BIO 265 – Human A&P II
-
Upload
stacey-curtis -
Category
Documents
-
view
27 -
download
0
description
Transcript of BIO 265 – Human A&P II

BIO 265 – Human A&P II
Chapter 19
Blood Vessels

Blood Vessels
• Amazing fact about blood vessels:– 60,000 miles in an adult!
– Earth’s circumference is 24,902 miles
• What are the different types of blood vessels?– Arteries - elastic, muscular, and arterioles
– Capillaries
– Veins – venules and veins
• Figures 19.1 and 19.2 and Table 19.1

Blood Vessels
• The inside of a blood vessel is called the lumen• All blood vessels have an internal lining called
endothelium (it lines the lumen)– Simple squamous epithelium
– This layer is continuous with the endocardium
• Capillaries:– Composed of endothelium with a basement membrane
– Figure 19.3 and others

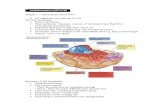
Structure of Arteries and Veins
• Three tunics or layers:– Tunica intima – primarily endothelium– Tunica media – location of circular smooth
muscle and elastin• Functions?
– Tunica adventitia – layer of connective tissue• Merges with other connective tissue around the
vessel• Also contains the vasa vasorum
– Figure 19.1 and other figure

Structure of Arteries and Veins
• Veins have valves that only allow blood to flow toward the heart– The valve structure and function is very similar
to the semilunar valves in the heart
• Figure 19.1 and other figure

Structure of Arteries and Veins
• The valves in the veins are critical for returning blood to the heart because there is almost no blood pressure in the veins– Blood is pumped through the veins by
respiration (breathing) and by skeletal muscle contractions
• Figure 19.6

Structure of Arteries and Veins
• Varicose veins result from these valves not functioning properly– Pot-bellies, pregnancy, standing, hemorrhoids– Figure 19.6

Capillaries
• What is the function of capillaries?– Capillary Exchange
• gases, nutrients, wastes, etc.
– Capillary exchange is driven by 2 things:• Concentration gradients (diffusion)
– Most solutes move this way
• Fluid movement (primarily moves water to the tissues)
– Tissue swelling and the lymphatic system
– Figures 19.14, 19.15, 19.2 and others

Capillaries
• Capillaries are organized into networks called capillary beds– Figure 19.4

Capillaries
• The structure of the capillary beds allows the regulation of blood flow through the tissues– This involves the precapillary sphincters– Figure 19.4

Control of Blood Flow
• Blood flow through tissues (tissue perfusion) is tightly controlled– It is related to the metabolic rate and function
of the tissue (muscle, liver, kidney, etc.)
– O2 (and other nutrients) are the key
• They are required for smooth muscle contraction
– Figure 19.4

Control of Blood Flow
• Long-term control involves the number of blood vessels and capillaries– Muscle and heart attack examples
• The growth of new blood vessels is called angiogenesis
• The density of capillaries primarily depends upon O2 concentration

Aging of Arteries
• Changes in arteries:– Arteriosclerosis – loss of elasticity in the
arteries• What effects does this have?
– Atherosclerosis – deposition of material in the arterial walls to form plaques
• Effect?
• Figure from other text

Blood Pressure Regulation
• Blood Pressure depends on 3 primary factors:– Cardiac output– Peripheral resistance (this is determined by
blood vessel diameter)– Blood volume

Blood Pressure Regulation
• There are two types of regulation:– Short-term and Long-term
• Short-term– Baroreceptors – get with a partner and discuss how this
mechanism could affect blood pressure.• They affect the cardiovascular center in the medulla
• This can change heart rate and peripheral resistance to raise and lower BP!
• Figure 19.8

Blood Pressure Regulation• Chemoreceptor Reflexes
– When oxygen, pH, or carbon dioxide levels change dramatically, the cardiovascular center can increase blood pressure.
• Adrenal Medulla Hormones– What hormones are produced here?– These affect heart rate and peripheral resistance
• Increase heart rate
• Vasodilation in cardiac vessels
• Vasoconstriction in vessels to the skin and viscera

Blood Pressure Regulation• Atrial Natriuretic Peptide (ANP)
– Released when atria are stretched– Increases Na+ loss in the urine– Also causes vasodilation– Effect?
• ADH (vasopressin) – at very high levels causes vasoconstriction
• Angiotensin II – vasoconstriction• Inflammatory chemicals (like histamine) cause
vasodilation• Alcohol – inhibits ADH and causes vasodilation

Blood Pressure Regulation
• Long-Term Regulation (these alter blood volume):• Direct renal filtering
– High BP causes more fluid to get filtered and lost– Low BP slows filtration and loss down
• Atrial Natriuretic Peptide – effect?• Renin-Angiotensin-Aldosterone Mechanism
– When BP decreases, the kidneys secrete renin– Renin activates a plasma protein called angiotensin II– Active angiotensin II causes vasoconstriction and the
release of aldosterone from the adrenal cortex

Blood Pressure Regulation
– Aldosterone increases Na+ and Cl- absorption by the kidney which increases water retention
– Angiotensin can also stimulate the release of ADH
– This mechanism is very important for daily regulation of BP and in countering circulatory shock
• ADH – effect?

Alterations in Blood Pressure
• Hypotension (BP below 100 mm Hg) – usually no problem
• Hypertension (BP over 140/90 mm Hg)– Temporary high BP can be normal– Strains the heart– Contributes to atherosclerosis– Can lead to heart failure– Cause is usually unknown

Circulatory Shock
• Shock is a condition where blood flow is not adequate to meet the body’s needs– (Low blood pressure)– Hypovolemic shock – blood loss, dehydration,
extensive burns– Vascular shock – extreme vasodilation
• Anaphylactic shock
• Septic shock – bacterial toxins