Goal: to assist clients with reproductive decision making, enabling the client to have control in...
-
Upload
wilfrid-williamson -
Category
Documents
-
view
215 -
download
5
Transcript of Goal: to assist clients with reproductive decision making, enabling the client to have control in...

Sexual Development/ Human Sexuality/ Contraception
Prepared by:Teresa Fisher, PBT, RN, BSNRevised & Presented by: Judy Carlyle,
MSN, RN

Family Planning Goal: to assist clients with reproductive
decision making, enabling the client to have control in preventing pregnancy, limiting the number of children, spacing the time between children, and voluntarily interrupting pregnancy as desired.

So Many options; which one to choose?????
Safe Easily available Economical Available Simple to use Promptly reversible

Nurses Role in Contraception
Foster safe environment for consultation
Provide correct education Distinguish myth from fact Clarify misinformation Fill in gaps of knowledge Provide visual samples Gain a complete history

History should include
Menstrual history Contraceptive history Contraceptive goal Obstetric history Medical history Familial history

Methods of Contraception
Natural Methods 1) Abstinence 2) Coitus interruptus Fertility awareness methods 1) Calendar method 2) Basal body temperature method 3) Cervical mucus method 4) Symptothermal method

Methods of Contraception
Spermicides & barrier methods
* condoms * diaphragm * cervical cap * cervical sponge Hormonal methods Emergency
contraception Intrauterine devices Sterilization

Abstinence
The practice of avoiding sexual intercourse

Advantages
Safe Free Available to all 100% effective in preventing
pregnancy & STIs Can be initiated at any time Encourages communication between
partners

Disadvantages
Both participants must practice self-control

Nursing Education
Teach alternative methods of obtaining sexual pleasure
Provide positive feedback to clients who desire and maintain abstinence

Coitus Interruptus
AKA withdrawal Male partner
withdraws penis prior to ejaculation
Effectiveness depends on man’s ability to withdraw prior to ejaculation

Advantages
Can be practiced at any time during the menstrual cycle
Free

Disadvantages One of the least reliable contraceptive
methods Only 80% effective Does not protect from STIs Some pre-ejaculatory fluid, which may
contain sperm, may escape from the penis during the excitement phase prior to ejaculation
At the peak of sexual excitement, exercising self-control may be difficult

Nursing Education
Before engaging in sexual intercourse, the male should urinate and wipe off the tip of the penis to decrease the potential of introducing sperm into the vagina
Conception may occur if pre-ejaculatory fluid containing sperm enters the vagina
A spermicide or post-coital contraceptive may be needed if the female partner is exposed to sperm

Fertility Awareness Methods
Calendar based methods
Symptoms based method
Biologic marker methods

Advantages
Free Safe Acceptable to couples whose religious
beliefs prohibit other methods, such as Roman Catholics
Increases awareness of the woman’s body
Encourages couple communication Can be used to prevent or plan a
pregnancy

Disadvantages
Requires extensive initial counseling and education
May interfere with sexual spontaneity May be difficult or impossible for
women with irregular menstrual cycles Used alone, they offer no protection
against sexually transmitted infection Less effective in actual use

Calendar Rhythm Method
Based on assumption that ovulation occurs 14 days prior to the next menses, sperm are viable for 5 days, and the ovum is capable of being fertilized for 24 hours
91% effective if used perfectly

Calendar rhythm method
Based on number of days in each cycle, counting from first day of menses
Beginning of fertile period is estimated by subtracting 18 days from length of shortest cycle in last 6 months
End of fertile period is determined by subtracting 11 days from length of longest cycle

Example of Calendar Rhythm Method
Shortest cycle 24 days 24-18 = 6th day
Longest cycle 30 days 30 -11 = 19th day
• To avoid conception the couple would abstain during the fertile period days 6-19

Lets Try One
You are educating a client on the contraceptive calendar rhythm method. When you ask her how long her cycles have been for the last 6 months, she explains that her cycle is consistently 28 days. What days should you tell her to abstain from sexual intercourse???

Let’s Work This Together
Shortest cycle 28 days 28 -18 = 10th day
Longest cycle 28 days 28 – 11 = 17th day
To avoid pregnancy the couple abstains from day 10-17.

Disadvantage To Calendar Rhythm Method
Attempting to predict future events with past data

Standard Days Method A modified form of calendar rhythm
method Has fixed number of days of fertility for
each cycle Day 8 – 19 Cycle Beads (bracelet) Is useful for women who have 26-32 day
cycle Unreliable for others 12% failure rate

Cervical Mucus Method Based on monitoring and recording of
cervical secretions
Cervical mucus changes occur in response to levels of estrogen and progesterone
Spinnbarkeit – Watery thin, clear mucus becomes more abundant and thick. Feels similar to a lubricant and can be stretched 5+ cm between the thumb and forefinger

Spinnbarkeit
Presence indicates period of maximal fertility
Sperm deposited in this type of mucus can survive until ovulation occurs

Cervical Mucus in Relation to Conception
Cervical mucus that accompanies ovulation is necessary for viability & motility of sperm
Mucus alters pH by neutralizing acid

Barriers to Assessing Mucus Contraceptive gels or foams Vaginal infection Douches Vaginal deodorant Medications (antihistamines dry up
mucus) Sexually aroused state thins mucus Uncomfortable touching genitals

Education
Assess cervical mucus daily Avoid intercourse when first notices
cervical mucus becoming more clear, elastic, and slippery and then for 4 days
Instruct women on barriers to cervical mucus assessment

Basal Body Temperature Method
BBT is lowest body temperature of a healthy person taken immediately after waking and before getting out of bed
BBT varies from 36.2-36.3 during menses and 5 - 7 days after
At time of ovulation there is a slight decrease in temperature (fertile period)
After ovulation the BBT increases slightly and remains until 2-4 days prior to menstruation

Basal Body Temperature Method
Fertile period is day of first temp drop or first elevation through 3 days of elevated temp
Abstinence begins the first day of menstrual bleeding and lasts through 3 consecutive days of sustained temp rise

Basal Body Temperature Method
Temps are recorded on graph97% effective if performed correctly

Alterations in BBT Accuracy
Infection Fatigue Less than 3 hours sleep per night Awakening late Anxiety New thermometer Jet lag Alcohol Antipyretic medications Heated waterbed Electric blanket

Combination contraception
Calendar rhythm method Two day method BBT

Urine Ovulation Predictor Test
Detects the sudden surge of luteinizing hormone (LH) that occurs 12-24 hours before ovulation
Test is not affected by illness, emotional upset, or physical activity

Mechanical Methods of Contraception
Spermicide Male condom Female condom Diaphragm Cervical cap Contraceptive sponge Intrauterine device (IUD)

Spermicides
Serve as chemical barriers against the sperm
Nonoxynol-9 (N-9) work by reducing the sperm’s mobility
Attacks sperm flagella and body so they cannot reach the cervical os
Use of N-9 too often could increase transmission of HIV by disrupting vaginal mucosa

Intravaginal spermicides Foams Tablets Suppositories Creams Films Gels Preloaded single-dose applicators Inserted high in vagina to reach cervix Inserted 15 min – 1 hr before sexual
intercourse When used alone 94% effective

Advantages
No prescription required May be used alone or with a diaphragm
or condom May add additional lubrication and
moisture Penis can remain in vagina following
ejaculation Safe for breast-feeding women Several choices

Disadvantages
The spermicide may be irritating to one or both clients
Some forms may be perceived as messy
May interfere with spontaneity

Nursing Education
Apply spermicide inside vagina & close to the cervix prior to inserting penis
Spermicides must be applied with each act of sexual intercourse
Onset of spermicidal action varies When used alone effectiveness lasts no longer
than 1 hour Foams, creams, & gels are effective
immediately Vaginal contraceptive film & suppositories
become effective 15 minutes after insertion into vagina

Male Condoms Are made of latex, polyurethane, or
animal tissue Polyurethane is thinner and stronger
than latex Protects against pregnancy and some
STIs Latex condoms will break down with
oil-based lubricants Only water-based or silicone lubricants
should be used

Advantages Males are able to participate in
contraception Sexual intercourse may be prolonged Condoms are available in a variety of
sizes & styles at low cost or free Partners can participate in placing the
condom to enhance enjoyment All condoms except those made of
natural skins offer protection against pregnancy

Natural Skin Male Condoms Natural skin condoms (lamb cecum)
does not provide same protection against STIs & HIV
Contain small pores that could allow passage of viruses such as hepatitis B, HSV, & HIV

Disadvantages
Penis must be erect before placing the condom on
To prevent spillage of semen, the male must withdraw after ejaculating, while the penis is still erect
Condoms can rupture or leak Oil-based lubricants can decrease
effectiveness of condom

Use of the Male Condom
Make sure to educate on proper use and fit
Condom should be in place prior to any penile penetration

Client Education Check expiration date on package Avoid using oil-based lubricants Put on condom by placing condom on the tip of the
erect penis, leaving enough room at tip to collect sperm, then unroll condom from tip of erect penis to base
After intercourse erect penis should be withdrawn from vagina while holding rim of condom to prevent leakage
Inspect used condom for tears or holes Discard used condom in disposable waste container Do not flush in toilet

Female Condom Thin, polyurethane sheath with flexible
rings at each end, which covers cervix, lines vagina, and partially shields perineum
95% effective with perfect use

Female Condom

Insertion of Female Condom

Advantages
May be inserted up to 8 hours prior to intercourse
Not made of latex Both partners are protected against
STIs Available without prescription Use of lubricants will not decrease
effectiveness Breast-feeding women can safely use

Disadvantages
May twist or slip during intercourse Improper removal results in risk of
ejaculate leaking Outer ring may irritate external
genitalia High cost Noise produced with intercourse Altered sensation Initial insertion may be awkward

Client Education
Insert closed end of condom into vagina so ring fits loosely against cervix
After intercourse, condom should be removed before standing up by squeezing and twisting outer ring to close sheath while gently pulling out of vagina

Diaphragms
A shallow dome-shaped latex or silicone device with a flexible rim that covers cervix.

Advantages
Gives woman control Partner may insert diaphragm as part
of foreplay Diaphragm contains no hormones and
is safe for breast-feeding client Penis can remain inside vagina after
ejaculation

Disadvantages
Must be fitted by healthcare provider Must be replaced every 2 years Refitting & replacement may be
needed following pregnancy or a 15 pound weight gain or loss (20% weight fluctuation)
Difficulty with learning how to place correctly
Should not be used if client has UTI or TSS or history of either

Diaphragms
Available in many sizes Should be largest size woman can wear
without her being aware of its presence Most effective when used with
spermicide Annual gynecologic exam to assess fit Inspect device prior to each use

Inspecting Diaphragm Hold diaphragm up to light source Carefully stretch at area of the rim, on
all sides Make sure there are no holes Sharp fingernails can puncture
diaphragm Can fill diaphragm with water to
assess for holes If diaphragm is puckered do not use

Insertion of a Diaphragm Can be inserted up to 6 hours prior to intercourse Hold diaphragm between thumb and fingers Dome can be up or down Insert inward and downward as far as it will go Do not use oil based products such as vaginal
lubricants b/c they weaken the rubber

Disadvantages of Diaphragms
Diaphragms are contraindicated for women with pelvic relaxation,
uterine prolapse, or large cystocele.
Not a good option for women with poor vaginal muscle tone or recurrent UTIs
Toxic shock syndrome TSS can occur

Toxic Shock Syndrome Remove diaphragm within 6-8 hours after intercourse Do not use diaphragm or cervical cap during menses
Watch for danger signs of TSS * Sunburn type rash * diarrhea * dizziness * faintness * sudden high fever * vomiting * weakness * sore throat * aching muscles and joints

Client Education
Should be inserted 6 hours prior to sexual intercourse
Should remain 6 hours after sexual intercourse

Cervical Cap
Small thimble-shaped device Made of soft rubber Fits over cervix Held in place by suction Acts as barrier b/t sperm & cervix Effectiveness determined by
childbearing hx Nulliparous – 91% effective Parous = 74% effective

Cervical Cap
Three types Advantages & disadvantages
same as diaphragm Should remain in place for at
least 6 hours and no more than 48 hours after intercourse
Provides a physical barrier to sperm
Spermicide is inside the cap

Cervical Cap
Fits the same way as a diaphragm Requires less spermicide than the
diaphragm Can be inserted hours before sexual
intercourse without need for additional spermicide
Repeated acts of intercourse are possible
There is a potential risk of TSS

Cervical Cap

Contraceptive Sponge
Small, round polyurethane sponge that contains N-9 spermicide
Designed to fit over cervix One size fits all One side is concave Other side has woven
polyester loop to be used for removal of sponge
Before insertion, sponge must be moistened with water

Contraceptive Sponge Provides protection for 24 hours Should be left in place for at least 6
hours after last intercourse Wearing longer than 24 hours places
women at risk for TSS

Contraceptive Sponge

Hormonal Methods
More than 30 different formulations Oral Transdermal Vaginal Injectable Emergency Intrauterine

Combined oral contraceptives (estrogen – progestin)
AKA COCs Suppress the action of the hypothalamus
& anterior pituitary which leads to insufficient secretion of FSH & LH
Follicles do not mature Ovulation is inhibited Should be taken at the same time each day

COC
Available in 21 day, 28 day, 91 day packages
99.1% effective if used perfectly

COC Regimen
Is initiated on the first Sunday after day one of the menstrual cycle or after childbirth or abortion
Another form of contraception should be used throughout the first week
Taken the same time each day Almost 100% effective Almost all failures are a result of omission
of one or more pills during regimen

COCs
From 1-4 days after last COC, the endometrium soughs and bleeds
Due to hormone withdrawal
Bleeding is less profuse than normal menstruation
May only last 2-3 days

What to do if COC is Missed
If one pill is missed: * take pill immediately * begin regimen with time new
pill taken * no alternate forms of contraception is necessary

What to do if COC is Missed
If two pills are missed * Take one pill every day until
Sunday * Begin new pack on Sunday * Do not take 2 pills at same time * Use backup contraception for one week

Advantages of COCs Does not effect sexual act Improvement in sexual response may occur
once possibility of pregnancy is not an issue
Convenience of knowing when next menstrual flow will occur
Decreased menstrual blood loss Decreased iron-deficiency anemia Regulation of irregular cycles Reduced incidence of dysmenorrhea & PMS Return to fertility happens quickly

Disadvantages
No protection against STIs Clients need to remember to take a pill
at the same time each day Clients with preexisting medical
problems may not be candidates for this method
Effectiveness may be decreased with certain medications
May decrease effectiveness of insulin or warfarin (coumadin)

Contraindications include HX. Of:
thromboembolic disorders cerebrovascular or coronary artery disease breast cancer Estrogen dependent neoplasms Currently pregnant, lactation <6 weeks
postpartum Smokes >35 years old Hypertension DM with vascular disease Surgery on legs gallbladder disease

Common Side Effects
Nausea Breast tenderness Fluid retention Chloasma (klo – as-mah) Increased appetite Tiredness Depression Breast tenderness Hirsutism Bleeding irregularities

Serious Adverse Effects
Attributable to estrogen, progestin, or both
Stroke MI Thromboembolism Hypertension Gallbladder disease Liver tumors

Finding the Right COC
The right product for a woman contains the lowest dose or hormones that prevents ovulation and that has the fewest and least harmful side effects

Effectiveness is Altered When Women also Take:
phenytoin (Dilantin) topirimate (Topamax) ampicillin (Omnipen) tetracycline (Achromycin) penobarbital rifampin (Rifadin) Anti-HIV inhibitors St. John’s wort

Nursing Considerations
A drop of blood or small brown smear counts as a period
All women taking oral contraceptives should be aware of alternate methods of contraception
Assure woman knows that oral contraceptives will not protect them from STIs or HIV

Oral Contraceptive 91-Day Regimen
Some women take COCs in 3 month cycles
Have fewer menstrual periods Seasonale
› Take 3 months of active pills followed by 1 week of inactive pills
› Menstrual period occur during 13th week› If 13th week period does not occur, woman
should consider pregnancy

Transdermal Contraceptive System
Small continuous levels of progesterone and estrogen are released to suppress ovulation
Applied to intact skin of upper outer arms, upper torso, lower abdomen & buttocks

Advantages
Patch requires only weekly application Patch stays on even when showering
and swimming

Disadvantages
No protection against sexually transmitted infections
Not recommended for obese women, or women with skin disorders
Clients with preexisting medical diseases may not be candidates for this method
Medication precautions are same as oral contraceptives

Client Education
Do not apply to breasts Apply same day once a week for 3
weeks Followed by week without patch Failure rate < 8% in women weighing
less than 198 pounds

Vaginal Contraceptive Ring
Available only with a prescription Flexible ring made of ethylene
vinyl Worn in the vagina to deliver
continuous levels of progesterone & estrogen
Worn for 3 weeks Followed by 1 week without ring Bleeding occurs during ring free
week

Advantages
Requires application only once every 4 weeks
Requires no special fitting Can safely be left in place during
exercise or intercourse

Disadvantages
Offers no protection against sexually transmitted infections
Clients with marked vaginal prolapse should be cautioned to check for expulsion
Med precautions are same as taking oral contraceptives

Vaginal ring insertion
Ring is inserted by woman Does not have to be fitted If woman or partner notices discomfort
during coitus, ring can be removed and still be effective up to 3 hours
Failure rate is < 8 %


Progestin-Only Contraceptives
Impair fertility by inhibiting ovulation, thickening and decreasing the amount of cervical mucus, thinning the endometrium, and altering cilia in the uterine tubes
Oral Injectable Implantable

Advantages
95.5% effective
May be used by: * lactating women * women with mild hypertension

Oral Progestin (Minipill)
Failure rate 1-10% Must be taken correctly to increase
effectiveness Must be taken at same time every day

Oral Progestin (minipill)
If client misses one pill * missed pill should be taken immediately * next pill taken at regular time * Additional method of
contraception through end of that cycle

Injectable Progestin
Depo-provera Given IM or subcutaneously
4 times a year Should be initiated during
first 5 days of menstrual cycle
Administered every 11-13 weeks
97.7% effective

Depo-provera
Blocks the luteinizing hormone surge Suppresses ovulation Thickens cervical mucus to prevent
penetration of sperm

Important Education
Subsequent dose must be given 80-90 days after previous dose for continuous contraceptive protection
Return of fertility may be delayed up to 1 year after stopping this method

Implantable Progestins
Norplant 6 Implants are inserted
under the skin of the woman’s arm
Effective up to 3 years Prevent ovulatory
cycles, thicken cervical mucus

Side Effects of Implantable Progestins
Irregular menstrual bleeding HA Nervousness Nausea Skin changes Vertigo

Advantages
Not user-dependent for effectiveness 99.95% effective Does not contain estrogen Effective within 24 hours Lasts up to 5 years

Disadvantages
Minor surgery for insertion & removal May be visible under skin Irregular or prolonged menses No protection against STI Slightly higher failure rates in women
>154 pounds in fifth year of use

Emergency Contraception
Plan B Available without a
prescription Is available in 1 or 2 dose
regimens Should be taken by women
as soon as possible within 120 hours of unprotected intercourse, or birth control mishap
Risk of pregnancy is reduced by 75% - 89%

Emergency Contraception
If taken before ovulation emergency contraception prevents ovulation by inhibiting follicular development
If taken after ovulation there is little effect on ovarian hormone production or endometrium
If woman does not begin menstruation within 21 days, she should be evaluated for pregnancy
Is ineffective if the woman is pregnant because the pills do not disturb an implanted pregnancy

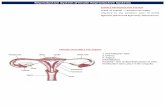
Intrauterine Device
A small T-shaped device with bendable arms for insertion through the cervix into the uterus
Mirena – releases levonorgestrel gradually from a reservoir
Impairs sperm motility, thickens cervical mucus, decreases lining of uterus
Uterine cramping & bleeding is decreased Effective for 5 years

Mirena
Provider inserts against uterine fundus Arms open near fallopian tubes Adversely affect sperm motility &
irritate lining of uterus Failure rate < 1%

Mirena
2 strings hang from base of stem through cervix & protrude into vagina
Woman must have negative pregnancy test, cervical cultures to rule out STIs & consent form signed

Advantages to IUD (Mirena)
Long-term protection Highly effective Continuous protection Good option for women
who cannot use hormone contraception, breastfeeding, >35, or smoke
Immediate return to fertility when removed

Disadvantages to IUD
Has to be inserted by healthcare provider
Risk of PID Unintentional expulsion of device Infection Possible uterine perforation No protection against HIV or STIs

Nursing Considerations
Teach woman to check for strings once a week for first month then once a month after menstruation

Signs of Potential Complications with IUD
P – period late, abnormal A – abdominal pain; pain with
intercourse I – Infection exposure, abnormal vag d/c N – not feeling well, fever, chills S - string missing, shorter, longer

Sterilization
Refers to surgical procedures intended to render a person infertile
Involves the occlusion of the passageways for the ova & sperm
Woman – uterine tubes are occluded Men – vas deferens are occluded Only a hysterectomy or oopherectomy
guarantees absolute sterility in women

Tubal Ligation
Fallopian tubes are accessed through two small incisions into the abdomen and visualized using a laparoscope
They are cut, tied, cauterized, or banded to block passage of sperm & prevent ovum from becoming fertilized
96-99% effective

Tubal ligation
Takes 20-30 minutes Performed under general or local
anesthesia Pain for several days Avoid tub baths for 48 hours Avoid driving, lifting, & strenuous
activity for 1 week

Tubal Ligation
Health care provider must be certain woman is not pregnant
½ are performed immediately after pregnancy

Advantages
Permanent and effective in preventing pregnancy
May be performed at any time Immediately after childbirth is optimal
b/c uterus is enlarged and fallopian tubes are easily identifiable
Sexual function and spontaneity are not affected

Disadvantages
Requires outpatient surgery Potential complications such as infection &
bleeding If pregnancy does occur risk for ectopic
pregnancy is increased Reversal of procedure is not always possible Sterilization offers no protection from STIs May feel pain at ovulation The ovum disintegrates within the
abdominal cavity

Male Sterilization
AKA vasectomy Sealing, tying, or cutting vas deferens Sperm cannot travel from testes to
penis Done on outpatient basis Permanent method of sterilization Reversal is generally unsuccessful

Advantages
99.85% effective Recovery time is short Simpler, safer, and more effective than
female sterilization Complications are rare Sexual function is not affected Cost effective Convenient

Disadvantages
Very unlikely that it can be reversed
Potential complications include adverse infection, bleeding, sperm granuloma or spontaneous re-anastomosis of vas deferens

Vasectomy
Ice packs applied to scrotum intermittently for a few hours after surgery
Scrotal support Moderate inactivity for 2 days Suture removed 5-7 days postop Sexual intercourse resumed as desired

Considerations
Sterility is not immediate Some sperm remain in proximal
portions of sperm ducts Takes 1 week to several months to
clear ducts of sperm Alternate contraception should be
utilized until 2 sperm counts come back as zero

Vasectomy

Vasectomy

Sexual Function
Explain to male that ability to achieve and maintain erection or volume of ejaculate is not altered
Sperm production continues but are unable to leave epididymis

Laws & Regulations
Informed consent Always!!! Voluntary sterilization of any mature,
rational woman without reference to marital or pregnancy status
Partner’s consent is not required Partners are encouraged to discuss
situation with each other Health care provider may request consent Sterilization of minors is restricted

Laws & Regualtions if Using Federal Funds
Person must be 21 years old
Irreversible method of birth control and a statement that mandates a 30-day waiting period between giving consent and the sterilization

Induced Abortion
Purposeful interruption of pregnancy before 20 weeks of gestation
Elective abortion - is done at woman’s request
Therapeutic abortion – performed for reasons of maternal or fetal health or disease

Indications for woman’s decision to have an
abortion Preservation of life & health of mother Genetic disorders of fetus Rape or incest Pregnant woman’s request

Rowe VS Wade
Abortion is now regulated Prior to 1970 was not legal January 1973 Supreme court legalized
abortion

Trimester approach
First trimester abortion is permissible Different states have different laws
regarding second trimester abortions Third trimester abortions are limited &
may be prohibited by state regulations unless it interferes with life or health or pregnant woman

Attempted Abortion Bans
In 2006 several states introduced bills to ban abortions
US supreme court will decide the future of abortions
Hospitals maintained by Roman Catholics forbid abortion & sterilization

Incidence of Abortions
In 2006 there were 846,181 abortions Most are unmarried Caucasian women
b/t 20-29 years

Nurses Right
Association of Women’s Health, Obstetric & Neonatal Nurses (AWHONN, 200) supports a nurse’s right to chose to participate or not in abortion procedures in keeping with his or her “personal, moral, ethical, or religious beliefs.
Nurse have a professional obligation to inform their employers at time of employment of attitudes & beliefs that may interfere with job function