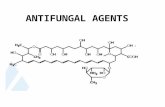
6.Antifungal Agents
-
Upload
mulatumelese -
Category
Documents
-
view
231 -
download
0
Transcript of 6.Antifungal Agents
-
7/27/2019 6.Antifungal Agents
1/51
8/20/2013 1
Antifungal Agents
-
7/27/2019 6.Antifungal Agents
2/51
8/20/2013 2
Fungal infections are termed mycoses
Can be divided into:
Superficial mycoses
Affect the skin, hair and nailsSubcutaneous mycoses (topical)
Affect the muscle and connective tissue below the skin
Systemic (invasive) mycoses
Involve the internal organsAllergic mycoses
Affect lungs or sinuses
Patients may have chronic asthma, cystic fibrosis or sinusitis
-
7/27/2019 6.Antifungal Agents
3/51
8/20/2013 3
Introduction
Fungal infections are usually more difficult to treat than
bacterial infections, because.
Fungal organisms grow slowly and,
Fungal infections often occur in tissues that are poorly
penetrated by antimicrobial agents.
-
7/27/2019 6.Antifungal Agents
4/51
8/20/2013 4
-
7/27/2019 6.Antifungal Agents
5/51
8/20/2013 5
Systemic Antifungal Drugs
Amphotericin B
Amphotericin B is a polyene antifungal drug produced by
the actinomycete Streptomycin nodosus
Consists of a large ring structure with both hydrophilic
and lipophilic regions (Amphoteric ).
-
7/27/2019 6.Antifungal Agents
6/51
8/20/2013 6
Mechanism of Action
Amphotericin B and other polyene macrolide antibiotics bind tothe fungal cell membrane sterol moiety, primarily ergostero l
Form pores or channels that increase the permeability of the
membrane Leakage of a variety of small molecules. Its Amphipathic characteristic facilitates pore formation.
It avidly with lipids (ergosterol) along the double bond-richside
Associates with water molecules along the hydroxyl-rich side
The lipophilic portions surround the outside of the poreand the hydrophilic regions line the inside.
-
7/27/2019 6.Antifungal Agents
7/51
8/20/2013 7
Amphotericin has a lesser affinity for the mammalian cell
membrane component cholesterol , but this interaction does
account for most adverse toxic effects associated with this drug.
The predominant sterol of bacteria, like in human cells, ischolesterol hence amphotericin B is selective in its fungicidal
effect.
Poorly absorbed from GIT.
Oral amphotericn B effective only on fungi with in the GIT
tract and not be used for treatment of systemic infection .
-
7/27/2019 6.Antifungal Agents
8/51
8/20/2013 8
The IM administration is painful
Is given iv in the treatment of systemic infections
The original preparation of amphotericin B for intravenous use is
a deoxycholate dispersion in dextrose.
This micellar suspension is associated with serious toxic side
effects, in particular renal damage
the toxic side effects were partially ameliorated when a lipid
carrier was used.
-
7/27/2019 6.Antifungal Agents
9/51
8/20/2013 9
Three lipid-associated formulations have been used:
1) Liposomal : drug is encapsulated in phospholipid-containing
liposomes2) Colloidal dispersion: drug is packaged into small lipid disks
containing cholesterol sulphate
3) Lipid complex: drug is complexed with phospholipids to produce
ribbon-like structures
-
7/27/2019 6.Antifungal Agents
10/51
-
7/27/2019 6.Antifungal Agents
11/51
8/20/2013 11
Antifungal Activity
Has the broadest spectrum of antifungal and is fungicidal actionincluding;-
Sporotrichum schenkii and
Cryptococcus neoforman,Histoplasma capsulatum,
Blastomycosis
Coccidioides immitis, Aspergillus fumigatus.
Candida albicans respond to higher concentrations
-
7/27/2019 6.Antifungal Agents
12/51
8/20/2013 12
Therapeutic use
The use of amphotericin B has diminished due to reduced
toxicity profile and ease of administration of newer drugs, the
azoles
But amphotericin B remains the drug of choice for initiation of treatment in nearly all life-threatening mycotic infections.
Once a clinical response has been elicited maintenance
therapy is continued with an azole.
-
7/27/2019 6.Antifungal Agents
13/51
8/20/2013 13
For the AIDS patient with moderate to severe cryptococcal
meningitis,
Amphotericin B appears to be superior to fluconazole for
initial treatment;Once infection is controlled, fluconazole in a daily oral dose
is superior to and more convenient than weekly intravenous
amphotericin B in the prevention of clinical relapses.
For the AIDS patient with disseminated histoplasmosis,
But once infection is controlled, daily oral itraconazole is
preferred
-
7/27/2019 6.Antifungal Agents
14/51
8/20/201314
Amphotericin B remains the drug of choice in the treatment of
invasive aspergillosis.
An opportunistic infection by a fungus of the genus
Aspergillus;Characterized by inflammation and lesions of the ear and
respiratory organs
The patient should be hospitalized For systemic infectionsIts toxicity could be reduced by using smaller doses of the drug
in combination with other systemic antifungal agents
-
7/27/2019 6.Antifungal Agents
15/51
8/20/201315
Adverse Effects
Infusion-Related Adverse Effects
IV infusion may cause phlebitis, fever, chills, muscle
spasms, vomiting, headache, and hypotension.
Possibly mediated by interlukines or prostaglandins.
Test dose of 1mg infused over 30-60 minutes is given to
reduce the risk of serious events anaphylaxis
Premedication with antipyretics, antihistamines, meperidine,or corticosteroids can be helpful.
-
7/27/2019 6.Antifungal Agents
16/51
8/20/2013 16
Nephrotoxicity is the most common and the most serious long-
term toxicity of amphotericin B.
It reduces glomerular and renal tubular blood flow through
a vasoconstrictive effect on afferent renal arterioles,
Which can lead to destruction of renal tubular cells and
disruption of the tubular basement membrane.
-
7/27/2019 6.Antifungal Agents
17/51
8/20/2013 17
Renal tubular acidosis and renal wasting of K+ and Mg2+ also
may be seen during and for several weeks after therapy.
May necessitates replacement of the minerals.
Nephrotoxicity is increased by concurrent therapy with other
nephrotoxic agents, such as aminoglycosides or cyclosporine .
-
7/27/2019 6.Antifungal Agents
18/51
8/20/2013 18
Keeping patients well hydrated may reduce nephrotoxicity;
Saline infusions prior to amphotericin B dosing have been
advocated, and
Concomitant diuretic therapy should be avoided.
Prolonging the infusion rate may decrease toxicity infuse
over 4-6 hrs for first dose and if tolerated reduce infusion to
over 2 hrs.
-
7/27/2019 6.Antifungal Agents
19/51
-
7/27/2019 6.Antifungal Agents
20/51
8/20/2013 20
There may be an increased risk of digitalis toxicity if digoxin is
administered concurrently with amphotericin B.
Administration with nephrotoxic drugs (eg, aminoglycosides orcyclosporine) may increase the risk of nephrotoxicity in patients
Amphotericin B decreases the effects of miconazole.
-
7/27/2019 6.Antifungal Agents
21/51
8/20/2013 21
Flucytosine
Flucytosine ( 5-fluorocytosine) is a fluorinated pyrimidinerelated to fluorouracil.
Mechanism of Action and Resistance
Flucytosine is taken up by fungal cells via the enzymecytosine permease and 5-FC is converted to 5-fluorouracil
inside the cell by the fungal enzyme cytosine deaminase
Fluorouracil is metabolized first to 5-fluorouracil-ribose
monophosphate (5-FUMP) by the enzyme uracil
phosphoribosyl transferase.
-
7/27/2019 6.Antifungal Agents
22/51
8/20/2013 22
5-FUMP is then;-
Either incorporated into RNA in place of uracil (may inhibit
protein synthesis) or
Metabolized to 5-fluoro-2'-deoxyuridine-5'-monophosphate
(5-FdUMP),
A potent inhibitor of thymidylate synthetase (interfere
with fungal DNA synthesis ).
-
7/27/2019 6.Antifungal Agents
23/51
8/20/2013 23
-
7/27/2019 6.Antifungal Agents
24/51
8/20/2013 24
The selective action of flucytosine is due to ;-
The lack or low levels of cytosine deaminase in mammalian
cells.
Mechanism of resistance can be;-
Loss of the permease,
Decreased activity of the enzyme uracil phosphoribosyl
transferase or cytosine deaminase
-
7/27/2019 6.Antifungal Agents
25/51
8/20/2013 25
Antifungal Activity and Clinical Uses
Spectrum of activity is restricted to Cryptococcus neoformans
and some candida species
The Clinical use at present is confined to combination therapy,
either with amphotericin B for cryptococcal. meningitis or withitraconazole for chromoblastomycosis (A fungal infection
characterized by itchy warty nodules on the skin).
When it is used as monotherapy, resistance and clinical failure
are common.
-
7/27/2019 6.Antifungal Agents
26/51
8/20/2013 26
Adverse Effects
Fluorouracil is responsible for the ADRs of flucytosine.
Bone marrow toxicity with anemia, leukopenia, and
thrombocytopenia are the most common adverse effects.
Other ADRs such as skin rash, epigastric distress, diarrhea,
and liver enzyme elevations can occur.
-
7/27/2019 6.Antifungal Agents
27/51
8/20/2013 27
The Azoles
Are broad spectrum antifungal
Concentration-independent fungistatic agents
Drugs includeTriazoles :-
Clotrimazole, Miconazole, Ketoconazole, Econazole,
Butoconazole, Oxiconazole, Sertaconazole, and SulconazoleImidazoles:-
Fluconazole, Itraconazole, Voriconazole, and Terconazole
-
7/27/2019 6.Antifungal Agents
28/51
8/20/2013 28
Mechanism of Action
All azoles exert antifungal activity by binding to cytochrome
P450 enzyme (14-a-sterol demethylase)
W/h is responsible for the demethylation of lanosterol to
ergosterol.
Impair the biosynthesis of ergosterol for the cytoplasmic
membrane.
Result in damaged, leaky cell membranes.
-
7/27/2019 6.Antifungal Agents
29/51
8/20/2013 29
Resistance
The primary mechanism of resistance in C. albicans is
accumulation of mutations in ERG11 , the gene coding for the
14-a-sterol demethylase.
Increased production of 14-a-sterol demethylase and
Increased azole efflux are other potential cause
Cross resistance is conferred to all azoles.
-
7/27/2019 6.Antifungal Agents
30/51
Mechanisms of antifungal resistance
Target enzyme modificationErgosterol biosyntheticpathwayEfflux pumpsDrug import
8/20/2013 30
-
7/27/2019 6.Antifungal Agents
31/51
8/20/2013 31
Fluconazole
Fluconazole is very effective and commonly used in the treatment
of infections with most Candida spp.
AIDS patients with esophageal candidiasis usually respond
to fluconazole.Thrush in the end-stage AIDS patient, often refractory to
Nystatin, Clotrimazole, and ketoconazole, can usually be
suppressed with oral fluconazole.
-
7/27/2019 6.Antifungal Agents
32/51
8/20/2013 32
Fluconazole is the azole of choice in the treatment and
secondary prophylaxis of cryptococcal meningitis.
It is a good alternative to amphotericin B in the initial
treatment of mild cryptococcal meningitis and superior to
amphotericin B in the long-term prevention of relapsing
meningitis.
-
7/27/2019 6.Antifungal Agents
33/51
-
7/27/2019 6.Antifungal Agents
34/51
8/20/2013 34
Adverse Effects
Fluconazole is well tolerated.
Nausea, vomiting, abdominal pain, diarrhea, and skin rash
have been reported in few patients.
Asymptomatic liver enzyme elevation have been reported.
Alopecia has been reported as a common adverse event in
patients receiving prolonged high-dose therapy.
-
7/27/2019 6.Antifungal Agents
35/51
8/20/2013 35
Drugs interaction
Fluconazole is an inhibitor of CYP3A4 and CYP2C9.
Significantly increases plasma concentrations of cisapride,
cyclosporine, phenytoin, sulfonylureas ( glipizide,
tolbutamide, others), tacrolimus, theophylline,
telithromycin, and warfarin.
-
7/27/2019 6.Antifungal Agents
36/51
Biopharmaceutical Characteristics of the Triazole Antifungals
Fluconazole Itraconazole
Voriconazole
Spectrum vs.Candida andAspergillus
C. albicans, C.tropicalis +/- C. glabrata No Aspergillus
Similar Candida coverage as fluconazole,+ Aspergillus
Broad, includes mostCandida spp.,
Aspergillus,Fusarium sp. Not Zygomycoses
Oral formulation(% bioavailibility) Tablet (>90%) Capsule (6-25%)Solution (20-60%) Tablet (>90%)
Intravenousformulation
Available, nosolubilizer
Available, cyclodextrin Available,cyclodextrin
Clearance Renal (80%) Hepatic 3A4 Hepatic 2C19, 3A4
Serum half life (hr) 24 24-30 6-24
CSF penetration Excellent Poor ExcellentCYP 3A4 inhibition Weak Strong Moderate-Strong
Adverse effects N&V, hepatic N&V, diarrhea(solution), hepatic, CHF
N&V, visualdisturbances,
hepatic, rash8/20/2013 36
-
7/27/2019 6.Antifungal Agents
37/51
8/20/2013 37
Ketoconazole
Systemic use of ketoconazole has diminished;
It has been replaced by itraconazole for the treatment of all
mycoses except when the lower cost of ketoconazoleoutweighs the advantage of itraconazole.
But it remains useful in the treatment of cutaneous and
mucous membrane dermatophyte and yeast infections.
-
7/27/2019 6.Antifungal Agents
38/51
8/20/2013 38
Ketoconazole has activity against some Gram-positive bacteria
and some antiprotozoal activity against Leishmania spp.
Itraconazole lacks ketoconazole's corticosteroid suppression,
while retaining most of ketoconazole's pharmacological
properties and expanding the antifungal spectrum.
IN large doses, Ketoconazole inhibit several biosynthetic
steps in the synthesis of adrenal and gonadal steroids.
Thus reduce the plasma conc. Of cortisol and testosterone
-
7/27/2019 6.Antifungal Agents
39/51
8/20/2013 39
Several factors affect the time taken for peak serum
concentrations (2-4hrs) :
1) disintegration/dissolution rate (favoured by acidic pH?)
2) Gastric emptying rate3) Intestinal metabolism (CYP 3A4 in intestinal wall)
4) Rate of absorption from the intestine
5) First Pass effect (metabolism in liver)
6) Clearance rate.
Food delays absorption, but does not decrease peak serum
concentrations significantly.
-
7/27/2019 6.Antifungal Agents
40/51
8/20/2013 40
-
7/27/2019 6.Antifungal Agents
41/51
Ketoconazole - Drug Interactions
Potent inhibitor of cytochrome P450 3A4
Rifampin and phenytoin decrease ketoconazole levels
Ketoconazole increases cyclosporin, warfarin, astemizole,
corticosteroid, and theophylline levelsMany of these drug interactions are severe
Drugs that increase gastric pH will decrease blood levels of
ketoconazole Antacids, omeprazole, H2 blockers
8/20/2013 41
-
7/27/2019 6.Antifungal Agents
42/51
Ketoconazole - Adverse effects
Adverse effects
N&V, worse with higher doses (800 mg/day)
Hepatoxicity (2-8%), increase in transaminases, hepatitis
Dose related inhibition of CYP P450 responsible fortestosterone synthesis
Gynecomastia, oligosperma, decreased libido
Dose-related inhibition of CYP P450 responsible for adrenalcortisol synthesis
8/20/2013 42
-
7/27/2019 6.Antifungal Agents
43/51
8/20/2013 43
Griseofulvin
Griseofulvin is fungistatic in vitro for various species of the
dermatophytes.
It is not effective against candida albicans.
Is mild cytotoxic and damage the microtubular protien, thus
inhibits fungal mitosis.
Acts mainly on the growing fungal cells
Exhibit greater affinity for the diseased than the normal skin
-
7/27/2019 6.Antifungal Agents
44/51
8/20/2013 44
It is not effective topically is administered orally
But has poor gastrointestinal absorption .
Can be improved by microcrystalline processing of the drugand by taking the drug with fatty meals
The drug binds to keratin precursor cells and newly
synthesized keratin in the stratum corneum of the skin, hair,
and nails, stopping the progression of dermatophyte infection
.
-
7/27/2019 6.Antifungal Agents
45/51
8/20/2013 45
Indications
Tinea capitis; clinical cure occurs within 4-6wks of therapy
Tinea pedis, Tinea cruris, Tinea barbae the treatment is
continued for 4-8wks
Onychomycosis: treatment for fingernail infection takes 4-
6months while infection of the toenail is treated for 6-12
months. Since chronic fungal infections tend to causehyperkeratosis, concomitant topical keratolytic therapy with
salicylic acid is beneficial
-
7/27/2019 6.Antifungal Agents
46/51
8/20/2013 46
Adverse effect
Headache, skin rashes and urticaria, dry mouth, an altered
sensation of taste, and gastrointestinal disturbances .
There have been a few reports of hepatotoxicity
Drug interaction
Griseofulvin increases warfarin metabolism, and
Griseofulvin metabolism is increased by phenobarbital.
Griseofulvin has been largely replaced by newer antifungalmedications such as itraconazole and terbinafine.
-
7/27/2019 6.Antifungal Agents
47/51
8/20/2013 47
Topical Antifungal
Nystatin
Nystatin is a polyene macrolide much like amphotericin B.
It has similar mechanism of action with amphotericin B.
Nystatin is active against most candida species.
Is most commonly used for suppression of local candidal
infections.
Some common indications include oropharyngeal thrush,vaginal candidiasis
Nail involvement due to candida does not respond to it
-
7/27/2019 6.Antifungal Agents
48/51
8/20/2013 48
It is too toxic for parenteral administration and is only used
topically.
Produce nephrotoxicity
It is not absorbed to a significant degree from skin, mucous
membranes, or the gastrointestinal tract.
oral administration may cause N,V,AND D
-
7/27/2019 6.Antifungal Agents
49/51
8/20/2013 49
Topical Azoles
Often used in vulvovaginal candidiasis and oral thrush.
Several other azoles are available for topical use.
Clotrimazole
Fungicidal concentrations remain in the vagina for as long as 3days after application of the drug.
Clotrimazole is available as a 1% cream, lotion, and solution
1% or 2% vaginal cream or vaginal tablets of 100, 200, or 500mg.
On the skin, applications are made twice a day
-
7/27/2019 6.Antifungal Agents
50/51
8/20/2013 50
For the vagina, the standard regimens are one 100-mg tablet
once a day at bedtime for 7 days, one 200-mg tablet daily for 3
days, one 500-mg tablet inserted only once, or 5 g of cream
once a day for 3 days (2% cream) or 7 days (1% cream).
Clotrimazole has been reported to cure dermatophyte
infections, cutaneous candidiasis, vulvovaginal candidiasis,
Recurrences are common after all regimens .
-
7/27/2019 6.Antifungal Agents
51/51
8/20/2013 51
Other topical azoles include
miconazole, ketoconazole, tolnaftate, terbinafine