Tf(I)
Mean ± SD
Tf(II)
Mean± SD
Td( I)
Mean± SD
Td(II)
Mean± SD
0.08 34.62±0.69 34.65±0.53 32.39±0.94 32.55±0.95 2.24±1.2 2.10±1.3
2.00 35.9±0.63 35.48±0.9 30.53±1.39 30.40±1.44 5.34±1.4 5.08±1.12
6 35.63±0.63* 35.95±0.46* 30.38±1.42* 32.51±1.5* 5.33±1.1* 3.44±1.5*
12 36.36±0.48 36.48±0.31 32.21±2.9 33.51±1.97 3.54±1.56 2.96±1.7
*P ≤.04 (SD) Standard Deviation
Area Between The curves Ta and Tf:
We assumed that the area between Ta and Tf over a unit time serves as a
proxy to metabolic stress in the baby. To estimate this stress we calculated the area
between mean Ta and Tf from birth to 12 hours age using the trapezoidal rule.
Fig 7.13 shows the area between Ta and Tf at three different locations. Table 7.13
shows the difference in Ta and Tf at each location of the infant from birth to first 12
hours of life and the metabolic stress experienced by these infants in these locations in
both seasons. The area between the curves Ta and Tf at each of the locations is
shown. The area between the curves per hour was the highest during transfer of the
infant from DR to PNW when Td widened further in both the groups and it was least
in the PNW when a gradual increase both in Ta and Tf was seen. The difference in Td
between both groups was statistically significant at all three locations. The stress
experienced during rainy season was also higher in all three locations but the
maximum total stress was observed in the PNW (75%) in both the groups.
-
SECTION-II 7 : Studies at KLEUH
81
Table 7.13. Difference between Ta and Tf (Td) and Area between Ta and Tf
Location
(Duration in
hours)
Td 0C Mean±SD Metabolic stress :Area between
Ta and Tf
Phase I Phase II Phase I Phase II
DR(2.5) 5± 0.72* 4.4± 0.72* 48428.47
(23 %) 17295/hr
26613(16 %)
15207.3/hr
TRANSFER(0.5) 5.39± 0.09* 5.27± 0.18* 14622.26 (6%)
29244/hr
14196 (8.6%)
28392/hr
PNW(8.5) 4.39± 1.03* 3.75± 0.87* 141041.92 (70%)
16593/hr
124037(75%)
12403.3/hr
*P≤.02.
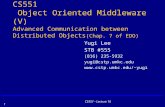
Fig 7.14 gives AUC (0C.min) between Ta & Tf in Phase I at three different
locations of infants after birth till 12 hours. Shaded area represents the metabolic
stress experienced by the infants. T stands for transport of infants from DR to PNW.
Fig 7.14. AUC between Ta and Tf in phase I