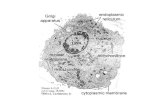
Bacteriology
-
Upload
margie-morgan -
Category
Education
-
view
6.121 -
download
0
Transcript of Bacteriology

Bacteriology Review

Beginning definitions• Obligate Aerobe – require oxygen (20%) to grow• Obligate Anaerobe –>30 min of oxygen exposure can be toxic• Facultative anaerobes – grow in aerobic and anaerobic
conditions, most “aerobic” bacteria are actually facultative• Microaerophilic – Grow better with reduced oxygen and
elevated Carbon dioxide %
• Aerotolerant anaerobes– anaerobe not killed by prolonged exposure to oxygen – example: Clostridium tertium
• Lag Phase - >24 hrs old, growth slowing, not appropriate for biochemical or susceptibility testing
• Log Phase – Exponential growth – appropriate for all testing• Stationary phase – appropriate for transporting specimens

Specimen collectionfor Aerobic Bacteriology
Throat / Wound collected using swab1. Swab placed in Stuart’s or Aimes transport media buffer
solution with peptones – 2. Preserve viability but not promote growth of bacteria3. Swabs made of polyester or sponge like material (not
cotton) – cotton traps organisms
Urine1. Boric acid to induce stationary phase2. Refrigerate within one hour, Specimen stable for 24 hours
• Purpose to maintain original colony count• Maintain viability of organisms

Gram stain
10 seconds-1 minute
Primary stain
Mordant 10 seconds-1 minuteRinse
5-10 seconds
Rinse
Decolorization
Counter
Counter stain10 seconds-1 minute

Gram positive cocciin pairs and chains Streptococcus
Gram negative bacillusMost likely anEnteric
Gram positive rodmost likely a Bacillus species
Gram positive cocci in clusters, Staphylococcus
Gram negative rod – fusiformShaped - Fusobacterium
Some Gram stains toRemember!!!

Gram stain is used to assess quality of Sputum specimen for culture
• Expectorated sputum specimen is rejected for bacterial culture if actually “spit”:– Perform Gram stain of sputum specimen – If >= 25 epithelial cells /field – Sputum is judged to be spit / not a sputum specimen– Bacterial culture is not performed / it is rejected– Request made for a new “deep cough” specimen
Bad Sputum Good Sputum
10X objective 10X objective

Most used Agar Media in Bacteriology
Blood agar- 5% sheep’s blood agar gauge hemolytic reaction of bacteria (alpha, beta, gamma)Grow variety of Gram positive & Gram negative bacteria and Yeast
Chocolate agar – “cooked” blood agar – more enriched than blood agarEverything blood agar can grow Plus more fastidious bacterialike Haemophilus influenzae and Neisseria gonorrhoeae

Most used agar media in Bacteriology
• MacConkey agar – Supports the growth of Gram negative bacilli only (crystal violet inhibits Gram positive organisms)Selective (only GNR) and Differential (Lactose fermentation)Lactose fermentation = pink (neutral red indicator)non-lactose fermentation = no color
• After media is plated incubated in aerobic and/or CO2 incubators at 35˚ C for 24 – 72 hours

Gram Positive Cocci
StaphylococcusStreptococcus Enterococcus

StaphylococcusGram positive cocci
clusters
All Staphylococcus are Positive for Catalase Enzyme
Staphylococcus aureus Coagulase Negative StaphCoagulase Enzyme Positive Coagulase Enzyme Negative
+/- Yellow colonyBeta hemolytic
White colonyMost not hemolytic

Catalase Enzyme ReactionNegative Positive
Hydrogen Peroxide plus bacteria
Avoid blood agar – blood has innate catalase activity and will give false positive reaction

Rabbit plasma inoculated with organismIncubate at 35˚C
Read at 4 hours and if negative read again at 24 hours
Negative tube coagulase =no clotCoagulase negative Staph
Positive tube coagulase [at 4 or 24 hrs] = Clot
Staph aureus
Tube Coagulase Reaction

Slide Agglutination Test to identify Staphylococcus aureus
• Clumping factor and protein A is found on the S. aureus cell wall.• Fibrinogen and IgG to protein A is on the surface of the Staphaurex latex beads• S. aureus will clump in the Staphaurex latex bead solution and• positively identifies Staphylococcus aureus.• Coagulase negative Staphylococcus species remain milky and do not clump in • the solution.•Advantage over tube coagulase – reaction time is 30 seconds vs. 24 hours
clumping
No clumping

Staphylococcus aureus • Primary virulence factor:
– Protein A – surface protein, ability to bind immunoglobulin and combat the immune response
• Diseases and associated toxin: – Toxic shock syndrome (TSST-1 toxin)– Scalded skin syndrome (Exfoliatin (SSS) toxin)– Soft tissue infection (Panton valentine leucocidin toxin – PVL)– Septic arthritis – primary cause– Food poisoning (Enterotoxins) – Bacteremia and endocarditis

Susceptibility issues –(1) MRSA• Methicillin Resistance (MRSA =Methicillin resistant S. aureus)
– Penicillin binding protein (PBP) produced by the mec A gene codes for resistance to oxacillin/methicillin/penicillin
– All MRSA are considered resistant to the cephalosporin antibiotics– Cefoxitin susceptibility testing is a more sensitive indicator of
resistance and provides better detection of MRSA than oxacillin testing. Shown is a Kirby Bauer (KB) disk test that is resistant to cefoxitin.

(2) The “D” Test for Clindamycin• To accurately determine if Staph aureus/MRSA is susceptible To accurately determine if Staph aureus/MRSA is susceptible
to Clindamycinto Clindamycin• During therapy, S aureus isolates resistant to Erythromycin During therapy, S aureus isolates resistant to Erythromycin
possess enzymes capable of inducing Clindamycin to become possess enzymes capable of inducing Clindamycin to become resistant and therefore not useful for therapy.resistant and therefore not useful for therapy.
• Kirby Bauer zone around Clindamycin will be blunted to form Kirby Bauer zone around Clindamycin will be blunted to form a D if Clindamycin can be induced by Erythromycin to be a D if Clindamycin can be induced by Erythromycin to be resistant – so called INDUCIBLE RESISTANCE. resistant – so called INDUCIBLE RESISTANCE.
• Clindamycin should be reported as resistant by clindamycin Clindamycin should be reported as resistant by clindamycin induction and not used for therapy.induction and not used for therapy.
D test positiveInducible resistance
D test negativeClindamycin canbe used for therapy

Nares is the colonization site for MRSA and the most common surveillance site for cultures.Hospitals have surveillance programs to prevent nosocomial spread of MRSA.
ChromAgar can be used to detect MRSA. It is a selective and differential medium with chromogenic substrates that turn specific colors for Staph aureus. Cefoxitin is added to the medium to detect methicillin resistant Staph aureus (MRSA)
Molecular assays (MA) can also be used to screen nares for MRSA. MAs increas sensitivity of detection (@5-10%) and increase laboratory costs.
Staphylococcus aureus (MRSA)Hospital Epidemiology Issue:Nasal surveillance for MRSA

Coagulase negative Staph (CNS)@ 15 species infect humans
• Staph epidermidis – is the most common– Major aerobic component of normal skin flora – Common cause of subacute bacterial endocarditis – Pathogenicity from cell adhesion factors forming biofilm on biologics and plastic
• Staph saprophyticus – – Urinary tract infections in the child bearing age female, – This species of CNS adheres in greater #’s to epithelial cells– Novobiocin resistant by KB disk test can be used as test to identify
Staph saprophyticus
White non-hemolyticcolony
resistant

CNS & Related Cocci• Staph hemolyticus –
– Can cause line related sepsis– This CNS is hemolytic on blood agar– Do not confuse with Staph aureus
• Staph lugdunensis– The PYR test is positive and used to identify– Perhaps greater pathogenicity than other species
• Micrococcus species– Mustard yellow colored colony– Catalase positive / Gram positive cocci tetrads– Tube coagulase negative – Does not ferment glucose
• Staphylococcus ferments glucose– Environmental contaminate
Pos Neg

Streptococcus
Gram positive cocci in chains and or pairs Catalase enzyme negativeGrouped by hemolytic pattern on 5% sheep’s blood agar
– Alpha – greening of agar, partial hemolysis of rbc• Viridans Strep, Strep pneumoniae,
Granulicatella/Abiotrophia– Beta – clearing of agar, complete hemolysis of rbc
• Beta hemolytic Strep groups A - G– Gamma – no clearing of agar
• Streptococcus bovis

Beta hemolytic Streptococcus
• Grouping of the Beta Streptococcus use the “C” carbohydrate in the cell wall of the bacteria
• Identifies the Beta Strep groups – A, B, C, F, and G that cause infections in humans.
• The Lancefield grouping system uses the “C” CHO in the cell wall (antigen) in a slide agglutination reaction with purchased monoclonal antibody attached to latex beads
See below slide for a positive and negative reaction.• Immunologic typing is more accurate than biochemical
testing to group Streptococcus
+-

Streptococcus pyogenes• Strep pyogenes – genus/species for Group A beta Streptococcus [GAS]
– Bacitracin KB sensitivity test – inhibited, no growth @ disk– This test is not specific for Group A , it x-reacts with group C– “A” disk is the Bacitracin disk
– PYR (pyrrolidonyl arylmidase) reaction• Organism spotted on moist disk• 2 min – RT incubation• Add Cinnamaldehyde reagent• Look for color reaction• Pink = positive = Strep pyogenes• This test is not exclusive for Strep pyogenes – Enterococcus and
Staph lugdunensis are also positive for PYR
– No resistance to Penicillin or Cephalosporin antibiotics

– Streptolysin O and Streptolysin S toxins • Comprise the ASO titer• Cell toxins lead to evasion from the immune system• O toxin is oxygen labile S toxin is oxygen stable• When both are active - most hemolysis occurs in the 5% Sheep’s blood
agar
Primary virulence factors:
M Protein – preventsphagocytosis
Capsule – hyaluronic capsule protects from phagocytosis

Strep pyogenes diseases
• Diseases – – Pharyngitis– Impetigo (1)– Erysipelas (2)– Cellulitis (3) – Necrotizing fascitis (4)– Puerperal sepsis– Toxic Shock– Scarlet fever (5)
1
2
3
45

Sequelae of Strep pyogenes infections
• Rheumatic fever– Caused by inadequately treated Strep throat– Rise in the 1990s due to EIA tests being used as the only diagnostic test for
pharyngitis – EIA tests are not very sensitive – and led to children not receiving antimicrobial therapy
– All negative EIA specimens on children should be confirmed by culture– Similarity between the proteins of the Strep A and muscle tissue cause immune
system confusion– Immune system attacks the heart, joint and bones and causing inflammation – can
lead to valve replacement surgery– Anti-streptolysin O measures the amount of antibodies against Streptococcus group
A in the serum• Glomerulonephritis
– 10-14 days following skin infection or pharyngitis– Renal disease with inflammation of the glomeruli– ASO titers will be positive– Usually resolves with therapy

Streptococcus agalactiae (Group B)Lancefield agglutination test demonstrates “B” cell wall CHO
Biochemical tests for identification:Camp test – performed using a Staph aureus strain with Camp
factor perpendicular to group B Strep, incubate 24 hr. intensifies toxin and produces arrow shaped hemolysis
Rapid hippurate hydrolysis4 hr test for identification of GBSHippurate disk incubated with Group B StrepAdd ninhydrin reagent for color formation
Positive/Purple
pos
Arrow-like
Staph aureus
Strep group B

Strep agalactiaeGroup B Streptococcus [GBS]
• Pathogen of neonate – associated with in utero or perinatal organism acquisition during birthing process – Early onset – within 7 days – Late 7 – 28 days from birth process.
• Pregnant women carry organism in the cervix and/or rectal area. All should be tested at 35 – 37 weeks of pregnancy.– Enrichment methods for GBS is standard of practice and must be used
• Swab placed into LIM broth – incubate for 18 hours at 35 ˚C then subculture onto agar media. This broth can also be used as an enrichment method followed by molecular testing.
• Carrot enrichment broth turns orange with growth of group B Strep
• GBS is also a pathogen of the elderly – causes bacteremia & UTI
• Susceptible to Penicillins and Cephalosporins
Carrot Broth

It used to be Streptococcus bovis Taxon update – 1) Streptococcus gallolyticus ssp. gallolyticus (formerly S. bovis biotype 1) associated with colonic cancer and endocarditis 2) Strep gallolyticus ssp. pasteurianus (formerly S. bovis biotype II) associated with neonatal meningitis Identification for S. gallolyticus (both ssp)
Bile esculin slant – positive (turns black)
6.5% NaCl – no growth
PYR reaction - negative
• Susceptible to Penicillin

• Two most common species E. faecium and E. faecalis• No well defined virulence factors• Possesses the Group D CHO in the cell wall
• Biochemical tests:– Bile esculin positive – growth and black precipitin– Growth in 6.5% salt– PYR positive (Group A beta Strep and Staph
lugdunensis also positive)*– E. faecium = arabinose fermentation positive – E. faecalis = arabinose fermentation negative
Enterococcus
Bile esculin
PYR
+ -
Neg Pos
Neg Pos
6.5% Salt

Enterococcus• Cause a variety of infections and is a pathogen of opportunity• Normal flora in the intestine• Cause UTI, bacteremia, and abdominal infections• Antimicrobial therapy:
– Natural resistance to cephalosporins– Ampicillin/Aminoglycoside can be synergistic for therapy in cases of
endocarditis
• Unusual susceptibility issues – Acquired resistance to vancomycin known as vancomycin resistant
enterococcus [VRE]• Van A (E. faecium) resistance genes• Van B (E. faecalis) resistance genes

Alpha hemolytic Streptococcus
Streptococcus pneumoniaeGram stain = gram positive bullet shaped cocci with capsule Polysaccharide capsule = virulence factor
Identification:– Bile soluble – colonies dissolve in sodium deoxycholate (bile salts)– Optochin sensitive – 14mm or greater zone of inhibition around the
6mm optochin disk
Inhibition >=14mm
NOInhibition
Colonies dissolved

Streptococcus pneumoniae• Upper and Lower respiratory tract, sepsis and meningitis • Prevent invasive disease with multi-serotype vaccine• Acquired Resistance to Penicillin due to Penicillin binding
proteins (PBP) • Minimum inhibitory concentration (MIC) testing necessary to
detect resistance to penicillin – in broth or Etest • Testing of CSF isolate:
– Penicillin R = >2 mcg/ml• Resistance to Penicillin• Cefotaxime 2nd drug of choice
Etest for Cefotaxime
MIC

Viridans Streptococcus
Several species of alpha hemolytic Streptococcus found as NF in mouth and upper respiratory tractS. mutans S. salivarius S. sanguis S. mitis
• Bile esculin slant negative• Not bile soluble• Optochin resistant - <=13 mm • Cause 30 – 40% cases of sub acute endocarditis / native valve• Can cause abscesses and various infections throughout the
body especially in the immune suppressed host• Variable susceptibility patterns, some isolates with elevated
MICs to Penicillin
Viridans Streptococcus

Viridans Streptococcus
• The Streptococcus anginosis group– S. anginosus S. constellatus S. intermedius
• Normal flora in human mouth• More virulent than “normal” viridans
Streptococcus, perhaps due to capsule• Cause deep tissue abscesses, bacteremia,
endocarditis, intra abdominal infections…• Variable susceptibilities – so need to test

Nutritionally Variant Streptococcus• Vitamin B6 (pyridoxal) deficient – so will not grow on BAP without B6
• Will grow in a patient blood culture bottle due to patient’s vit B6 in blood• but not on the subculture 5% Sheep’s blood agar plate ( no vit B6)• Requires streak of Staph aureus that supplies vitamin B6 • Nutritionally variant Strep will satellite @ S. aureus (see pix)
• There are 2 species– Abiotrophia – Granulicatella
• Endocarditis – – More destructive to valve than
than “normal” viridans Strep– Higher MIC’s to Pen or R
Satellite streptococcus

Gram Negative Cocci
NeisseriaMoraxella

Gram Negative Cocci• Neisseria species and Moraxella catarrhalis– Small kidney bean shaped cocci in pairs– Oxidase enzyme positive
• CTA (Cysteine Trypticase agar) carbohydrate fermentations are used for identification – glucose, maltose, lactose, sucrose– N. gonorrhoeae Gluc + Mal - Lac - Suc -– N. meningitidis Gluc + Mal + Lac - Suc -– N. lactamica Gluc + Mal + Lac+ Suc-– M. catarrhalis all negative Dna’ase +

Neisseria speciesgram negative diplococcus – intra and
extra cellular
Acinetobacter species –Cocci are more round and not usually in pairs – normal flora in femalegenital tract

Miniature CHO fermentation reactions for Neisseria and Moraxella catarrhalis
Compare (+) reactions to negative (red) control well
+
+ +
Oxidase enzyme spot test:Detects presence of enzyme cytochromeoxidase Add reagentN,N dimethyl-p-phylenediamine oxalateto filter paper with organism positive = purple/ blue
control
Full size tube CHO fermentation test

Neisseria meningitidis• Meningitis primarily in children and young adults• Hallmark is petechiae (organisms crowd capillaries) – can lead
to tissue necrosis and DIC – infection can be rapidly fatal• Carriage in Nasopharynx/ Susceptible to Penicillin• Capsular polysaccharide is the primary virulence factor• Complement deficiencies in 7,8,and 9 can predispose to
chronic type disease• Adrenal necrosis is referred to Waterhouse Friederichsen syndrome• Type C is the current endemic strain in the USA – 1*problem
in college Freshmen living in dorm• Immunization available for all serotypes except serogoup B

Neisseria gonorrhoeae– Acute urethritis, endocervix, ocular, rectal, oropharynx– 10 – 20 % female ascend to PID but only 0.5% disseminate– Gram stain of urethral discharge useful for male diagnosis– Gram stain of cervix not specific for females– Transport for culture – charcoal swabs, No refrigeration– Medium of choice: Thayer Martin or Martin Lewis– Amplification methods [PCR] increases sensitivity of detection and superior to culture – Produces a beta lactamase enzyme and also Chromosomal resistance
– Therapy: Ceftriaxone + Azithromycin or Doxycycline to prevent
– resistance – currently an important issue!

Moraxella catarrhalis• Pneumonia, ocular, sinusitis, otitis media• Gram stain of sputum can be helpful in
diagnosis of pneumonia– Polys with gram negative diplococci
• Hockey puck colony – able to push around on agar surface– oxidase enzyme positive– DNA’ase enzyme positive– Resistant to ampicillin by beta lactamase enzyme
production

Gram Positive Rods
CorynebacteriaBacillusListeria
Erysipelothrix

Corynebacterium• Corynebacterium species are:
– Catalase +, – Diphtheroid morphology (Chinese letter forms)– no spores are produced
• C. diphtheriae – agent of Diphtheria– Diphtheritic pseudo membrane produced and adherent in throat– Phage mediated toxin is distributed from the membrane causing respiratory paralysis – Toxin detected by Elek immunoprecipitation procedure– Grows well on 5% Sheep’s BAP– Selective media Cysteine tellurite agar
Produces black colonies with brown halos
– Grown on egg containing Loeffler medium then stain with methylene blue to look for metachromatic granules that are colorful granules characteristic of C. diphtheria
Elek plate

Other Corynebacterium• Corynebacterium jeikeium – – normal skin flora bacteria / thrives on lipid – Infects patients with plastic catheters and indwelling
devices by tunneling into the device from the skin– Biofilms are formed on the plastic, protecting the
organism from antibiotic therapy– Very resistant to most antibiotics– Susceptible to vancomycin and tetracycline only
• Corynebacterium urealyticum – – Rapidly urease positive diphtheroid– Urinary tract infection in post renal transplants – Resistant to many antibiotics – vancomycin susceptible
Red is (+)Urease reaction

Bacillus speciesLarge gram positive rod – boxcar shaped with square endsCan over-decolorize easily and appear reddishSpores produced – causes clearing in rodCatalase enzyme positive
Bacillus anthracis - Agent of AnthraxNatural infection of herbivores Skin, pulmonary, GI and CSF infectionsUnique black eschar skin lesions Bioterrorism - effective due to highly resistant spores that can be easily disseminated into
the environment

BacillusBacillus anthracis culture: medusa head colonies on BAP
non-hemolytic on 5% Sheep’s blood agarnon-motile Penicillin susceptibleWith these reactions – contact public healthdepartment for assistance with identification
Bacillus cereus – food poisoning with rapid onset (1 – 6 hr) of vomitingPreformed emetic toxin in food Fried rice is one of the most common food sourcesbeta hemolytic colony on Sheep’s blood agar and motile

Listeria monocytogenesSmall gram positive rod
Catalase positive / No spores producedSubtle beta hemolysis on Blood agar Tumbling motility on wet mountUmbrella motility in tube media More motile at 25˚C than 35˚CCold loving – grows well at 4˚C and the reason it is abundant in refrigerated foodsFound in dairy products and deli case meatsInfections: Bacteremia in pregnant women and can induce still birthsBacteremia and CNS in immune suppressed
Ampicillin is drug of choice/ resistant to Cephalosporins

Erysipelothrix rhusiopathiae
Small gram positive rodCatalase negativeAlpha hemolytic colony
Only G+R that produces hydrogen sulfide (H2S) in a TSI agar
Human skin infection acquired from swine erysipelas or poultry and is most common in butchers
Uncommon isolate in human blood cultures most common in drug addicts
high % of endocarditis with extensive damage to valveIntrinsically resistant to Vancomycin
H2S production on Triple sugar iron agar (TSI)

Gram negative bacilli
EntericsNon fermenters
Fastidious

Gram negative cell Wall
Rod shaped
Simple flow chartIdentification
Strategy
Enteric Gram Negative Rod
Ferment GlucoseFerment LactoseEx. Escherichia
coli
Enteric GramNegative Rod
Ferment GlucoseDo NOT ferment
LactoseEx. Proteus species
Gram negative BacilliDo NOT ferment
GlucoseDo not ferment
LactosePositive Oxidase
PseudomonasBurkholderia
Gram negative BacilliDo NOT ferment
GlucoseDo NOT ferment
LactoseNegative Oxidase
AcinetobacterStenotrophomonas
EnterobacteriaceaeEnteric Gram Negative BacilliFerment glucoseAlmost all are oxidase negativeNitrate reduced to nitrates
Non fermentersGlucose is not fermentedOxidase positive and negativespecies

Enterics that Ferment Glucose• Escherichia coli
– Major aerobic NF in intestine– #1 cause of UTI– Common in abdominal infections and bacteremia– Indole reaction is positive
• Enterobacter species– Enterobacter cloacae and E. aerogenes most common– Environmental organism with low pathogenicity– Enterobacter sakasaki associated with neonatal meningitis
• Klebsiella species – K. pneumoniae most common– Mucoid colony– Currant jelly sputum in alcoholics due to blood mixed with capsular
polysaccharide in sputum
Green sheen onEMB agar
Mucoid colony
Indole positive =Robin’s egg blue

Enterics that do NOT ferment lactose!No lactose fermentation = No color produced on Macconkey agar
• Proteus species Swarming colonies in layers on agar surface
• Indole positive – Proteus vulgaris• Indole negative – Proteus mirabilis
• Serratia marcescens – Red pigment produced and intensifies at room temp– Infections in immune suppressed– Ventilator associated pneumoniae– Bacteremia

Gram negative bacillus MacConkey agar
Lactose fermenter
Lactose non fermenter
Gram stain enteric bacilli – plump
No lactosefermentation
Lactose fermentation

Glu/lac/suc fermentedwith gas
Glucosefermentedonly
Glucosefermentedwith H2S
No CHO fermentationNon fermenter
Triple Sugar Iron Agar – detect fermentation of glucose, lactose and/ or Sucrose and the production of hydrogen sulfide [H2S]

Extended Spectrum Beta Lactamase Extended Spectrum Beta Lactamase Enzymes - “ESBL” Enzymes - “ESBL”
• ESBL enzymes are produced by numerous gram negative rodsESBL enzymes are produced by numerous gram negative rods– Confer resistance to Cephalosporins and synthetic PenicillinsConfer resistance to Cephalosporins and synthetic Penicillins
• Plasmid mediated Tem 1 beta lactamase is the most common Plasmid mediated Tem 1 beta lactamase is the most common enzyme producedenzyme produced– Possible plasmid dissemination makes this an infection control issuePossible plasmid dissemination makes this an infection control issue
• Detect presence of ESBL in a gram negative rodDetect presence of ESBL in a gram negative rod– Double disk test Double disk test – MIC breakpoints for the cephalosporins are set at very low MIC values to MIC breakpoints for the cephalosporins are set at very low MIC values to
catch subtle resistance catch subtle resistance
• ESBL producing GNR are treated with:ESBL producing GNR are treated with:– Imipenem [Carbapenemases]Imipenem [Carbapenemases]
– Piperacillin/Tazobactam which blocks beta lactamase enzyme functionPiperacillin/Tazobactam which blocks beta lactamase enzyme function

Typical ESBL Susceptibility PatternTypical ESBL Susceptibility Pattern• Escherichia coliEscherichia coli
– Ampicillin RAmpicillin R– Cefazolin RCefazolin R– Gentamicin RGentamicin R– Cefotetan Cefotetan S S (Cephamycins are not cephalosporins)**(Cephamycins are not cephalosporins)**– Amikacin SAmikacin S– Ceftazidime RCeftazidime R– Cefpodoxime R Cefpodoxime R – Piperacillin RPiperacillin R– Pip/Tazobactam SPip/Tazobactam S (Tazobactam is a Beta lactam blocker)(Tazobactam is a Beta lactam blocker)– Imipenem SImipenem S
Double disk test – demonstrates how the beta lactam blockers [clavulanate] can stop the beta lactamase activity
Cephalosporin
Cephalosporin +Clavulanate

Carbapenemase enzymes are most commonly produced by Klebsiella pneumonia and known as KPC which stands for K. pneumoniae carbapenemase however, they have been found in many genera of enteric gram negative rodsResistant to all carbapenem antibiotics - imipenem, meropenem, ertapenem, doripenem
CRE have cross resistance to virtually all antibiotic classes - Polymyxins [colistin, polymyxin B] used for therapy - High fatality rates associated with infectionsOther resistance mechanisms:New Delhi metallo-beta lactamase [NDM-1] enzymes – resistant to all drug classes including carbapenems
Carbapenemase Enzyme producing Enterics [CRE] and NDM-1 Enzyme

Salmonella species• Salmonella spp.
– Diarrhea with +/- fever – polys in the stool– Infection from food ingestion – must ingest large #’s of
organisms to make you ill (1,00,000 bacteria)– Eggs, meats and contaminated uncooked vegetables– Does not ferment lactose/ produces Hydrogen sulfide– Selective agars: SS and Hektoen– Identification based on biochemical reactions to get to genus
and serologic typing “Kaufman White typing scheme” to get to species
– O Somatic (cell wall) antigen – Salmonella group B– H flagellar antigens – 2 phases [h1 & h2] speciates the
Salmonella – ie Salmonella enteritidis– Vi capsular antigen – Found in S. typhi only

Salmonella Shigella Agar (SS agar) Salmonella and Shigella are colorless because they do not ferment lactose
Hektoen agar – Salmonella produces H2S [Hydrogen sulfide] turning the colonies blackNormal flora – orange colored due to fermentation of lactose

Salmonella typhi• Typhoid fever – fever, sepsis, high fatality rate
• Vi capsular antigen surrounds the D cell wall antigen• Boil solution of organism for 15 minutes to destroy the
Vi capsular antigen and expose the cell wall antigen D• Serotyping can then be performed for the D antigen• Moustache of H2S in the TSI tube
– Carrier state in gallbladder– Ingest organism, clears the bowel– In @ 1 week then enters– Blood stream & Bone Marrow

Shigella• Diarrhea, +/-vomiting, fluid loss, polys and blood in stool
[10%], tenesmus• Human to human transmission • Low #’s of organisms to make you ill [10 – 100 bacteria]• Non motile and No H2S produced (differ from
Salmonella)• Does not ferment lactose • 4 species based on somatic antigen – S. boydii Group C– S. dysenteriae Group A– S. flexneri Group B– S. sonnei Group D

Yersinia enterocolitica
• Diarrhea• Major reservoir – swine• Human usually infected by non pasteurized milk• Causes septicemia in iron overload syndromes• Unique infection Mesenteric adenitis – RLQ pain
which mimics appendicitis• Grows well at 4*C (like Listeria)• CIN agar (Cefsulodin-irgasan-novobiocin)• Has been associated banked blood infections related
to Transfusion of infected products

Yersinia pestis - Plague
• Possible organism of bioterrorism• Obligate flea/ rodent/ flea cycle • Infected Flea bite - leads to Bubonic form/ painful buboes (lymph node swelling)• Pneumonic form- bacteremic spread or
patient to patient fatality >=50%• Southwestern part of USA• Grows on BAP, • catalase +, oxidase -• Bipolar staining “safety pin”

Enteric Glucose Fermentersthat are Oxidase +
• Vibrio cholerae– Rice water stool produced due to mucus flecks in diarrhea – Virulence is due to Toxin – receptor on the epithelial cell –
activates adenylate cyclase – increases cAMP – hyper secretion of NaCl and H20 – death from dehydration
– It is a Halophilic bacteria which means it is a salt loving organisms, 1% salt actually enhances growth
– Selective media – TCBS = thio citrate bile sucrose agar, colony turns yellow due to sucrose fermentation
– 01 most virulent due to high production of toxin
TCBS AGAR

Classic Gram Negative Rod Gram Stains
Campylobacter
Vibrio species
Enteric gram negative rod
Sea gull wings C shaped
Plumb and rectangular

Other Vibrio species
Vibrio parahaemolyticus• Colony on TCBS medium is green – sucrose negative• Diarrhea from ingestion of raw fish and shellfish
• Vibrio vulnificus• Very virulent Vibrio species – infection leads to formation of
painful skin lesions with muscle necrosis on lower extremities• Most prevalent in patients with pre existing liver disease • 50% fatality rate even if treated• Ingestion of raw oysters and shellfish from coastal waters• Green or yellow colonies TCBS

Do not ferment Glucose Oxidase negative
• Acinetobacter – hospital environment and human skin– Major nosocomial pathogen – Acquires antibiotic resistance with pressure– Gram negative cocco-baccilli – big cocci– Acinetobacter baumannii – glucose oxidizer– Acinetobacter lwoffi – glucose non oxidizer
• Stenotrophomonas maltophilia – Rapid maltose oxidizer– Long Gram negative bacillus– Naturally resistant to many antibiotics– Nosocomial pathogen – super-colonizer when on long term Imipenem
therapy because Stenotrophomonas is naturally resistant to Imipenem

Glucose non-fermenterOxidase Positive
Pseudomonas aeruginosa • Fluorescent pigment and blue-green pigment (pyocyanin)• Grape like odor • Growth at 42˚C
Ps fluorescens/putida – no growth at 42*• Major pathogen in cystic fibrosis
– Mucoid strains– in combination with Burkholderia cepacia can cause major lung damage
• Nosocomial pathogen – associated with water

Glucose Non Fermenters/oxidase +
• Burkholderia cepacia– Dry , yellow colony – oxidase negative– Problem organism in cystic fibrosis
• Flavobacterium (Chryseobacterium) meningiosepticum– Associated with fatal septicemia in the neonate– Low virulence– Environmental source

Haemophilus speciesHaemophilus influenza– Causes a variety of infections
• Pneumonia, meningitis, otitis media, ocular– Two nutritional factors for growth
• X = hemin• V= NAD (nicotinamide adenine dinucleotide)• Demonstrate by satellite phenomenon or X/V strips (slide 74)
– Grows on chocolate agar – Will not grow on 5% sheep’s blood agar– Requires high level C0₂ [5 – 8%] for growth– Resistance to Ampicillin by beta lactamase production [15-
20 %]
+

Disk test for Beta lactamase Disk test for Beta lactamase DetectionDetection
• Add bacteria to filter paper impregnated with Nitrocefin or Add bacteria to filter paper impregnated with Nitrocefin or Cefinase test (yellow colored/chromogenic cephalosporin)Cefinase test (yellow colored/chromogenic cephalosporin)
• Incubate at room temp (30 sec - 60 min) depending on Incubate at room temp (30 sec - 60 min) depending on bacteria being testedbacteria being tested
• Positive result is color change from Positive result is color change from yellow to redyellow to red - beta - beta lactamase enzyme breaks down beta lactam ring to form lactamase enzyme breaks down beta lactam ring to form hydrolyzed red end producthydrolyzed red end product
• Detects resistance to Amp/Pen/Cephalosporin in Detects resistance to Amp/Pen/Cephalosporin in Haemophilus, N. gonorrhoea , Moraxella catarrhalis, and Haemophilus, N. gonorrhoea , Moraxella catarrhalis, and anaerobic gram negative rodsanaerobic gram negative rods

Haemophilus species• H. parainfluenza – – requires V factor only– Normal flora in the upper respiratory tract– One of the HACEK organisms of endocarditis
• H. (Aggregatibacter) aphrophilus – – No factor requirements for growth– Infections: abscesses (liver, lung, brain) & endocarditis
• H. ducreyi – – Requires X factor– Cause of Chancroid - venereal disease– “school of fish” appearance on stains

Satellite phenomena
Demonstrates need for X and V factor

HACEK group
• Oral flora that can become pathogens of endocarditis usually caused by dental procedures
• Require 2-4 days to grow in patient blood cultures• Haemophilus species = oxidase neg, catalase neg • Actinobacillus actinomycetom-comitans = oxidase
neg, catalase pos• Cardiobacterium hominis = oxidase pos• Eikinella corrodens = oxidase pos, colony pits BAP• Kingella kingii = oxidase pos, hemolytic on BAP, also
cause infections in small children (septic joints)

Bordetella pertussisWhooping cough – three stages of disease
• (1)Prodromal – flu like disease – most contagious stage• (2) Catarrhal - cough with classic whoop in small children• (3) Paroxysmal - recovery phase• Gram = Tiny gram negative coccobacillus• Inhabits Nasopharynx• Harsh cough caused by toxin adhering to bronchial epithelial
cells, can last for months, especially deadly to young children• PCR for diagnosis – most sensitive and specific • Charcoal containing media for transport and culture – Regan
Lowe Charcoal agar • Reservoir for infection – adults due to waning immunity• Outbreaks due to lack of vaccination of children and adults

Pasteurella multocida
Primary cause of Cat and Dog bite wound infectionsCan also cause pneumonia from close animal contactInfections can disseminate to blood streamFound as normal flora animal’s mouthSmall gram negative coccobacilliGrowth on 5% Sheep’s blood agarWill not grow MacConkey agar (big clue)Oxidase PositiveOne of very few Gram negative rods sensitive to penicillin

Capnocytophaga• Fusiform shaped gram negative rods – very pleomorphic
Gliding motility, fingerlike projections from colonies• Oxidase negative, Catalase negative• C. canimorsus – dog bites with bacteremia – high% of
infections lead to endocarditis
• Other Capnocytophaga species normal flora in the human mouth and
• Can infect mouth ulcers induced by chemotherapy – this becomes route of entry into bloodstream

Brucella species
• Disease – Fever of unknown origin, significant joint pain• Small gram negative coccobacilli – slow and difficult to grow in blood
cultures– Castaneda biphasic blood culture held for 21 days [old school]– Current: Automated Blood culture systems grow within 5 days
• Specimens: blood and bone marrow most profitable– Granuloma formation in bone marrow
• Serology can be used for genera/species diagnosis• Brucella species in clinical specimen related to animal
species the patient was exposed: – B. abortus – ingestion of raw cow milk– B. melitensis – ingestion raw goat milk, feta cheese– B. suis – contact with pigs B. canis - contact with dogs
Granuloma in bone marrow

Campylobacter• Small curved bacilli –
shaped like sea gull wings• C. jejuni – agent of diarrhea
– Related to undercooked poultry ingestion– Requires selective media containing antibiotics -Skirrow’s blood agar– Thrives at 42˚C - can use to selectively culture Campylobacter– Requires microaerophilic atmosphere (high CO₂, low O₂)– Significant % Guillain-Barre syndrome as sequelae
C fetus – Bacteremia in the immune suppressed host / does not cause diarrheal disease
C. jejuni – grows at 37˚C and 42˚, hippurate positiveC. fetus - grows at 37˚C and 25˚C hippurate
negative

Reservoir – rabbits, rodents, ticks and flies. Humans infected by bug bites or directly from exposure to animal blood
Strongly associated with skinning rabbits with bare handsBacteria can penetrate small breaks in skin:
cause painful skin lesions – enlarged lymph nodes –
leading to bacteremia (ulcerogladular tularemia) Pneumonia
Great hazard to lab workersFastidious small gram negative cocco-bacillusCulture media requires cysteine*
Francisella tularensis

Helicobacter pylori
• Small curved bacilli• Cause of acute gastritis• Rapidly!! And strongly urease positive – used for detection
directly from antral biopsy tissue• Difficult to grow in culture• Stool antigen – diagnose and test of cure• Serum antibody can aid in diagnosis and avoid biopsy

Legionella
Legionella pneumophila most common [6 serotypes]• Requires cysteine in media for growth • Media of choice Buffered Charcoal Yeast Extract agar
with colonies forming in 3-5 days• Does not stain with gram stain in direct specimens • Use silver impregnation stains in tissue • Pulmonary disease associated with water,
cooling towers, shower heads, stagnant water• Urinary antigen test to detect L. pneumophila type I infection• Treatment: Erythromycin (macrolide)

Bacteria without cell walls• Mycoplasma and Ureaplasma – have cell membranes only! Media and
transport must contain sterols to protect the membrane to promote survival and growth
• Do not form discreet colonies on agar plates – must read plates under a microscope to visualize organisms
• PCR is becoming the detection method of choice since culture is cumbersome and slow (3 – 14 days)
• M. pneumoniae –– community acquired pneumonia– Serology and PCR for diagnosis
• Genital mycoplasmas– M. hominis – fried egg colony, vaginitis, cervicitis, postpartum sepsis,
neonatal infections , pre rupture of membranes– Ureaplasma urealyticum – rapid urea hydrolysis in broth, NGU & upper
genital tract infection, spontaneous abortion, neonatal infections
Ureaplasma
Mycoplasma hominis

Difficult to grow• Bartonella henselae – Diagnose be PCR and/or serology
– Cat scratch disease – exposure to cat and cat boxes (excrement)– Bacillary angiomatosis – vascular skin lesion +/- invasion / HIV
• Bartonella quintana – cause of trench fever/ vector is the body louse/Diagnose by Serology
• C. trachomatis Serovars L1,L2,& L3 cause of Lymphogranuloma venereum– Serology / clinical findings – lymphatics and lymph nodes involved
• C. pneumoniae (TWAR agent)- Pneumonia, Diagnose by PCR• C. psittaci- psittacosis, pneumonia, exotic parrot exposure/ Serology and epidemiology• Chlamydiae trachomatis
– trachoma - eye infection

Molecular Testing for Neisseria gonorrhoeae Molecular Testing for Neisseria gonorrhoeae and Chlamydia trachomatisand Chlamydia trachomatis
• Amplification of DNA by Polymerase Chain Reaction (PCR)Amplification of DNA by Polymerase Chain Reaction (PCR)– Urine, Cervix, and urethral most often testedUrine, Cervix, and urethral most often tested– More sensitive than any culture based systemMore sensitive than any culture based system• Sensitivity/Specificity @ 96%/99%Sensitivity/Specificity @ 96%/99%• Females most sensitive specimen = cervixFemales most sensitive specimen = cervix• Males good sensitivity with urine / equal to urethralMales good sensitivity with urine / equal to urethral
• Has replaced culture methods as “Gold” standard of detectionHas replaced culture methods as “Gold” standard of detection
Iodine staining of inclusions fromCulture method
Elementary bodies from infected cells using Fluorescent antibody stain

More difficult to grow
• Ehrlichiosis – – Obligate intracellular pathogen– Anaplasma, inclusion in the PMN– Ehrlichia inclusion in the Monocytes– Vector = tick bite– fever, leukopenia, thrombocytopenia, – elevated serum aminotransferases,– no rash (differs Rocky Mountain Spotted Fever)
• Found in the south central, southeast , midwest USA• PCR and serology for diagnosis

Spirochetes
• Borrelia burgdorferi - Lyme’s disease– Primarily found in NE part of USA– Vector = bite of the Ixodes tick
• Borrelia recurrentis - Relapsing fever Vector =bite of the human body louse Blood smear observe spirochete

Spirochetes• Treponema pallidum
– Agent of Syphilis– RPR and VDRL for antibody detection– Molecular methods
• Brachyspira – intestinal spirochete found on the brush border of the intestine, ?? Role in disease
• Leptospira interrogans – Leptospirosis– Fever with rash and renal involvement– Urine from rats and other animals contaminate water supplies
Darkfield from chancre lesion
Spirochete – Shepherd’s crook

Unusual Bacterial diseases
• Granuloma inguinale– Klebsiella (Calymmatobacterium) granulomatis– Rare STD – causes ulcerative genital lesions
• Streptobacillus moniliformis – Rat bite fever or Haverhill fever– L form or cell wall deficient bacteria– Inhibited by SPS in blood culture media– Needs serum supplementation to grow, will not grow in a
bacteriology culture– Infection obtained from a rat bite

Anaerobes• Anaerobic infections can occur in virtually
every organ and region of the body• Polymicrobial – both aerobic and anaerobic species in the
infections• Endogenous organisms (commensal flora) cause most
anaerobic infections– Due to Trauma, vascular or tissue necrosis cutting off the oxygen
supply to the involved tissue• Surgery plus antibiotics often necessary• Anaerobic culture collection – must be oxygen free
– Gel contaning swabs – Eswab, – Evacuated vials (port o cult)/ oxygen free collection– Do not refrigerate specimens – absorb oxygen and kill anaerobes

Anaerobes• PRAS media – pre reduced anaerobically sterile
– Media packaged in oxygen free environment• Most common media used
– CDC anaerobic blood agar– Kanamycin-vancomycin blood agar– Bile Esculin agar– Thioglycollate broth– Chopped meat glucose broth
• Anaerobic gas pack jars – incubate cultures in anaerobic conditions• Wet pack – add 10 ml water to hydrogen and CO2 generating
envelope/ requires palladium coated catalysts – generate heat• Dry pack – (Anaeropack) Absorbs O2 and generates CO2
• Anaerobic bacteria can be poorly staining and bizarre or irregularly shaped

Anaerobic Gram Negative Rods

Gram negative Anaerobic Bacillus• Bacteroides fragilis group –
– Pleomorphic gram negative rod– Growth in the presence of bile– Esculin positive – turning media black– Resistant to Penicillin and Kanamycin– Most common organisms in human bowel – B. fragilis– B. ovatus– B. thetaiotamicron – indole positive– B. uniformis – B. vulgatus
• Resistant to Penicillin by beta lactamase enzyme – • Metronidazole is antibiotic of choice
Growth on bileBlack pigment

Gram Negative Anaerobic Bacillus
• Prevotella and Porphyromonas species– Will not grow in the presence of bile– Will not turn black on esculin media– Brick red fluorescence or black pigment– Normal commensal flora of the upper respiratory tract– Cause respiratory tract infection

FusobacteriumFusiform gram negative bacilli – spindle shaped with pointed ends • Normal flora in upper respiratory tract• Associated with mouth and respiratory tract abscess
formation and liver abscess • Vincent’s angina – necrotizing oral infection caused
by Fusobacterium species plus spirochetes• Lemierre’s syndrome - oropharyngeal infection that
leads to thrombosis in jugular vein, septicemia, high fatality rate, caused by Fusobacterium necrophorum

Anaerobic Gram Positive Rods

Clostridium species
• Gram positive bacilli (boxcar shaped ) with spores– Some rods may over-decolorize and appear red
• Clostridium perfringens – most common species– Predominate anaerobic G+R in intestine – Double zone of beta hemolysis on BAP– Lecithinase produced on egg yolk agar– reverse camp test +
Lecithinase
Reverse Camp Test

Clostridium• Clostridium botulinum –
– Adult disease – Preformed heat labile toxin ingested in mass produced or home-canned foods
– Infant disease - spore ingested from nature, neurotoxin produced in gut, • Begins with constipation and difficult sucking bottle • Honey, soil, household dust
– Life threatening neuroparalytic disease• Clostridium tetani
– Disease = Tetanus– On Gram stain the cells appear like Tennis racket – Toxin enters due to penetrating skin injury– Disease in Non immunized– Spastic contractions of voluntary muscles, hyperreflexia, lock jaw
(trismus)

Clostridium • C. septicum –
– Bacteremia or Gas Gangrene in patient with underlying malignancy– Normal flora in the GI tract
• C. difficile – – Disease = Antibiotic associated colitis– Transmission can also occur in the hospital environment due to the viability of the spores– Diagnosis of infection:
EIA methods are not sensitive and are discouraged
PCR methods are more sensitive and specific for disease detection
– Two toxins produced: Toxin A – enterotoxin causing fluid
accumulation
Toxin B – potent cell cytotoxin – detected in PCR assays*

Actinomyces• Branching gram positive bacilli - do not form spores • Normal flora in the mouth• Capable of forming sulfur granules in tissue – often found on normal tonsil• Actinomyces israelii – associated with oral, thoracic, and abdominal infections, IUD infections
Bread crumb colonies in broth
Molar tooth colony on agar plates
Penicillin susceptible.

Branching Gram positive rods of Actinomyces – antler like
Molar tooth colony
Sulfur granule

Propionibacterium acnes
• Pleomorphic gram positive rod• Catalase positive• Spot indole positive• Normal flora skin, oral, GU and GI• Potential contaminate in blood cultures• Can be pathogen in cerebral shunt infections • Firmly established as significant cause of prosthetic joint
infection – particularly shoulder joints• Cultures should be held 7- 14 days to detect• Therapy - Ampicillin

Bacterial vaginosis
• Clue cells are diagnostic• Mixed anaerobic/aerobic bacterial infection are the two most
common organisms in vaginosis:– Gardnerella vaginalis (aerobic gram variable rod) and Mobiluncus
(anaerobic curved gram negative rod)– Human blood agar for the culture of Gardnerella, it
is beta hemolytic and distinctive
• Nugent score Gram (for BV diagnosis)– Healthy = Lactobacillus Gram positive rods– Intermediate = mixed bacterial types– BV = Gardnerella and Mobiluncus on smear