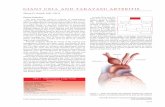
A case of temporal arteritis
Click here to load reader
-
Upload
anahita-sharma -
Category
Health & Medicine
-
view
156 -
download
0
Transcript of A case of temporal arteritis

A Case of Temporal Arteritis
KEY LEARNING POINTSFROM A MEDICAL HISTORY OBTAINED BY FOUR THIRD-YEAR MEDICAL
STUDENTS FROM A PATIENT WITH NEUROLOGICAL SIGNS

THE CASE. 80 YEAR OLD WOMANo 2 years ago: began to experience severe episodes of persistent headaches not relieved by over-the-counter and
prescribed analgesics, that occurred recurrently and for several hours at a time
Headaches were described as a crushing pain that radiated from her neck, over her head, and into her face
Associated with loss of appetite, jaw pain, and photosensitivity
No other abnormal neurological signs were present, no true visual loss, and no identifiable triggers
An in-hospital diagnosis of temporal arteritis was made on an especially acute episode of the headache, and steroidal treatment immediately commenced
On a daily dosage of prednisolone (3.5 mg); self-administration is increased on episodic flares Low-dosage aspirin, omeprazole, a supplementary medication for her joints, as adjuncts in her steroidal treatment
Levothyroxine prescribed for hypothyroidism prior to diagnosis of temporal arteritis
Has otherwise been of normal health and fitness over the course of her life Nothing of note on systematic enquiry
Previous hospitalisation has been for childbirthNo apparently significant family history
Personally believes her headaches may have been triggered by stressful, financially-related, life events; her relationship with her husband is a positive one and he was highlighted as a significant source of psychosocial support
LEARNING
POINT 1
LEARNING POINT 2
LEARNING POINT 3

WEAKNESSES IN THE HISTORY Information that would have been useful to obtain in retrospect:
▪ What were the precise time distributions of her headaches, in terms of their onset and how long they lasted? This could have been undertaken in more detail, and is essential to a differential diagnosis.
▪ What were the precise dosages of the NSAIDs prescribed? This is of particular significance on revelation of the patient’s diagnosis. Temporal arteritis is an inflammatory condition, and given the anti-inflammatory mechanism of NSAIDs, pain relief should have been obtained. However, an inadequate dosage in light of the severity of the diagnosis may explain why this was not the case.
▪ Given her appetite loss, did she experience any degree of weight loss over the course of her headaches? This might suggest involvement of the Temporalis. If mastication becomes associated with pain, one might naturally expect lower food intake over time.

What it looks like
Left: Normal Aorta
Right: Giant-Cell Arteritis

LEARNING POINT 1. It’s
A CHALLENGING DIAGNOSIS• May be complicated by features of other neurological conditions
• Headaches are a common presentation in a geriatric population, with tension-type headaches being the most frequently occurring – there are multiple overlapping features
• Irreversible vision loss is a consequence, and therefore, treatment must be immediately commenced on clinical suspicion
CLINICAL DIAGNOSIS: internal and external carotid artery involvement
Jaw claudication
Headache; temporal
pain
Scalp tenderness
Acute onset of visual
disturbance
Abnormal temporal artery
on gross examination

ACUTE PHASE REACTANT MARKERS
✓ Elevated ESR: erythrocyte sedimentation rate – high specificity
✓ Elevated CRP – also a marker of ‘disease activity’
TEMPORAL ARTERY BIOPSY
◆ Classification by vessel wall involvement e.g. small periadventitial, up to transmural
◆ Identification of no. of white blood cells
◆ Presence of thromboses and necroses
◆ A wide histiologic spectrum of inflammatory lesions in temporal artery biopsy VASCULAR IMAGING
Delineation of vascular anatomy features such as luminal narrowing, occlusion, and calcification
MULTIDISCIPLINARY INVOLVEMENT Rheumatologists play a role So does the ophthalmologist, as ocular symptoms are crucial and common clinical manifestations