4 chambers Blood vessels Valves Path of oxygenated and deoxygenated blood When drawing the left...
-
Upload
bernard-jasper-carpenter -
Category
Documents
-
view
221 -
download
1
Transcript of 4 chambers Blood vessels Valves Path of oxygenated and deoxygenated blood When drawing the left...
Drawing must include:
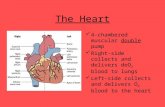
4 chambers Blood vessels Valves Path of oxygenated and deoxygenated blood When drawing the left side of the heart should
be on the right side of the drawing. This is as if you were looking at a heart in a body or a tray.
Show wall thicknesses – left side should be thicker
See page 158 in text, it is better than the pic in the ppt
Chambers
Atria – Thin walled, upper chambers that receive slow moving blood from body or lungs
Ventricles – Thick walled, lower chambers that receive blood from the atria and pump it to the body/lungs
The right side of the heart is responsible for pulmonary circulation. The heart sends blood to lungs for gas exchange.
The left side of the heart is referred to as systemic circulation. Blood leaves the heart via the aorta and branches of the aorta carry blood to organs and tissues.
Valves
All valves ensure that blood flows in a single direction and prevent the backflow of blood.
Atrioventricular (AV) valves (are between the atria and ventricles on the left and right sides. These open to permit blood flow from atria to ventricles. Prevents backflow of blood into atria Right AV valve AKA tricuspid valve Left AV valve AKA bicuspid or mitral valve
Semilunar valves separate ventricles and arteries and prevent blood in the arteries from going back into ventricles Right semilunar valve AKA pulmonary valve
or pulmonary semilunar valve Left semilunar valve AKA aortic valve or
aortic semilunar valve
There are no valves where blood enters the atria. Why?
Vena cava and all veins have valves to prevent backflow
Atrial systole does not generate much pressure (note the thinner walls) because blood only need enter the ventricles below.
Heart valve replacement
Mechanical -- made of man-made materials, such as cloth, metal (stainless steel or titanium), or ceramic. These valves last the longest, but you will need to take blood-thinning medicine, such as warfarin (Coumadin) or aspirin, for the rest of your life.
Biological -- made of human or animal tissue. These valves last 12 - 15 years, but you may not need to take blood thinners for life.
Biological Valves
Xenograft - valve made from animal tissue
Allograft/homograft – valve taken from human tissue of a donated heart.
Autograft - a patient's own tissue can be used for valve replacement
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC483933/?page=1 Autograft done in children.
6.2.3 Action of HeartTo do!
Be able to describe the circulation of blood along both the pulmonary and the systemic circuits.
See pages 158-160 for a description of this but be able to put in into your own words!
Did you ever ride body wars at EPCOT? It takes you on this journey…..
6.2.2 The heart needs blood too!
The heart is a muscle which requires a blood supply.
Coronary arteries supply the heart with oxygen and nutrients.
The picture shows narrowing of the coronary arteries due to plaques of cholesterol and dead cells. The artery can be as much as 70% blocked before symptoms occur.
Symptoms include angina, cramp-like pains in the chest.
If plaque buildup causes artery wall to split, bleeding occurs and a clot may form. The clot may block the artery and starve the tissue of oxygen causing a myocardial infarction (heart attack) http://www.healthyheart.nhs.uk/heart_works/heart01.shtml
H.5.1 Cardiac Cycle
Cardiac cycle is all heart events from the beginning of one heartbeat to the beginning of the next heartbeat
The frequency of the cardiac cycle is your heart rate (beats per minute)
Electrical signal causes muscle fibers of the heart chamber to contract. This squeezes blood from that chamber and it leaves through any opening. This is referred to the systole .
When the chamber is relaxed this is called diastole Both atria contract at the same time and both
ventricles contract at the same time.
Heart Sounds
Lub dub lub dub lub dub…. Each lub dub is one cardiac cycle.
Sounds are the sounds of valves closing “lub” is the sound of the AV valves closing “dub” is the sound of the semilunar valves
closing A heart murmur occurs when blood leaks
back past the valves (backflow) and makes a swishing sound
See page 620 for a sample of the timing of the cardiac cycle.
H.5.2 Pressure data analysis
This is explained on pages 621 – 622 of your book.
Basically you are comparing pressures in chambers in 3 situations: When both chambers are in diastole (relaxed) When the atrium is in systole (contracted)
and the ventricle is in diastole (relaxed) When the atrium is in diastole (relaxed) and
the ventricle is in systole (contracted)
Both chambers in diastole
Since both chambers are relaxed the pressure is low in both. The left AV valve is open.
Blood is entering atrium from pulmonary veins and blood may be passively entering the ventricle from the atria
Pressure in the aorta is high (ventricle has just completed a contraction sending blood to the aorta) so the semilunar valve is closed
Atrium in systole/Ventricle in diastole
Contractions of atria are not very strong so pressure produced is not very high.
Recall that most blood in the atrium passed passively into the ventricle
Any blood remaining in the atrium will be forced into the ventricle
Atrium systole/Ventricle diastole
As the muscular walls of the ventricle contract, pressure in the ventricle begins to increase. This causes the Left AV valve to close (lub)
The aortic semilunar valve is still closed so pressure builds even further.
When pressure in ventricle is greater that pressure in aorta the aortic semilunar valve opens allowing blood to flow into the aorta
As contraction finishes, pressure in ventricle falls and higher pressure in the aorta causes the aortic semilunar valve to close (dub)
Repeat the cycle again….
6.2.4 Regulation of heartbeat
Myogenic muscle contraction - Cardiac muscle contracts and relaxes without nervous system control
Contractions must be timed for heartbeat to be useful
Pacemaker – sinoatrial (SA) node (found in right atrium) sends an electrical signal to trigger contraction of both atria
Atrioventricular (AV) node (also in right atrium) receives a signal from the SA node and sends a signal to ventricles for contraction
If exercising, heart needs to beat faster to remove carbon dioxide and obtain oxygen
The chemoreceptors of the medulla (part of brainstem) senses an increase in carbon dioxide level of blood (and a lowering of blood pH) and sends a message via the cardiac nerve to increase heart rate
SA node receives signal and increase rate of contraction
As carbon dioxide levels fall the medulla senses this and sends a message via the vagus nerve to the SA node. Heart rate slows
The increase in heart rate due to exercise is a result of actions of the autonomic nervous system. Antagonistic nerves initiate opposite responses
Chemicals such as adrenaline also stimulate the SA node to cause heart to beat faster.
6.2.5 Blood Vessels
Arteries – carry blood away from heart (blood that has not yet reached a capillary)
Have thick muscular walls that can constrict and dilate to regulate blood pressure
Carry blood at high pressure due to their proximity to heart
Branch to form arterioles which lead to capillary beds
Capillaries – beds of capillaries are found penetrating all tissues.
Pressure in these beds is low Capillaries are a single cell thick to allow
diffusion of molecules between tissues and blood
1 blood cell fits in a capillary at a time!
As capillaries leave tissues they merge to form venules which merge to form veins.
Blood in veins is very low pressure so veins have valves to ensure that blood flows through the veins in one direction
Because blood is low pressure, walls of veins are thin
6.2.6 Blood Components
Plasma – 55% of blood volume. Contains salts, proteins, cells, nutrients, gases, wastes
Leukocytes – white blood cells (immune system)
Erythrocytes – red blood cells(carry oxygen)
Thrombocytes – platelets (clotting)
6.2.7 Materials transported by blood
Nutrients – glucose, amino acids, fatty acids…. Gases – oxygen and carbon dioxide (CO2 is
dissolved in plasma, O2 is carried by RBC’s) Hormones – produced by endocrine gland and
carried to a target cell Antibodies – protein molecules involved in
immunity Urea – waste product of protein metabolism
(protein amino acid ammonia urea kidney removes)
Heat – blood carries heat to surface of body
11.1.1 Blood Clotting
Blood contains two clotting proteins, fibrinogen and prothrombin
Blood also contains platelets which are fragments of large cells made in the bone marrow. They have no nucleus and live only 8-10 days.
If a vessel is damaged the vessels releases a chemical which causes platelets to collect in that area and form a platelet plug.
The damaged tissue and platelet plug release chemicals called clotting factors that convert prothrombin to thrombin.
Thrombin is an enzyme that catalyzes the transformation of fibrinogen to fibrin (an insoluble fibrous protein)
Fibrin forms a mesh over the platelet plug and as cells and debris get caught in the mesh the blood flow will cease
Damaged vessel releases
chemical causing platelets to adhere to
wounded area.
Damaged tissue and platelets released
clotting factors
H.5.4 Athersclerosis and coronary thrombosis
Athersclerosis – build up of lipids, cholesterol, cell debris and calcium, collectively called plaque.
The plaque builds up on the artery lining (endothelium) makes arteries less flexible and reduces the diameter
Less blood is carried and tissues served by that artery get less oxygen
Clots may form then break away, blocking other arteries
H.5.4 and review of 6.2.2
The heart has 3 coronary arteries that supply it with blood
If a coronary artery is blocked the heart may not get enough oxygen.
Coronary thrombosis (heart attack/myocardial infarction) is blockage of a coronary artery
Symptoms are chest pain (extending into left arm) , constricting sensation around throat, breathing difficulties, dizziness, fainting.
H.5.5 Coronary disease
Coronary heart disease (CHD) refers to plaque build up over time and its associated problems
Risk factors may be related to age, gender, heredity, and race. These of course cannot be controlled.
Risk factors that can be controlled are blood cholesterol level, smoking, high blood pressure, lack of exercise, obesity, stress, diabetes
Many of the risk factors overlap http://
www.webmd.com/heart-disease/risk-factors-heart-disease Check this out!