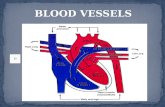
Blood Vessels
description
Transcript of Blood Vessels

2/25/08
Blood Vessels
Chapter 19 – Day 1

2/25/08
Blood Vessel Structure
Fig. 19.1

2/25/08
Blood Vessels - Intro
Blood vessels are essentially a “pipeline” to:♦Carry blood TO parts of the body = arteries♦Carry blood BACK FROM parts of the body = veins
Subdivisions♦Pulmonary blood vessels: blood to the lungs and back♦Systemic blood vessels: blood to and from the rest of the
body

2/25/08
Blood Vessels - Intro
Veins = mostly deoxygenated – except pulmonary vein & umbilical vein
Arteries = mostly oxygenated – except pulmonary artery & umbilical artery
Capillaries = interconnecting vessels♦Enable gas exchange, etc.
Blood vessel structure and comparison activity in lab

2/25/08
Blood Vessel Structure
Fig. 19.1

2/25/08
Arteries vs. Veins - Similarities 3 LayersTunica Externa
♦Connective TissueTunica Media
♦Smooth muscle cells ♦Elastic fibers (arteries)♦Collagen fibers
Tunica Interna♦Elastic layer♦Endothelial cells & connective tissue with elastic fibers
(arteries)

2/25/08
Arteries vs. VeinsArteries are thick walledLarger arteries have more elastic fibers
♦Tunica media – thicker, concentric & longitudinal♦Tunica interna – internal elastic membrane
ARTERIES♦Elasticity
•Ability to stretch when full = high pressure•Return to their original state when relaxed
♦Contractability•More smooth muscle (than veins)•Vasodilation, Vasoconstriction
Both veins & large arteries need O2 – supplied by vaso vasorum

2/25/08
Arteries vs. VeinsHierarchy of organization
♦(learn examples from text)Largest vessels coming out of heart or to heartThese carry the most volume
♦If arteries – they have the highest pressureDiagram on board and Fig. 19.2
Be able to work though these – know order and characteristics

2/25/08
Blood Vessel Hierarchy
Fig. 19.2

2/25/08
Capillaries
Fig. 19.5

2/25/08
Arteries vs. VeinsDifferent jobs and different driving forcesArteries
♦Force of contraction pushes blood forward♦Blood pressure = driving force♦Moves downhill to lower extremities - gravity
Veins ♦Lower extremities to heart = against gravity♦Low pressure♦Relies on other driving forces

2/25/08
VeinsTwo features help to push blood forward:
♦Valves – keep blood from flowing backward (flow is possible in 1 direction only)
♦Skeletal muscle contraction•Helps to push blood forward
♦Breathing action•Pressure in chest helps venous flow
♦All contribute to venous return
Fig. 19.6

2/25/08
Blood vessel functionUltimately blood delivers O2 & nutrients to tissues as
well as removing wastes How does this happen?Any organ:
♦Blood vessels (in & out): arteries – smallest branch = capillary
♦The organ is infused with capillaries♦Nutrient exchange occurs at this level
In the capillaries – only the endothelial layer is presentSubstances in the capillaries move to the Interstitial
Fluid → then into cells

2/25/08
O2, Nutrient, and Waste ExchangeWaste products are released into the interstitial fluid
Waste products are then taken up by fenestrated capillaries because they are typically large molecules (recall differences between fenestrated & continuous capillaries)
Fig. 19.4

2/25/08
O2, Nutrient, and Waste Exchange Exchange between blood and interstitial fluid
1. Simple (& Facilitated) Diffusion:♦In response to a concentration gradient
2. Filtration♦Force pushes out substances – based on pressure
3. Osmosis♦Reabsorption of water

2/25/08
Diffusion Ions and small organic molecules (glucose, amino
acids, urea – move through pores in fenestrated capillaries or move via diffusion between endothelial cells of adjacent capillaries
Ions (Na+, K, etc.) diffuse across endothelial cells by passing through channels in cell membranes
Large water-soluble compounds can only work enter or leave blood stream via fenestrated capillaries
Lipids (FAs, steroids) and lipid-soluble compounds (esp. CO2, O2) cross capillary walls by diffusion through endothelial cell membranes
Plasma proteins can only diffuse through in sinusoids (such as those in the liver)

2/25/08
Filtration Driving force =
PRESSURE in capillary = Capillary Hydrostatic Pressure (CHP)
Water is forced across a capillary wall and small solutes travel with the water♦Through endothelial cells
or pores of fenestrated capillaries
Fig. 19.11

2/25/08
Reabsorption Occurs as a result of osmosis
♦Diffusion of water across selectively permeable membrane•Remember, water molecules move toward soln with higher
solute concentration Process by which dissolved solutes is moved Osmotic pressure = amount of pressure that must be
applied to prevent osmotic movement across a membrane (Blood Osmotic Pressure = BOP; IOP=?)♦BCOP = blood colloid osmotic pressure = osmotic pressure
of blood (also BOP) Remember…hydrostatic pressure forces water OUT
of solution, whereas osmotic pressure draws water INTO a solution (BHP vs. IOP; BOP vs. IFHP)

2/25/08
Pressures have to be balanced so that fluid in and out can be coordinated – refer to handout (review!!)
Fig. 19.11

2/25/08
Filtration & Reabsorption If BHP > BOP in the blood vessel, fluid is pushed out If BHP < BOP fluid enters in
IFHP & IOP – low & stable because there are fewer proteins in interstitial fluid
Net Filtration Pressure is the difference between the net hydrostatic pressure and the net osmotic pressure: ♦Net filtration = net hydrostatic – net colloid pressure pressure osmotic pressure
If positive fluid moves OUT of capillary If negative fluid moves INTO capillary

2/25/08
Equilibrium Analogy to filtration experiment
♦Charcoal = cells & proteins♦CuSO4 = nutrients & O2
Cells & Proteins remain in blood vessel H2O, hormones, other chemicals, nutrients, O2,
glucose, ions = pushed out Equilibrium between arterial & venus ends maintains
proper pressure differences (Starling’s Law of Capillaries)
Excess fluid expelled into tissues causes an increase in interstitial fluid – if in excess, causes EDEMA♦Excess fluid buildup, swollen ankles, etc
Read in book and follow handout

2/25/08
Equilibrium Equilibrium between arterial & venus ends maintains
proper pressure differences Excess fluid expelled into tissues causes an increase
in interstitial fluid – if in excess, causes EDEMA♦Excess fluid buildup, swollen ankles, etc
Read in book and follow handout Different demands for gas and nutrient exchange For proper delivery – the cardiovascular system
depends on:1. Cardiac Output2. Peripheral Resistance3. Blood Pressure

2/25/08
St

2/25/08
Blood Pressure and Blood Vessels Blood Pressure
♦Pressure within blood vessels♦Influenced by cardiac output, but other factors are involved
as well
1. Vasomotor tone♦Muscle tone of smooth muscle♦Resistance against blood♦This is controlled by the medulla in the brain♦VASOCONSTRICTION - ↑ sympathetic impulse♦VASODILATION - ↓ sympathetic impulse♦THESE CHANGES AFFECT BLOD PRESSURE

2/25/08
Blood Pressure and Blood Vessels Blood Pressure1. Vasomotor tone2. Baroreceptors
♦Monitor the degree of stretch♦Special receptor nerve cells in specific areas of the body♦Baroreceptors adjust cardiac output & resistance
3. Chemoreceptors♦Special nerve cells sensitive to chemical concentrations♦These sense arterial levels of CO2, O2, H+ (pH),♦Can adjust constriction based on the concentration of these
chemicals

2/25/08
Blood Pressure and Blood Vessels Blood Pressure4. Cerebral Cortex
♦Stress, anger, depression♦All of these emotions affect the sympathetic division of the
nervous system♦The cerebral cortex alters blood pressure/flow by altering
levels of vasoconstriction/vasodilation
5. Local Changes♦Sphincters near capillaries
6. Chemicals♦Drugs♦Alter vasodilation & constriction

2/25/08
Hypertension Abnormally high BP levels (>150/90)
♦Approximately 25% of the population suffers from hypertension
Cause & Effects♦uncertain♦Heart works harder – O2 demand is high ♦Hypertension: accelerates artherosclerosis, increases clot
formation, causes kidney damage Treatment
♦To reduce heart workload♦Diuretics - ↓ blood volume (increasing urine output)♦Vasodilators – relax smooth muscle♦β – blockers: affects sympathetic receptors (reduces cardiac
output)♦CA2+ blockers: reduce cardiac output

2/25/08
Other Vessel Disorders Varicose veins
♦Hemorrhoids Circulatory Shock
♦Hematogenic Shock♦Cardiogenic Shock♦Neurogenic Shock♦Septic Shock

2/25/08
Equilibrium Need constant control of these factors to maintain
homeostasis= CARDIOVASCULAR REGULATION
Controlled by♦Autoregulation Mechanisms
•Local factors change pattern of blood flow w/in capillary beds•Response to chemical changes in interstitial fluids
♦Neural Mechanisms•Respond to changes in arterial pressure or blood gas levels @
a specific site stimulates cardiovascular centers of ANS♦Endocrine Mechanisms
•Releases hormones that enhance short-term adjustments and direct long-term changes in cardiovascular performance

2/25/08
Auto Regulation Local changes
♦Sphincters near capillaries are adjusted♦Depend on local VASODILATION & VASOCONSTRICTION
chemicals (nitrous oxide) – know examples from text (p 547)•Vasodilator: factor(s) that promote the dilation of precapillary
sphincters•Local vasodilators act at the tissue level & accelerate blood
flow through the tissue of origin

2/25/08
Neural Mechanisms Neural Mechanisms
♦Sympathetic division controls…•Smooth muscle tone (vasomotor tone)•Increased sympathetic impulses ( vasoconstriction)•Decreased sympathetic impulses ( vasodilation)
♦Receptors

2/25/08
Capillaries
Fig. 19.5