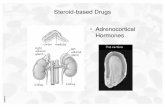
Adrenocortical hormones. Classification of Adrenocortical Hormones 1.Glucocorticoids...
-
Upload
conrad-chambers -
Category
Documents
-
view
240 -
download
2
Transcript of Adrenocortical hormones. Classification of Adrenocortical Hormones 1.Glucocorticoids...

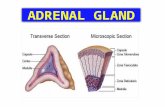
Adrenocortical hormones

Classification of Adrenocortical Hormones
1. Glucocorticoids2. Mineralocorticoids3. Sex hormones

1. Glucocorticoid
1. Short acting: hydrocortisone, Prednisone (8-12 hours)
2. Intermediate-acting: triamcinolone (12-36 hours)3. Long acting: dexamethasone (48 hours)

Pharmacokinetics:• Well absorbed after oral administration.• 75% of corticosteroids are bound to plasma globulins
(CBG). CBG is increased by estrogen and decreased in liver cirrhosis.
• Metabolism is by the liver and excretion is by the kidney.
Mechanism of action:• Corticosteroids transported to the nucleus, where it
interacts with many DNA receptors (genes) and affect their function.

Pharmacological effects:1. On metabolism:
A. Carbohydrate metabolism: hyperglycemia (↓ peripheral glucose utilization).
B. Protein metabolism: Catabolic effect → ↓ muscle mass and thin limbs.
C. Fat metabolism: ↑ lipolysis with redistribution of fat.
2. Na+ & water retention and hypokalemia.

3. Anti-inflammatory and anti-immunological effects:– Inhibit antigen-antibody reaction.– Inhibit lymphocyte and macrophage activity and
function.– Stabilize lysosomal membrane.– ↓ release of inflammatory mediators and cytokine
production by inflammatory cells.– Inhibit phospholipase A2 enzyme so reduce
synthesis of PGs & LTs. – ↓ capillary permeability.

4. CVS: Hypertension due to Na+ & water retention.5. Hematological effects:
1. ↑ RBCs and ↓ lymphocytes and eosinophils.2. ↑ coagulation factors and blood cholesterol.
6. On growth:1. Growth retardation, which is not prevented by
growth hormone.7. On bone:
1. ↓ bone matrix and ↑ Ca2+ excretion (osteoporosis).
8. Inhibit hypothalamo-pituitary-adrenal axis.

Doses:• Short-term therapy: duration of
therapy is < 2 weeks.• Long term therapy: duration of
therapy is > 3 weeks.• Alternate day therapy: double
the dose and give it every other day.

Therapeutic uses:1. As replacement therapy in adrenocortical insufficiency:
A. Acute adrencortical insufficiency (acute addisonian crisis
B. Chronic adrenocortical insufficiency (Addison’s disease).
2. Adrenocortical hyperplasia due to elevated ACTH:A. Congenital adrenal hyperplasia:B. Cushing syndrome: due to pituitary adenoma, adrenal
tumors.

3. Stimulation of lung maturation in the fetus
4. Anti-inflammatory: e.g. vasculitis, rheumatic fever, arthritis, bronchial asthma, etc.
5. Allergic diseases: e.g. anaphylactic shock, urticaria and bronchial asthma.
6. Autoimmune disease: e.g. SLE 13. Shock and hypotension14. Organ transplantation: as immunosuppressive to
prevent graft rejection.15. Cerebral edema: dexamethasone is used after brain
surgery to minimize edema.16. Acute hypercalcemia: to enhance Ca2+ excretion.

Side effects:1. Acute adrenal insufficiency (acute addisonian crisis):– It occurs after sudden withdrawal of corticosteroids
after prolonged administration.– Prevention: Gradual withdrawal of corticosteroids.
2. Iatrogenic Cushing syndrome: – Occurs if high doses used or it is used for > 2 -3
weeks. It is characterized by moon face, buffalo hump, weak muscles, osteoporosis, hypertension, DM, edema, etc.


3. Immune suppression leading to:– Flaring of infections (especially viral and TB). – Decrease wound healing
4. Peptic ulcer– Due to prolonged PGs suppression.
5. Rise of IOP (Glaucoma).6. Hyperglycemia.7. Hypercoagulability leading to thromboembolism8. Osteoporosis.9. Retardation of growth in children.10. Pregnancy: congenital cleft palate.

6. Local side effects:• Skin atrophy & hypopigmentation on prolonged
use.• Repeated administration in joints may produce
joint destruction & infection

Contraindications:
1. Presence of infections: especially viral infection and TB:
because corticosteroids can inhibit immune functions.
N.B. Uses of corticosteroids in presence of T.B:
• TB meningitis: to prevent adhesions.
• TB of the suprarenal gland: to correct hypofunction.
• Miliary TB: to ↓ TB toxemia.

2. Peptic ulcer: they ↓ synthesis of PGE2 and I2 that protect
the stomach.3. Hypertension & heart failure: they cause salt and water
retention.4. DM (except fluorinated corticosteroids e.g.
dexamethasone and betamethasone because they have anti-inflammatory with less hyperglycemic effects).
5. Mental disorders e.g. psychosis or depression.6. In early pregnancy: may cause cleft palate.

Drug interactions:1. With NSAIDs: ↑ incidence of peptic ulcer and
decreases its healing2. With insulin: It has anti-insulin effect
(hyperglycemia)3. With anticoagulant drugs: it decreases their effect.4. With loop diuretics: it aggravate hypokalemia.

Mineralocorticoids1. Natural mineralocorticoids: • Aldosterone• It binds to specific intracellular receptors in the distal
convoluting tubules to inhibit Na+ excretion and stimulates K+ and H+ excretion.
2. Synthetic mineralocorticoidsA. Deoxycorticosterone acetate(DOCA)• It has mainly mineralocorticoid effect.B. Fludrocortisone• It has both glucocorticoid and mineralocorticoid
effect.

Adverse effects
• Hypernatremia• Hypervolemia• Hypokalemic alkalosis (weakness, paralytic ileus and
tetany)• Hypertension
Therapeutic uses
• Acute adrenal insufficiency• Chronic adrenal insufficiency (Addison's disease)

Hyperaldosteronism
• Treatment of hyperaldosteronism:1. Primary hyperaldosteronism: by surgical removal
of tumor.2. Secondary hyperaldosteronism: Aldosterone
antagonists: spironolactone.

Adrenocortical hormone antagonistsA. Glucocorticoid inhibitors:
1. Aminoglutethimide:• Inhibit steroid hormone synthesis .• Used in adrenocortical malignancies and cancer
breast. In postmenopausal or Ovariectomized women with metastatic breast cancer (to eliminate adrenal estrogen production
2. Metyrapone:• It inhibits enzyme necessary for synthesis of
glucocorticoids. • Used to measure the capacity of the anterior
pituitary to secrete ACTH.

3. Ketoconazole:• It is antifungal drug with slight inhibition of
mineralocorticoids synthesis.• Used in Cushing’s syndrome
4. Mifepristone • Blockade cytoplasmic glucocorticoid receptor• Inoperable patients with ectopic ACTH
secretions or adrenal carcinoma (it is also an antiprogestin)

B. Aldosterone receptors inhibitors:Spironolacone • Blockade of cytoplasmic mineralocorticoid
receptor• (used in hyperaldosteronism)

Good luck