224 Jones H - cmcgc.com · 9/24/2010 2 Micro 101 • Gram’s stain – Offer earliest information...
Transcript of 224 Jones H - cmcgc.com · 9/24/2010 2 Micro 101 • Gram’s stain – Offer earliest information...

9/24/2010
1
General Approach to Antimicrobial Use
in the Outpatient Wound Care Setting
Clinical Symposium on Advances in Skin & Wound Care
October 2, 2010
Harriet Jones, MD, BSN; FAPWCA
Disclosures
• Speakers Bureau
– Cubist Pharmaceuticals
• Editorial BoardEditorial Board
– Today’s Wound Clinic
• Graphic Pictures to Follow
Objectives for Participants
• Increased understanding of a bug’s life*– Laboratory identification of microorganisms encountered in the
outpatient wound care setting– Continuum of organisms in wounds: colonization infection
• Non‐exhaustive review antimicrobial agents– Topical
S i f bl f i i i– Systemic agents favorable for use in outpatient setting• Oral• Intravenous • Personal pearls & pitfalls (PPP)
• Increased appreciation for MRSA as a pathogen• Recognition that options in antimicrobial arsenal are limited– Must prescribe antimicrobial agents wisely
* Credit: Disney Films

9/24/2010
2
Micro 101
• Gram’s stain – Offer earliest information for provider– Differentiates Gram Positive Cocci (GPC’s) from
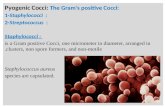
Gram Negative Rods (GNR)• Gram Positive Cocci (GPC)
– Staph sppStaph spp– Strep spp
• @ 24h if + growth on streaked plate – Coagulase test – chemical reagent– Coagulase positive = unique to Staph aureus– Coagulase negative = any other Staph spp
• Do NOT yet know if MRSA– Must assume MRSA
Process for Gram Staining
arrowscientific.com.au
Gram’s Stain showing GPC and GNC
library.med.utah.edu

9/24/2010
3
Blood Agar Plate
http://www.lexic.us/definition‐of/blood_agar
The Microbial Continuum in Wounds
• Contamination
• Colonization
• Critical Colonization
• Infection
Contamination
• Presence of non‐replicating microorganisms on the wound surface
• Occurs 100% at time of wounding
• Absence of host clinical response
• Sources:
– Skin, periwound
– Linen, devices
– Urine, stool

9/24/2010
4
Colonization
• Occurs shortly after contamination• Replicatingmicroorganisms
– superficially attached to wound surface
• Not necessarily harmful– No need for topical or systemic antibiotics– Risks development of drug resistant bacteria
• Absence of host response• Variety of organisms
– Coagulase negative staph spp (Staph epi’s)– Pseudomonas– Non beta‐hemolytic Streptococci spp
Critical Colonization
• Bacterial bio‐burden sufficient to cause arrested healing – Perpetual inflammatory phase
• Topical antimicrobials are indicated
• Organisms have not yet invaded deeper soft tissue – no activation of hosts immune cells
• Granulation tissue may appear unhealthy
• Colonizer ≠ pathogen
Infection• Determination by culture
– When ‐ not if ‐ to culture a chronic wound • After infection clinically diagnosed
• By definition = 105 cfu/gram tissue– 102 : beta hemolytic strep– Any Mycobacterial spp; Anthracis spp; Yersinia pestis
• Presentation depends on – Hosts ability to mount response– Type of organism(s)– Chronicity of wound
• dose x virulencehost resistance
• Treatment = patient tailored
Acute and Chronic Wounds; Bryant & Nix; 3rd edition; Dow; OWM vol 49 5A supplement

9/24/2010
5
Graphic Example of Microbiologic Continuumon ONE Wound
Antimicrobial Agents
• Topical Antibiotics & Antiseptics
– Dressings
/ /– Creams/ Gels/Ointments
• Systemic
– Oral
– Intravenous
Topical AgentsNothing ‘new’ under the sun….
• ~ 2500 years ago
– Chinese ‐moldly soybean curd for carbuncles boilscarbuncles, boils
– Greeks ‐ wine, myrrh, inorganic salts for wounds
PPID; 6th edition ch.16; p242; Advances in Wound Care; 2010 ; WHS

9/24/2010
6
WHY Topical
• Favorable route of administration– Time released formulations
• Lower risk noncompliance– Various formulations allow less frequent dressing changes
D d i k f b i l i• Decreased risk of bacterial resistance or antimicrobial cross‐resistance
• +/‐ cost savings• Lower risks
– cytotoxicity– adverse reaction
–all have risk contact dermatitis
WHY Topical continued
• Distribution and concentration profile opposite of systemic agents with respect to the target site
• Achieves highest concentration at target site/organsite/organ– Favored for delivery to epidermis or papillary cutis
– Useful for lower dermis or sub‐dermis
• Can be given concurrently with systemic therapies
PPID 6th ed; ch 35
Topical Antimicrobial DRESSINGS
• Honey
• Iodine
• Silvers
• Methylene Blue w/ Gentian Violet
• PHMB

9/24/2010
7
Honey
– Egyptians – early use
– Medicinal grade honey (Manuka)
– Leptosperum spp; New Zealand
– Various formulations
– Components include
• Inhibin → hydrogen peroxide & Gluconolactone …antimicrobial activity
• Propolis– mild antibiotic
• Creates acidic environment – pH 3.2‐4.5
Iodine
– Bacteriostatic and cidal
• no reported resistance
– Usually well tolerated
– Effective against
• Staphylococci spp including MRSA• Staphylococci spp including MRSA
• Streptococci spp
• Pseudomonas
• Anaerobes
– Debrides
– Three forms aqueous solutions
• all bacteriocidal
Iodine cont’d
• Cadexamer iodine– 0.9% in paste or ointment– Iodine released slowly over 48h as the base absorbs wound fluid– Preferred for use in proliferative phase of healing
• noncytotoxic and still kills bacteria
– Requires secondary dressing
• Caution– Thyroid dysfunction– Full thickness burns– Children– Pregnant women; lactating mothers
• Povidone iodine– recommended only for surgical scrubs and disinfecting intact
skin
• Contraindicated for pts w/ Iodine sensitivity

9/24/2010
8
Silver
• Many formulations– Elemental Ag or Ag+
– Binds to bacterial cell wall at multiple sites• Cell death by interference w/ cell replication; cell leak
– Resistance noted in GNRs
• Silver Sulfadiazine– Most rapidly absorbed– Can raise blood level of heavy metal– Contraindicated for < 2 y/o– Warning
• lactating mothers• renal dz• blood disorders
Silver cont’d
• Nano crystalline silver dressings– Not systemically toxic
– Faster healing rates
– Higher concentrations suggested for more infected wounds
• Highest concentration• Highest concentration– Acticoat
– Arglaes
• Selection of dressing dependent on – Size; depth; shape; tissue characteristics; amount of exudate
Sibbald et al; Advances Skin and Wound Care 2007; 20: 549
Methylene Blue w/ Gentian Violet
Hydrofera blue
Broad spectrum Bacteriostatic Absorbs bacteria in exudate B t i l i Bacteriolysis Singlet oxygen and free radicals
Unclear effect on tissue early in healing Requires moistening prior to application and secondary dressing Dressing changed when turns light or after 72h Available in rope or sheet (can cut to fit)

9/24/2010
9
Polyhexamethylene biguanide
Combination of cationic biguanide groups interspersed between hydrophobic hexamethylene groups
Binds to negatively charged organisms Bacteriocidal
PHMB
Cell wall disruption
GNR; GPC including MRSA; VRE; molds and yeasts
Activity independent of wound fluid Biosynthesized cellulose delivers PHMB to wound
Autolytic debridement
Available in blended gauze and a nonwoven drain sponge
Maintains moisture balance
wormandflowers.wordpress.com
TOPICAL ANTIBIOTICS
• Bacitracin– Polypeptide produced by Bacillus subtilis
– A, B, C – subgroups
– A = major constituent of commercial preparationsA = major constituent of commercial preparations
– Binds to bacterial cell wall and stunts its growth
– Primarily for Staph and Strep spp
– Minor toxicity profile
• some irritation
– May cross react with Polymyxin B

9/24/2010
10
Topical Antibiotics
• Neomycin – Aminoglycoside
– Isolated from Streptomyces fradiae
– Inhibits protein synthesis ‐ binds 30S ribosomal subunit & may inhibit DNA polymerasey p y
– Broad spectrum activity
– Reported resistance = Plasmid mediated• Cross resistance to other AG atbx is possible
– Not absorbed through intact skin
– Can be absorbed through denuded or damaged epithelium
Neomycin cont’d
• Systemic toxicities likely if absorbed
– Irreversible ototoxicity; cilia/hair cells
– Renal clearanceRenal clearance
• Contact sensitivity
– Prevalence 1‐6%
– Incidence 3‐ 6%
– Has its own ICD‐9 code
• Cross reactivity
Topical Antibiotics
• Polymyxin B– Isolated from Bacillus polymyxa; soil organism
– Destroys bacterial membranes with surface detergent‐like interaction; increases celldetergent like interaction; increases cell permeability
– Mostly active against gram negative organisms
– Added to cocktail compound for broader use
– Little systemic absorption due to size

9/24/2010
11
Topical Antibiotics
• Mupirocin (bactroban)
– Formerly aka pseudononic acid
• major metabolite derived from Pseudomonas fluorescens
– Inhibits bacterial RNA and protein synthesis by binding to tRNA synthetasey
– Does not cross react w/ other topicals
– Broad gram positive and negative coverage
– Resistance not uncommon
– Rare systemic absorption
– Contact dermatitis reported
HOT FOOT
9/06
What to treatWhat to treat WITHWITH ????

9/24/2010
12
Core Systemic Oral Antimicrobials useful in the Outpatient Setting
• � ‐lactams
• Sulfa – based• LincosamidesLincosamides
• Macrolides
• Quinolones• Tetracyclines• Oxazolidanone
� ‐lactams
All have similar chemical core structure: �‐lactam ring
–Penicillins Amino‐Penicillins
h ll ( k ) Anti ‐ staph Penicillins (risky)
–Cephalosporins Cephalexin : Keflex Cefuroxime : Ceftin
Loracarbef : Lorabid Cefpodoxime : Vantin
Ceftibutin : Cedax
PPPs
• Mechanism of Action for all βeta‐lactams– Inhibits bacterial cell wall development; Cell lysis
• Oral or intravenous administration routes
• Interstitial nephritis – penicillins
• Renal dosing
• Tetracycline antagonism ?• Tetracycline antagonism ?
• PCNs = gold standard for Gp A Strep infections
• Don’t rely on anti‐staph PCNs for tx of MSSA– Erratic to poor absorption
– 1st Gen Cephalosporin preferred – even over 3rd Generation agent
• The only 3rd Gen CSP with good anti‐MSSA activity is Cefpodoxime : Vantin

9/24/2010
13
Sulfonamide Folate Antagonist
• Trimethoprim – sulfamethoxazole
– Bactrim; Septra
• Bacteriocidal as compound
• Single or Double strengthSingle or Double strength
– (80/400 or 160/800)
• If allergy – due to sulfa; trimethoprim active as static
• Coverage equivalent to IV Ceftriaxone
PPPs
• Mechanism of cell kill similar for pathogen and host’s cells
• Wide range of dosages; pt dependent
– 1 ss bid to 2 ds tid
– Renal clearance
– Higher doses = incr’d marrow suppression
• Interactions
– Incr’d coumadin, methotrexate and dilantin levels,
– Rifampin decreases levels of TMP‐SMX
• Sulfa allergy ‐ contraindicated
– Rash; welts; itching
• Hemolytic anemia ‐ consider G6PD level
• Hyperkalemia, increased activity of oral sulfonylureas
• Photosensitivity
• Drug fever
Lincosamide
• Clindamycin : Cleocin
• Bacteriocidal
– Binds 50S ribosomal subunit causes early chain termination
N i l d i• Nonequivalent dosing
– IV ‐ 300mg ‐ 900mg q 6‐8 hrs
– PO – 150mg – 300mg q 6–8 hrs
• Resistance to EES presumes resistance to clinda; d‐test

9/24/2010
14
PPPs
• Risk of C. difficile• Oral > Parenteral
• Additional uses despite Staph resistanceAdditional uses despite Staph resistance• Antitoxin
• Anaerobic coverage
• Misses ~ 15% non‐aureus staph spp
Macrolides
• Inhibit 50‐s ribosomal subunits– prevents polypeptide synthesis
• Clarithromycin : BiaxinE th i EES• Erythromycin : EES
• Azithromycin : Zithromax– Tri‐pak ‐ 3 day dosing equivalent to 7d tx
– Z‐pac ‐ 5 day dosing equivalent to 7‐10 d tx
• Largely responsible for pcn‐resistant strep pneumo
• Can cause irritative diarrhea
PPPs
• Effectiveness against Groups A & B Strep decreasing

9/24/2010
15
msnbc.msn.com Grain of willow pollen has wedged between flower petals.
Quinolones
–Ciprofloxacin : Cipro–Levofloxacin : Levaquin–Levofloxacin : Levaquin–Moxifloxacin : Avelox
PPP
• NOT Gram Positive drugs
• Mental Status changes in elderly
• Lowers seizure threshold; QT l i h i i iprolongation; photosensitivity
• Achilles tendon rupture
• Appropriate dosing information for pts
– cations

9/24/2010
16
Tetracyclines
• Inhibits protein synthesis Binds 30s ribosomal subunit and–Binds 30s ribosomal subunit and blocks tRNA
• Sumycin• Vibratabs • Minocycline• Doxycycline
PPPs
• Bacteriostatic as single drug
• Stains teeth in pts < 8 yrs old
• Photosensitivity
• Wide range of dosing strengths
100 bid– 100 bid
– 500 qid
• GI intolerance – Vibratabs better tolerated
• Favorable pricing
PPPs
• Tetracycline sensitivity ≠ to Doxycycline sensi vity– Request lab to ck
• Take 2h before/after meal and any cations
– Magnesium, calcium, milk, dairy, cheese, yogurt, ice cream, rolaids, tumsrolaids, tums
– Instruct on correct dosing
• Minocycline
– superior; more reliable anti‐MRSA/MSSA– One of few oral agents active against VRE
• Doxycycline – MRSA treatment failures occur

9/24/2010
17
Oxazolidonone
Linezolid : Zyvox• 600 mg q 12h
– Equivalent dosingIV l• IV = oral
• Highly effective against• MSSA• MRSA• VRE• VSE
PPPs
• Baseline and weekly cbc – Consider addition of daily pyridoxine
• Caution w/ SSRI’s– Serotonin syndrome
– Fever ; delirium; htn; tremors
• Peripheral neuropathy
• Month of therapy may be ~ $3000
• Preauthorization
• Hefty copay
Dandelion pollen at 800X byteland.org

9/24/2010
18
Systemic Intravenous Therapy in the Outpatient Setting
• Patient selectionInsurance coverage
Social issues
Support systempp y
• Driven by frequency of administration
• Once daily vs multiple dosing preferred Consider cad‐pump
• May require PICC/central accessEspecially if tx longer than 10‐14 days
Intravenous options
• Cephalosporins– Ceftriaxone : Rocephin
• Carbapenem– Ertapenem : Invanz
• Televancin : Vibativ
• Vancomycin : Vancocin
• Daptomycin : Cubicin
CeftriaxoneRocephin
• 1 – 2 grams q day or bid
• Similar coverage as oral BactrimSimilar coverage as oral Bactrim– Good bridge
• Renal dose

9/24/2010
19
PPP
• True PCN allergy = high risk
– First dose in monitored setting
• No oral equivalent
– Bactrim closest
• Fairly broad spectrum coverage
Not MRSA
ErtapenamInvanz
– Broad spectrum ‐ GNRs and anaerobes
• No MRSA coverage
– DOC initial therapy DFU
– Excellent outpatient / home infusion drug
– Daily dosing
• 1 gram normal renal function
• ½ gram if reduced Creatinine Clearance
PPP’s
• Somnolence in elderly
• Renal dosing
• Broad spectrum
• No coverage for
– MRSA or Ps aeruginosa

9/24/2010
20
VancomycinVancocin
• Bacteriocidal– Concentration dependent killing
• 10‐20mg/kg bid (? daily)
• Peaks 30‐50 / troughs 10‐18
• Weekly labs– cbc, pk & tr’s; chemistries
• Penetrates lung tissue
PPP
• Gram positive organisms only– Tolerance common
• Marrow Suppressive
• Considerations for Optimum use– BID dosing required for maintenance of g qtherapeutic blood levels
– Lengthy infusion times; large volumes
– Red Man Syndrome ‐ histamine related
• Greater costs for weekly labs
• Predisposes for VRE
• Cell lysis – immunologic trigger ?
• MICs rising

9/24/2010
21
DaptomycinCubicin
• Indicated for SSSIs & Right Sided endocarditis
• Bacteriocidal for all GPCs– Without cell lysis
• 4‐6 (6‐8) mg/kg once daily– IVP or over 30 mins
• Baseline and weekly– CPK, creatinine
• Does not require central access
Daptomycin cont’d
• Mechanism of action
– Irreversible calcium dependent binding to cell membrane
– Inserts large tail of molecule into GP cell wall
P t i ffl– Potassium efflux
– Penetrates biofilm
• Rapidly cidal
– Causes multiple failures in organism biosystems
• DNA / RNA synthesis
• Protein synthesis
TelevancinVibativ
• SSSI’s
• Inhibits bacterial cell wall synthesis
• 7‐10 mg/kg per day intravenous
• Infusion over one hour
• Renal dosing

9/24/2010
22
PPP
• Daily dosing – one hour minimum
• Taste disturbance; N/V
• Red Man Syndrome
• QTc prolongationQTc prolongation – > 60 msec in 1.5% study pts vs 0.6% Vanco pts
• AVOID use w/ other agents that cause QT prolongation (Clarithromycin; Moxifloxacin)
• Animal data suggests fetal harm possible– Serum pregnancy test recommended
The culprit for most non‐healing wounds
MRSA
• 1998‐2004 – Staph aureus responsible for 44% SSSI’s– 35% MRSA
• 2005 – CDC serious/invasive MRSAf– ~ 94,360 infections
– ~ 18,650 deaths
– 2008 ~ 12 million physician visits for suspected MRSA
• 2009 – SSSI’s– 59% ‐MRSA– 14% ‐Invasive disease

9/24/2010
23
MRSA
• ~ 30% normal individuals carry S.aureus in anterior nares
• Broad spectrum of disease
– Cellulitis
– Endocarditis
– Necrotizing pneumonia
– Disseminated invasive osteomyelitis
Odds Ratio: MRSA or not?
Risk fx OR (95% CI)• ATBX within last month 2.4
• Abscess 1.8
• Reported spider bite 2.8
• Underlying illness .3
• Hx MRSA infx 3.3
• Close contact w/ other +MRSA 3.4
• Older age 0.9 (per decade of life)
• Snorting or smoking illicit drugs 2.9
• Incarceration w/ in last 12 mos 2.8
• Presentation w/ non skin infx .3
May et al JFP 5/09; vol 58, no 5

9/24/2010
24
9/09
How can WE ALL help decrease infections?