2. Oesophagus, Stomach and Digestive System
-
Upload
ka-heng-lian -
Category
Documents
-
view
81 -
download
4
Transcript of 2. Oesophagus, Stomach and Digestive System


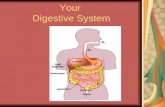
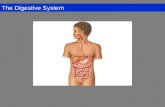
THE DIGESTIVE SYSTEM
The digestive system is made up of: gastrointestinal tract
accessory glands of the GI tract viz:1)The salivary glands2)Liver & gall bladder3) Pancreas

THE DIGESTIVE TRACT BEGINS AT THE MOUTH AND
ENDS AT THE ANUS
It is essentially a long tube , distended at one point ( the stomach)
Entry from one part into the next is limited by the “gates” which are closed unless food /chyme has to pass through


THE DIGESTIVE TRACT

Digestive processes
Ingestion…via mouth Propulsion…peristalsis Mechanical digestion…chewing,
mixing Chemical digestion…catabolic
steps from mouth to small intestine
Absorption…mainly in small intestine
Defeacation…removal of undigested stuff

Digestive processes
Initiated Mechanical & chemical stimuli
– Organ distension– Osmolarity– pH– Substates– End product of digestion
Regulated Intrinsic & extrinsic
– Hormones, short reflexes (local plexuses), long reflexes (autonomic nerves, CNS)

Pharynx (throat) is a common channel that conducts air & food
THE PHARYNX


DEGLUTITION
Buccal phase Pharyngeal phase Oesophageal phase

BUCCAL PHASE
food rolled into bolus
tongue arches to push it backwards

PHARANGEAL PHASE
elevation of soft palate (closes nasopharynx)
Pharynx is elevated

pressure of food on pharyngeal wall stimulates receptors; activates reflexes which (a) inhibit respiration (b) raise the larynx (c) close the glottis
passage of food bolus downwards tilts the epiglottis backwards
PHARANGEAL PHASE

a wave of contractions sweep through the pharyngeal muscles; food propelled towards upper oesophageal sphincter
PHARANGEAL PHASE

OESOPHAGEAL PHASE
reflex relaxation of upper oesophageal sphincter
sphincter closes when food has passed
glottis opens; breathing resumes
peristaltic waves propel food forward
lower oesophageal sphincter (LES) relaxes due to VIP and NO ; food enters stomach

THE STOMACH

Functional anatomy
Fundus : half- sphere; less circular muscle; mucus cells
Body: curved cylinder; “pacemaker” in greater curvature, at junction with fundus; numerous cells secreting mucus + HCl + pepsinogens
Antrum :cone-shaped; muscular; gastrin and IF secreted
Pylorus: circular muscle; ? true sphincter; gatekeeper (keeps bile from stomach)

NERVE SUPPLYParasympathetic cholinergic ( ACh) stimulatory effects on GI motility and
secretion relaxes sphincters ( contraction of radial
muscles of sphincters) Vagus supplies the oesophagus, small
intestines, and colon (up to the hepatic flexure).
Sympathetic adrenergic (NA) inhibit secretion
[Peptidergic; peptides like VIP ( vasoactive intestinal peptide) influence motility and secretion]

GASTRIC SECRETION & MOTILITY
Movement: slow waves;peristalsis; churning/mixing
Secretion: gastric juice ( HCl + pepsins +IF +mucus)
Function: storage; digestion of protein (fat,C/H); erythropoiesis (IF; abs.of iron) protection (HCl)
* Not very important for absorption!

BASIC ELECTRICAL RHYTHM- GASTRIC SLOW WAVES
GD PUMP- PROPULSION
OBLIQUE MUSCLES- CHURNING/ MIXING
RECEPTIVE RELAXATION
ANTI-PERISTALSIS

MOVEMENTS IN THE STOMACH
Peristaltic waves moves towards pylorus (>vigorous) >fluid chyme is pushed into duodenum >solid chyme squeezes back towards the body for
further mixing (churning)
PYLORIC VALVECLOSED
PYLORIC VALVE SLIGHTLY OPEN

GASTRIC EMPTYING
Rate depends upon volume of food consistency of food (liquid exit 1.5-2.5 hrs,
solid longer time, totally empty 3-4 hrs) contents (fats leave slowest) nervous control humoral factors (chemicals and hormones).
“gastroduodenal pump” = antrum , pylorus and duodenum act together (pylorus = gatekeeper).

GASTRIC EMPTYING
Stimulated by the vagus GASTRIN (hormone produced by the
stomach) Inhibited by Sympathetic stimulation hormones SECRETIN, CHOLECYSTOKININ
(CCK), GASTRIC INHIBITORY PEPTIDE (GIP) fats, acid and hyperosmotic substances in
the duodenum fear and anxiety.

The stomach musculature RELAXES before and after food gets into it:
“RECEPTIVE RELAXATION” :occurs when food is still in the oesophagus; vagally- mediated
“ADAPTIVE RELAXATION”: when food is in stomach (dilates in response to gastric filling); local nerve plexus (mediated by NO)
PLASTICITY: intrinsic ability to relax ( keeps intra-gastric pressure low)
P
T
P = 2T /r
[Law of Laplace]

The stomach musculature is rarely inactive…….
..soon after the stomach is emptied, mild contractions begin, gradually increasing in intensity over a few hours ( HUNGER CONTRACTIONS/ “HUNGER PANGS”)

BEGINS FROM OESOPHAGUS AND TRAVELS ALONG THE WHOLE GI TRACT
OCCURS EVERY 60-90 MINUTES
RELATED TO MOTILIN LEVELS IN BLOOD


Gastric glands and their secretions
*n eck m u cu s ce lls(m u cu s )
p arie ta l ce lls(oxyn c tic ce lls )
H C lIn trin s ic fac to r
ch ie f ce lls(p ep tic /zym og en ce lls )
p ep s in og en s I - V II
B od y o f s tom ach *
G as tric g lan d s
*antrum + pylorus secrete GASTRIN (from G cells) and mucus

GASTRIC JUICE( 2- 3 litres/day)
H C l:*ac tiva tes p ep s in og en*a id s iron ab sorp tion
*k ills in g es ted b ac te ria
P ep s in og en* in it ia tes p ro te in
d ig es tion
IN TR IN S IC F A C TO R* req u ired fo r ab sorp tion
o f B -1 2
W ater (m ore th an 9 8 % )+ m u cu s , H C l, P E P S IN O G E N S , IF

MECHANISM OF GASTRIC SECRETION (HCl)
The Vagus stimulates HCl secretion directly and indirectly through stimulation of GASTRIN release
Distension of the stomach also stimulates HCl secretion in both ways
Stimulation of HCl secretion occurs in response to * GASTRIN ** ACh *** Hi (histamine)**** PGE (prostaglandin E)

Source: Lamb et al
Stimulation of the VAGUS results in secretion of ACID brought about by (a) direct stimulation and (b) through stimulation of GASTRIN
HCl secretion
CNS
VAGUSGASTRIN
G CELLS
Polypeptides,secretagogues
DISTENSION
GASTRIN RELEASING PEPTIDE

3 Phases of Gastric Secretion
Cephalic phase Gastric phase Intestinal phase

CEPHALIC PHASE
parasym
Ach
Stimulates secretions by parietal & chief cells

GASTRIC PHASE
parasym
(secretion)
Food chemicals
G cells
Gastrin

INTESTINAL PHASE
Inhibit gastrin sec in duo
Aa,peptides, pH>3
Fat, pH<2
X

Digestion of carbohydrate
Average diet – starch, disaccharides, monosaccharides
Broken down to monosaccharides (glucose, fructose, galactose)
Lack enzymes to breakdown polysaccharides (eg cellulose), helps peristalsis

Digestion of carbohydrates
Salivary amylase– Starch to oligosaccharides– Works best at pH 6.75-7 (saliva
buffered by bicarbonate & phosphate)– Inactivated by stomach acid
Pancreatic amylase– Conversion continues in small
intestine

CYTOPLASMMICROVILLUS
MEMBRANEINTESTINAL LUMEN
STARCHAMYLASE
MALTOSEMALTASE 80%
GLUCOSE
LACTOSELACTASE
GALACTOSE
SUCROSESUCRASE
FRUCTOSEFACILITATED DIFFUSION (GLUT5)
Na+ACTIVE TRANSPORT
LACTASE DEFICIENCY = DIARRHOEA
INSULIN
INDEPENDENT
Recreated from Rhoades& Pflanzer; Ganong
Na+

Digestion of fats
Small intestine is the only site for fat digestion
Pancreas produces lipases Emulsification with bile salts

Bile salts are not absorbed until reaching ileum, form new micelles
CHYCLOMICRON
ABSORPTION OF LIPIDS

CYTOPLASMMICROVILLUS
MEMBRANEINTESTINAL LUMEN
RESYNTHESIS
LA
CT
EA
L
PORTAL CIRCU-
LATION
F/A, MG, Chol, Bile salts
Micelle
Bile salts are absorbed only in the ileum
LONG CHAIN F/A
[ Re- esterified into TG]
SHORT CHAIN F/A (water soluble)
CHYLO-MICRON
PROTEIN + PHOSPHOLIPIDS + CHOLESTEROL

Digestion of proteins
Proteins to amino acids Begins in the stomach
– Pepsinogens → pepsin (works in pH 1.5-2.5)
– Pepsin inactivated by high pH in duodenum In the small intestine
– Pancreas: Trypsin, chymotrypsin, carboxypeptidase,
– Brushborder enzymes: carboxypeptidase, aminopeptidase, dipeptidase


CYTOPLASMMICROVILLUS
MEMBRANEINTESTINAL LUMEN
TRIPEPTIDES
DIPEPTIDES
NEUTRAL A/A; Phen; Met
ACIDIC A/A
PEPTIDASES
Na+
5 transport systems
A/A
PORTAL CIRCU-
LATION
SMALL PEPTIDES
Undigested PROTEINS ENDOCYTOSIS
BASIC A/A
Fac. Dif.
H+

THANKS FOR YOUR ATTENTION……...
“I hear, I know,I see, I remember,I do, I understand.”
-Confucius 551BC-479BC