1. Renal System
Transcript of 1. Renal System

BASIC MEDICAL SCIENCES 2
CHAPTER 1 RENAL SYSTEM
INTERNATIONAL COLLEGE OF HEALTH SCIENCES (ICHS)

LEARNING OUTCOMESAt the end of this topic the students will know the:• Functions of the urinary system• External and internal anatomy and physiology
of the kidneys• Physiology of nephrons• Anatomy and physiology of ureters, urinary
bladder and urethra.• Mechanism of urine production.

THE URINARY THE URINARY SYSTEMSYSTEM
•The job of urinary system is to make urine, thereby controlling the body’s fluid and ion balance and eliminating waste products
•Helps keep the body in homeostasis by removing and restoring selected amounts of solutes and water from the blood.


WHAT ARE THE WHAT ARE THE URINARY ORGANS URINARY ORGANS
INVOLVED??INVOLVED??

STRUCTURE AND STRUCTURE AND FUNCTIONSFUNCTIONS
STRUCTURE FUNCTION
Kidney - Two kidneys (right and left), bean shaped organs- Filtration, regulation of blood volume, regulation of
solutes, pH of extra cellular fluid, RBC synthesis, Vit. D synthesis
- Makes urine
Ureters - Urine flows from kidneys to urinary bladder
Urinary bladder - Storage of urine
Urethra - Transports urine out from the urinary bladder

KIDNEYKIDNEY

KIDNEYKIDNEY• Paired organs, reddish in color and
bean-shaped• The main filtering organs of the
system, producing the urine.• Average adult kidney: 11.25 cm (4 inches) long5.0 to 7.5 cm (2-3 inches)

• Kidneys are located just above the waist between the parietal peritoneum and the posterior wall of abdomen (RETROPERITONEAL)
• Located between the twelfth thoracic and third lumbar vertebrae

FUNCTIONS OF KIDNEYFUNCTIONS OF KIDNEY1. EXCRETION: Removal of organic wastes
from body fluids like urea, Creatinine, uric acid and bilirubin
2. ELIMINATION: Discharge of harmful substances entering the body like drugs, toxins, heavy metals and pesticidies.
3. pH REGULATION: The kidneys control the proper balance of hydrogen ions in the blood.

4. HOMEOSTATIS : Kidney maintain water balance of body by excreting it when it is in excess, and conserving it when there is substantial loss of water.
- Kidneys also maintain electrolyte balance specially that of sodium

5. BLOOD PRESSURE: The kidney produce the enzyme RENIN, which helps adjust filtration pressure.
6. ERYTHROCYTE CONCENTRATION: The kidneys produce ERYTHROPOIETIN, a hormone that stimulates red blood cell production in red bone marrow.
• They help regulate the concentration of erythrocytes in the blood in cases of chronic hypoxia.

6. VITAMIN D PRODUCTION: The kidneys convert vitamin D to its active form (calciferol).
• Vitamin D is important for normal bone and teeth development.
• It also helps control calcium and phosphorus metabolism.

Renal artery
Interlobar arteries
Arcuate arteries
Interlobular arteries
Afferent arterioles
Glomerulus
Efferent arterioles
Peritubular capilaries
Interlobular veins
Arcuate veins
Interlobar veins
Renal vein
PATWAY OF BLOOD THROGH THE RENAL SYSTEM (RENAL BLOOD
VESSELS)

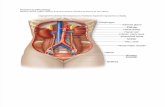
EXTERNAL ANATOMY OF THE KIDNEY
a. RENAL HILUM : gives kidney bean shape, root of renal arteries (bring blood to kidney), renal vein (brings blood out) and ureter (transport urine out)
b. RENAL SINUS: The entrance to a cavity in the kidney which is occupied by the renal pelvis, renal calyces, blood vessels, nerves and fat

a. Renal capsule • Innermost layer,
covers the kidney• Smooth transparent• It is a barrier against
infection and trauma to the kidney.
Three tissue layers protecting kidney are:

b. Adipose Capsule
• It is a mass of fatty tissue that protects the kidney from blows.
• Firmly holds the kidney in place in the abdominal cavity.
c. Renal Fascia
• Consist of a thin layer of fibrous connective tissue that also anchors the kidneys to their surrounding structures and to the abdominal wall.

INTERNAL ANATOMY OF KIDNEY

The kidney can be divided into three mainlayers:
Renal Cortex- Superficial region- The outer area of the kidney.
Renal Medulla- Middle layer of the kidney- Renal pyramids – cone shaped structures that make up the medulla.- Medullary rays – extend from the renal pyramids into the cortex. - Renal columns - consists of the same tissue as the cortex that projects between the renal pyramids. - Renal papillae – tips of the pyramids project toward renal sinus.

Renal Pelvis• Occupies a large portion of the renal
sinus • An open space which forms the ureter as
it exits the kidney • Forms the major and minor calyces
which enclose the papillae of the renal pyramids where each kidney contains 8 to 20 minor calyces and 2 to 3 major calyces.
– Minor calyces – funnel shaped chambers
into which the renal papillae extend.
– Major calyces – a larger funnel formed by the minor calyces of several pyramids

NEPHRONNEPHRON

NEPHRON The part that performs the real functions of the kidney consists of millions of microscopic funnels and tubules. These fundamental units are NEPHRONS
Each kidney contains 1,000,000 nephrons that filter the blood and form urine.
The number of nephrons does not increase after birth. When nephrons are damaged they are not replaced or regenerated.
Nephron is divided into two parts, Renal Corpuscle and Renal Tubule. Renal corpuscle is a site of filtration while Renal tubule is a site of reabsorption and secretion .

FOUR MAJOR FUNCTIONS OF NEPHRONS
1. Control blood concentration and volume by removing selected amounts of water and solutes.
2. Helps regulate blood pH.
3. Remove toxic waste from the blood.
4. Stimulate red blood cell production in red bone marrow by producing a hormone called ERYTHROPOIETIN.

RENAL CORPUSCLE Blood enters the renal RENAL
CORPUSCLE via GLOMERULUS a capillary ball.
It is surrounded by glomerular capsule or BOWMAN’S CAPSULE: A double-walled, cup-shaped structure around the glomerulus of each nephrons . The visceral layer of Bowman’s capsule.
It serves as a filter to remove organic wastes, excess inorganic salts, and water.
Filtered fluid moves into RENAL TUBULE.

FUNCTIONS OF RENAL CORPUSCLE
Glomerulus – capillary within Bowman’s capsule
Bowman’s Capsule• Enlarged terminal end of the nephron.
Indented to form a double walled chamber.
a. VISCERAL LAYER – Is the innermost layer of the capsule made of by podocytes.
It serves as a filter to remove organic wastes, excess inorganic salts, and water.
b. PARIETAL LAYER – Is the outermost layer of the capsule

Reabsorption occurs here.• Active transport pushes materials back into
circulatory system that are needed by the body
The parts are involved are as proximal tubule, loop of Henle (descending and ascending), distal tubule and collecting duct.
RENAL TUBULE

PROXIMAL TUBULE: is the first part of the renal tubule. PCT located in the cortex.
DESCENDING LOOP OF HENLE: Which narrows in diameter as it dips into the medulla of the kidney.
As the tubule straightens, it increases in diameter and ascends toward the cortex of the kidney called ASCENDING LOOP OF HENLE.
PATHWAY OF RENAL TUBULE

In the cortex, the tubule again becomes convoluted called DISTAL TUBULE.
The distal tubule ends by merging with a large straight COLLECTING DUCT.
The COLLECTING DUCT now pass through the RENAL PYRAMIDS and open into the CALYCES Of THE PELVIS through the number of larger papillary ducts.
They empty urine in the RENAL PELVIS


30
URINE FORMATION

THREE PROCESS OF URINE FORMATION
1. GLOMERULAR FILTRATIONRemoves water and these dissolved substancefrom the plasma of blood
a. Sodiumb. Potassiumc. Calcium
d. Magnesiume. bicarbonate,f. Sulfateg. Ureah. uric acid

2. TUBULAR REABSORPTION• This step is known as selective reabsorption because only
some elements are reabsorbed back into the body.
• This selective reabsorption takes place by the capillary network surrounding the proximal convoluted tubule, loop of Henle and distal convoluted tubule. Absorption takes place both by osmosis and by active transport.

3. TUBULAR SECRETION • This is the step where the urine is made concentrated by increasing the concentration of
waste elements. Substances move into the distal and collecting tubules from blood in the capillaries around these tubules.
• These substances are secreted by the mechanism of active transport. The substances secreted include a. hydrogen ionsb. potassium ionsc. Ammoniad. certain drugs or metabolic end products.
• The distal convoluted tubules then drain the urine into the collecting tubules. • Then, several collecting tubules join together to drain their contents into the collecting duct.• This then eventually reaches the renal pelvis, from where the urine flows into the ureter to
reach the urinary bladder.

URETER, BLADDER AND URETHRA

URETER• Ureter - Are
muscular tube that propel urine from the kidneys to the urinary bladder.
• Are the tubes that connect each kidney to the bladder.
35

BLADDER• Muscular sac that serves as a
reservoir for urine and stretches to accommodate urine.
• Collects urine excreted by the kidneys prior to disposal by urination.
36

URETHRA• In the human
male, the urethra is about 8 inches (20 cm) long and opens at the end of the penis. The urethra provides an exit for urine as well as semen during ejaculation.
• In the human female, the urethra is about 1+1/2–2 inches (2–5 cm) long and opens between the clitoris and the vaginal opening, extending from the internal to the external urethral orifice.
37

THANK YOU















![Exercise 9 - Renal System Physiology[1]](https://static.fdocuments.us/doc/165x107/553dd6134a7959502f8b47ca/exercise-9-renal-system-physiology1.jpg)

